- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Just IN: WHO recommends 7-10 day bladder catheterisation for obstetric, Check out details
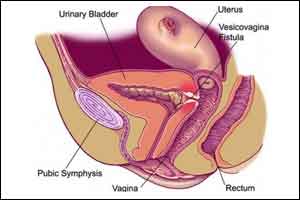
The WHO has issued a new guideline recommending a 7 10 day period of bladder catheterisation for an obstetric complication more common in South Asia and sub-Saharan Africa.
The World Health Organisation (WHO) recommendation on the number of days of bladder catheterisation following surgical repair is for simple obstetric urinary fistula.
Currentl,y the length of catheterisation is not standard and ranges from 5 to 42 days.
"The new guidance recommends a 7 10 day period of bladder catheterisation to allow complete healing," the global health body said.
Obstetric fistula is an abnormal opening between a woman's genital tract and her urinary tract or rectum.
When the mother's pelvis is too narrow or the baby is too large or in an abnormal position, labour can last for several days and often results in the death of the baby or the mother.
If the mother survives, she could develop a fistula. She may be unable to control her rectal or urinary functions.
"Longer periods of catheterisation can be inconvenient for the woman, her family and care providers as it is associated with more discomfort and inconvenience.
"It also increases the risk of infection and erosion related to catheterisation, requires more intensive nursing care and costs more per patient," the WHO said.
Obstetric fistula occurs primarily in sub-Saharan Africa (1.6 cases per 1,000 women) and South Asia (1.2 cases per 1,000 women).
Mostly it can be repaired surgically and catheterisation is important to allow tension-free healing of the surgical scar.
"As part of the WHO's normative work on supporting evidence-informed policies and practices, the Department of Reproductive Health and Research has produced a new guideline that defines the length of time required for effective catheterisation after the surgical repair of simple obstetric urinary fistula as a period of 7 10 days," the WHO said.
The global health body said that it is an intervention that can be implemented by any appropriately trained surgeon, including one with less experience, and it has direct health and cost implications in low-and-middle-income countries.
Shorter periods of post-operative bladder catheterisation have been tested in simple cases of obstetric fistula and shown to be effective in allowing complete healing with improved patient comfort and potentially lower risks of catheter-related urinary tract infections, it said.
The WHO said this, in turn, means less intensive nursing care is required, shorter hospital stays and thus reduced costs for the health system.
"With shorter stays in the hospital it should be possible to increase the number of fistula patients who could receive treatment using the existing facilities," it said. TDS ASK ASK
Important links to this guideline:

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd