- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Methotrexate ineffective in maintaining steroid-free remission in Ulcerative Colitis
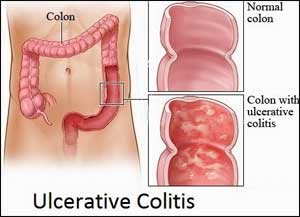
Methotrexate was not found more effective than placebo in maintaining steroid-free response or remission in ulcerative colitis, according to the findings of a trial published in the journal Gastroenterology.
Hans Herfarth and his associates conducted a trial to assess the efficacy of parenteral methotrexate in maintaining steroid-free response or remission in patients with ulcerative colitis(UC) following induction therapy with methotrexate and steroids.
The duration of the trial performed by the researchers was of 48 weeks. The study comprised a 16-week open-label methotrexate induction period followed by a 32-week double-blind placebo-controlled maintenance period. Patients were given subcutaneous methotrexate (25 mg/week) and a 12-week steroid taper.
At week 16, steroid-free responders were randomly assigned to groups that either continued methotrexate (25 mg/week, n=44) or were given placebo (n=40) until week 48. The authors compared the efficacy of treatment by analyzing the proportion of patients who remained relapse-free and were in remission at week 48 without the use of steroids or other medications to control disease activity.
Key findings:
- Ninety-one patients (51%) achieved a response at week 16, and 84 patients were included in the maintenance period study.
- During this period, 60% of patients in the placebo group (24/40) and 66% in the methotrexate group (29/44) had a relapse of UC.
- At week 48, 30% of patients in the placebo group (12/40) and 27% of patients in the methotrexate group (12/44) were in steroid-free clinical remission without the need for additional therapies.
- No new safety signals for methotrexate were detected.
Read Also: FDA approves first oral medication for Ulcerative Colitis
“Treatment options for active ulcerative colitis include thiopurines and biologics, but these drugs are expensive and come with significant adverse side effects. Previous studies of methotrexate that showed efficacy were uncontrolled, and a previous randomized trial done in France did show higher clinical remission rates with methotrexate versus placebo, but there was no maintenance phase to the study.” the authors write.
The commonly observed adverse effect was nausea which was reported in 20% of participants.
According to the authors, Methotrexate is not safe for those who are contemplating pregnancy or have risk factors for liver disease. However, it is cost-effective and the authors suggest that its appropriate role is to help with the induction of active disease and provide a bridge to another agent for maintenance therapy.
For more reference log on to https://doi.org/10.1053/j.gastro.2018.06.046

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd