- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Risk of Stroke doubles in patients of Inflammatory Myopathy
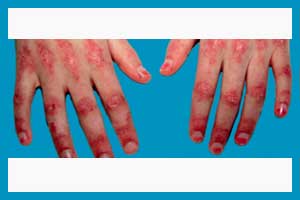
The patients with idiopathic inflammatory myopathies (IIM) are at double the risk for both ischemic (IS) and hemorrhagic stroke (HS) as compared to the general populations, shows findings from a Swedish population-based cohort study published in the journal Arthritis Care & Research.
John Svensson, Karolinska University Hospital, Stockholm, and colleagues conducted the study to analyze the occurrence of ischemic and hemorrhagic stroke among patients with IIM vs general population, and to determine variances based on sex, age, sub-diagnoses and time since initial diagnosis.
Idiopathic inflammatory myopathies are rare chronic rheumatic diseases mainly affecting skeletal muscle, causing weakness and low endurance. This group of diseases consists of dermatomyositis, polymyositis, and sporadic inclusion body myositis. The prognosis for these disorders has improved, but morbidity and mortality remain increased, with cardiovascular disease being the major cause of death.
Also Read: Statin exposure linked to idiopathic inflammatory myositis
For the study, the researchers conducted a population-based cohort study using data from the Swedish National Patient Register. The register includes all nonprimary outpatient visits from 2001, and all hospitalizations from 1987, for all residents of Sweden. Members of the general population were randomly selected from the Total Population Register.
It included 663 patients with newly diagnosed IIM and 6,673 individuals from the general population. Each member of the study population was followed prospectively until either death, emigration, first incident of stroke or December 2013.
Key Findings:
- There were 34 strokes recorded among patients with IIM, and 663 among the members of the general population.
- Increased risks for both ischemic and hemorrhagic stroke were seen among patients with IIM, even as few hemorrhagic-stroke events were reported. This association remained elevated after adjusting for the competing risk for death.
- For ischemic stroke, the rate difference was highest among patients aged 68 years or older.
- Hemorrhagic stroke was highest in the patients aged less than 56 years.
- Risk factors for stroke among patients included hypertension in 15%, diabetes and atrial fibrillation each in 5%, and congestive heart failure in 4%.
- The strokes occurred earlier among patients than controls, at age 66 versus 72.
The authors noted that inflammatory markers such as C-reactive protein have been associated with stroke risk in other rheumatic diseases including rheumatoid arthritis and lupus. However, the primary inflammatory marker utilized in clinical practice for the inflammatory myopathies is creatinine kinase, "and we know very little of its role in the pathogenesis of cardiovascular disease, including stroke," they wrote.
"Our findings indicate that the risk of both IS and HS is increased in individuals with IIM but it should be kept in mind that stroke is a rare event. Focus on prevention should be directed towards groups with the highest absolute risk, especially older patients," concluded the authors.
For more information log on to https://doi.org/10.1002/acr.23702

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd