- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Gout not primarily caused by diet: BMJ
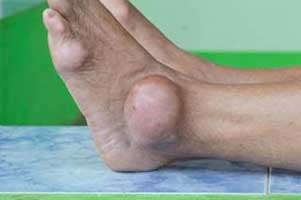
Genes are the main culprit behind the development of high serum (blood) urate levels that often precede gout, according to a new evidence published in The BMJ.
For centuries, diet has been seen as a risk factor for the development of gout. Recent studies suggest that certain foods (eg. meat, shellfish, alcohol, and sugary soft drinks) are associated with a higher risk of gout, while others (eg. fruit, vegetables, low-fat dairy products, and coffee) with reduced serum urate levels.
Studies also show that genetic factors play an important role. For example, the heritability of coffee consumption is estimated to be between 36% to 58%, alcohol consumption to be between 43% to 53%, and sugar-sweetened beverage consumption to be 48%. Genome-wide association studies have identified genetic associations with coffee and alcohol consumption habits.
Read Also: Quarterly Canakinumab reduces risk for gout Flares-Trial Report
The researchers conducted a study to have a better understanding of how both diet and genes might influence the development of gout. A team of researchers based in New Zealand analyzed dietary survey data for 8,414 men and 8,346 women of European ancestry from five US cohort studies.
The study participants were aged over 18 without kidney disease or gout and were not taking urate-lowering or diuretic drugs. Blood urate measurements and genetic profiles were recorded. Factors that could have affected the results, such as sex, age, body mass index, daily calorie intake, education, exercise levels, and smoking status, were also taken into account.
Dietary analysis revealed seven foods associated with raised urate levels (beer, liquor, wine, potato, poultry, soft drinks, and meat) and eight foods associated with reduced urate levels (eggs, peanuts, cold cereal, skimmed milk, cheese, brown bread, margarine, and non-citrus fruits). However, each of these foods explained less than 1% of the variation in urate levels.
Similarly, three diet scores, based on healthy diet guidelines, were also associated with lowered urate levels, while a fourth, based on a diet high in unhealthy foods, was associated with increased urate levels. Again, however, each of these diet scores explained very little (less than 0.3%) variance in urate levels.
Read Also: Gout Doubles risk of Atrial Fibrillation in elderly
In contrast, genetic analysis revealed that common genetic factors explained almost a quarter (23.9%) of variation in urate levels.
According to the authors, the study challenges widely held community perceptions that hyperuricemia is primarily caused by diet, showing for the first time that genetic variants have a much greater contribution to hyperuricemia than dietary exposure.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd