- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Pneumatic retinopexy offers better results in retinal detachment
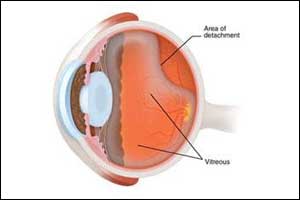
Canada: Pneumatic retinopexy (PnR), a minimally invasive treatment for retinal detachment, offers patients less distortion, sharper vision, and reduced side-effects as compared to pars plana vitrectomy (PPV), a new study finds.
Findings of the randomized controlled trial, published in the journal Ophthalmology demonstrates that PnR should be considered the first line treatment for RRD in patients fulfilling PIVOT recruitment criteria.
The optimal surgical intervention to repair certain common configurations of uncomplicated rhegmatogenous retinal detachment (RRD) is unknown.
Rajeev H. Muni, a vitreoretinal surgeon at St. Michael's Hospital in Toronto, Canada, and colleagues conducted the study to compare outcomes of PnR versus PPV for the management of primary RRD.
Also Read: How to manage pain following Vitrectomy for Retinal Detachment.
"The most commonly offered treatment for a retinal detachment in North America is an operating room surgery called a vitrectomy. The results of this study clearly demonstrate that many retinal detachments will have better results for patients with an alternative minimally invasive office procedure," said Dr. Muni.
"Although the better vision with the minimally invasive treatment (called pneumatic retinopexy, or PnR) is the most important finding of the study -- and it should change how most retina specialists treat simple retinal detachments -- we cannot ignore that PnR is also significantly less expensive to perform than vitrectomy (PPV), and offers significant hope to patients with retinal detachments in developing countries who would otherwise not be able to access care," said Dr. Muni.
"There are many countries where patients simply don't get treated in time because they can't afford it. There are places where people with a detached retina just go blind."
The trial recruited 176 patients who were randomly assigned to either PPV or PnR following their diagnosis of retinal detachment. The primary outcome being researched was visual acuity one year after treatment, as well as a metamorphopsia score for visual distortion, and anatomical success.
Also Read: Retinal detachment increases with increasing degree of myopia, Study finds
Key Findings:
- Patients who underwent PnR scored an average of 4.9 letters better on a standardized visual acuity test compared to those who had PPV, and had less visual distortion.
- A greater proportion of patients who had PnR achieved driving vision (20/40) in the affected eye (90.3 percent vs 75.3 percent).
- Although patients who had PPV treatment did have higher rates of primary anatomical success (93.2 percent versus 80.8 percent), patients who failed PnR still had very good visual outcomes, with secondary anatomical success being virtually identical between the groups.
- Patients in the PnR group also reported quicker recoveries and better quality of life in the six months after being treated.
Dr. Paul E. Tornambe, past president of the American Society of Retina Specialists, congratulated the research team "for completing a well-conceived and well-done" prospective randomized clinical trial.
"It is rare to prove a procedure (in this case PnR) not only results in better vision, is less invasive, restores the anatomy of the eye to its pre-detachment state, and avoids the operating room, but also costs significantly less than the more commonly used operation," said Dr. Tornambe.
The trial was the first to demonstrate that PnR can minimize visual distortion following retinal detachment repair and potentially avoid the so-called "Picasso effect," which causes some patients to suffer significant impairments to their vision, highlighted Dr. Muni.
"It can be debilitating, patients can read the letters on the eye chart, but everything is warped," Dr. Muni said. "Many people end up learning to completely ignore the involved eye. The issue of distortion is very important for patients, and the fact that it can be minimized with PnR is likely related to the better quality of retinal reattachment obtained with the procedure."
"PnR should be considered the first line treatment for RRD in patients fulfilling PIVOT recruitment criteria. PnR offers superior visual acuity, less vertical metamorphopsia, and reduced morbidity when compared to PPV," concluded the authors.
For further reference log on to https://doi.org/10.1016/j.ophtha.2018.11.014

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd