- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Vertebroplasty ineffective for reducing vertebral fracture pain, Says ASBMR
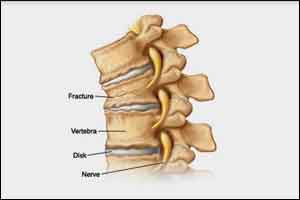
Vertebral augmentation is among the current standards of care for pain reduction in patients with vertebral fractures (VF). Despite this, there is a lack of consensus on the safety and efficacy of percutaneous vertebroplasty and kyphoplasty that raises questions on what basis clinicians should choose one therapy over another.
The American Society for Bone and Mineral Research (ASBMR) formed a Task Force to address key questions on the efficacy and safety of vertebral augmentation and other nonpharmacological approaches for the treatment of pain after VF.
Findings and recommendation of the Task Force, published in the Journal of Bone and Mineral Research, does not support the routine use of vertebral augmentation for pain relief after vertebral fracture.
The most common vertebral augmentation procedures are percutaneous vertebroplasty that involves an injection of medical-grade cement to fuse the bone and balloon kyphoplasty wherein a balloon is used to lift the compressed area of the spine before cement is inserted.
The review found that vertebroplasty did not provide significantly better pain control than placebo in five randomized placebo-controlled trials.
Meanwhile, there was weak evidence of the benefit of kyphoplasty in one clinical trial of this procedure versus nonsurgical management, which had no placebo arm.
Key Findings and Recommendations:
- For patients with acutely painful VF, percutaneous vertebroplasty provides no demonstrable clinically significant benefit over placebo. Results did not differ according to the duration of pain.
- There is also insufficient evidence to support kyphoplasty over nonsurgical management, percutaneous vertebroplasty, vertebral body stenting, or KIVA.
- There is limited evidence to determine the risk of incident VF or serious adverse effects (AE) related to either percutaneous vertebroplasty or kyphoplasty. No recommendation can be made about harms, but they cannot be excluded.
- For patients with painful VF, it is unclear whether spinal bracing improves physical function, disability, or quality of life. Exercise may improve mobility and may reduce pain and fear of falling but does not reduce falls or fractures in individuals with VF.
- General and intervention‐specific research recommendations stress the need to reduce study bias and address methodological flaws in study design and data collection. This includes the need for larger sample sizes, the inclusion of placebo control, more data on serious AE, and more research on nonpharmacologic interventions.
- Routine use of vertebral augmentation is not supported by current evidence. When it is offered, patients should be fully informed about the evidence.
- Anti‐osteoporotic medications reduce the risk of subsequent vertebral fractures by 40–70%.
"For those unfortunate patients who have suffered a vertebral fracture, the message of the Task Force is clear: vertebroplasty does not work to relieve pain from the fracture, and kyphoplasty should generally only be done in the context of a placebo-controlled clinical trial, " ASBMR President Bart L. Clarke, and Sundeep Khosla, MD, both from the Mayo Clinic College of Medicine, Rochester, Minnesota, wrote in an accompanying editorial.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd