- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Double artery grafts better than single in CABG: ESC 2018
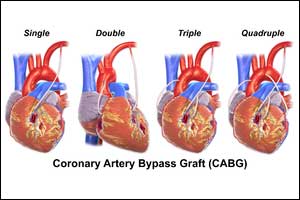
A 10-year follow-up from Arterial Revascularisation Trial (ART) has revealed that the patients receiving two arterial grafts in performing coronary artery bypass graft surgery (CABG) had better outcomes as compared to those receiving a combination of artery and veins.
The results were presented at the European Society of Cardiology (ESC) Congress 2018.
Coronary artery bypass graft surgery is indicated in patients with angina and advanced coronary artery disease. With about one million operations per year globally, it is one of the most common major surgical procedures undertaken worldwide. Establishing the best methods for CABG is, therefore, a key element of the successful management of patients with advanced coronary artery disease, who have narrowed coronary arteries and are at higher risk of limited exercise capacity due to angina, myocardial infarction, and death.
But because many participants were treated off-protocol in the so-called Arterial Revascularization Trial (ART), the definitive answer remains in doubt.
The trial enrolled patients from June 2004 through December 2007 from 28 cardiac surgery centers in the United Kingdom, Poland, Australia, Brazil, India, Italy, and Austria. The researchers randomized 3,102 patients – 1,554 to a single thoracic artery and 1,548 to a double thoracic artery procedure. Taggart said the patients were well-treated medically with 89% on statins, 81% on aspirin, 73% on angiotensin inhibitors and 74% on beta blockers.
Also Read: Radial-Artery grafts lead to improved outcomes of CABG
Key Findings:
- In the primary endpoint of the study (10-year mortality), 329 CABG patients who were treated randomized to the single arterial graft died during the study period compared with 315 patients who died who were originally assigned to receive two arterial grafts (HR 0.96, 95% CI 0.82-1.12).
- There was also no significant difference between groups for the composite of death, myocardial infarct, or stroke at 10 years.
- In the end, 14% of patients randomized to receive two thoracic (mammary) arteries actually received just one artery graft, and 22% of the patients assigned to receive a single arterial graft actually got two – most often the thoracic artery plus a radial artery.
- In his as-treated exploratory analysis, patients who received any two arterial grafts appeared to have a lower mortality (HR 0.81, 95% CI 0.68-0.95) and a lower composite of death, MI, or stroke (HR 0.80, 95% CI 0.69-0.93) compared to those who received a single arterial graft.
The results were confounded because more than one-third of patients received a treatment opposite to the one assigned," said David Taggart, the University of Oxford in the United Kingdom, in his presentation at ESC.
He also said the trial's results may have also been skewed because some surgeons involved in the trial did not have the expertise required to perform the dual thoracic artery CABG procedure. "Surgeons tend to exaggerate their experience," he said.
Among surgeons who had completed fewer than 50 operations before entering the trial, the mortality and composite outcomes were not significantly different between the single and double graft arms. But among surgeons completing more than 50 procedures, outcomes were significantly in favor of the dual artery treatment. He noted that one surgeon – who completed 416 procedures in the trial – had a crossover rate of less than 1%.
"I think that if everyone had done the procedure to the same extent as this surgeon then we would have had a very substantial positive result," Taggart said. "Surgeon experience appears to be a crucial factor for outcomes with bilateral internal thoracic grafts," he said.
Indeed, Taggart said there were populations that would not be candidates for the dual artery surgery. "I would avoid using dual artery CABG in patients who are severely obese, or who have diabetes. These patients have a higher risk of internal infection. But if you take the 80% of patients who are not morbidly obese, without diabetes, you can harvest these arteries without problems."

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd