- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Diabetic Retinopathy Associated with Higher Risk of Depression : JAMA Study
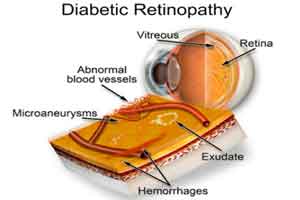
In a study published online by JAMA Ophthalmology, Gwyneth Rees, Ph.D., of the University of Melbourne, Australia, and colleagues examined the association between severity of diabetic retinopathy and diabetic macular edema with symptoms of depression and anxiety in adults with diabetes.
Diabetic retinopathy (DR) is a common micro vascular complication of diabetes. It is a progressive eye disease that is characterized by an asymptomatic non-proliferative stage (NPDR) and symptomatic proliferative stage (PDR). The PDR stage, together with diabetic macular edema (DME), which can develop at any stage, are the primary causes of vision loss in people with diabetes. Research is needed to clarify inconsistent findings regarding the association between diabetes-related eye complications and psychological well-being.
This study included 519 participants with a median duration of diabetes of 13 years. Patients underwent a comprehensive eye examination in which images were obtained and graded for the presence and severity of DR and DME. Visual acuity was also assessed. Patients were screened for symptoms of depression and anxiety.
Eighty individuals (15 percent) screened positive for depressive symptoms and 118 persons (23 percent) screened positive for symptoms of anxiety. Severe NPDR/PDR was independently associated with greater depressive symptoms after controlling for various factors. A history of depression or anxiety accounted for 61 percent of the unique variance in depressive symptoms, and severe NPDR or PDR contributed to 19 percent of the total explained variance of depressive symptoms. Diabetic macular edema was not associated with depressive symptoms. No association between DR and symptoms of anxiety was identified.
“The findings of our study demonstrate that severe NPDR or PDR and moderate or severe vision impairment, but not DME, were independent risk factors for depressive symptoms in people with diabetes,” the authors write. “The severity and progression of DR may be a useful indicator to prompt assessment of psychological well-being, particularly in individuals with other risk factors.”
The researchers note that further work is required to replicate these findings and determine the clinical significance of the association.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd