- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Vasa previa, a potentially tragic complication: grossly under appreciated
Vasa previa is a rare condition in obstetrics, if undiagnosed, may prove to be fetal to the fetus. Recently the author came across with a case where the condition was diagnosed by chance while performing artificial rupture of membrane. Timely intervention saved the baby. This paper discusses about the etiology, risk factors, mode of diagnosis and management of a case of Vasa Previa. As many studies have confirmed that the condition can be diagnosed accurately and with very high degree of sensitivity and specificity by transvaginal ultrasound using color Doppler, the author is of the opinion that sonologist should specially look for this condition to all women with one or more risk factors while doing 2nd trimester U/S which adds little or no extra time to the duration of the obstetric sonographic examination. This will be of enormous help to avoid tragic complication of neonatal mortality and morbidity associated with Vasa Previa.
Case report
A 34 years-year-old, unbooked multigravid (p3+0) was admitted in early labor at our hospital. She was from a rural area of Haryana and had her antenatal follow up by a general physician. As per her LMP she was at 36and ½ wks gestation. Her U/S was done once at 30weeks gestation. Ultrasound reported a single viable fetus in cephalic presentation with normal growth parameters with heart beats 134/ minute. Expected fetal weight was2000 gm +/- 150 gm, AFI was 9.2cm; placenta was low lying at the anterior wall and away from the os.
All of her previous deliveries were normal. Rest of her medical and surgical history was unremarkable.
On clinical examination during the process of labour, her FHR and other vital parameters were normal. She was having moderate uterine contraction. Presenting part vertex was engaged. Per vaginal examination revealed 5cm dilated cervical os with well-formed bag of membrane. The vertex felt at ‘0’ station. A distinct pulsation was felt over the bulging bag of membrane which gave us a suspicion of rare possibility of Vasa previa. ARM was abandoned and the patient was taken to OT for further evaluation. A gentle speculum examination made our suspicion stronger. Decision for emergency cesarean section was taken. LSCS was done under spinal anesthesia. A male baby of approximately 36 wks weighing 2.3 kg was delivered in good condition. Placenta was situated in the anterior wall of the uterus. A small lobe of placenta with infarction was found on the lower segment of the posterior wall. A diagnosis of succenturiate placenta with Vasa previa was made. Post LSCS period was uneventful. The patient with the baby was discharged on third post operative day in good condition.
Discussion: Vasa previa is a condition in which the umbilical vessels traverse within the fetal membranes of the lower uterine segment and overlie the cervix. These vessels are at risk of rupture when the membranes get ruptured spontaneously or artificially and result in an acute fetal hemorrhage and death. The largest studies report a prevalence of 1.5–4:10,000.
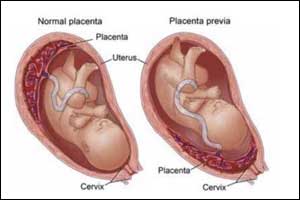
Vasa previa may be due to velamentous cord insertion (Umbilical cord inserting into the membranes of the placenta rather than onto the placental mass) in a single lobe placenta or a succenturiate placenta (accessory lobe of placenta) with the connecting vessels crossing over the os. There are certain pregnancy conditions that may be associated with Vasa previa. These include Pregnancy with assisted reproductive technologies, low lying placenta in the second trimester, Placenta previa, bi-lobed or succenturiate-lobed placenta, Multiple pregnancy (especially mono-chorionic).
It is not very clear why some placentas implant in the lower uterine segment rather than in the fundus in early pregnancy. However it has been postulated that as the pregnancy progresses, the placenta grows preferentially toward the better-vascularized fundus (this is also termed “placental migration” or Trophotropism), whereas the placenta overlying the less-well-vascularized lower uterine segment atrophies. In some cases, this atrophy leaves vessels running through the membranes, unsupported by placental tissue or cord and resulting in Vasa previa. In cases where the atrophy is incomplete, a succenturiate lobe may develop. Literature suggests much higher prevalence of Vasa previa (1:202) in pregnancies conceived following use of assisted reproductive technologies.
Gone are the days when Vasa previa was detected only during rupture of membranes. That was invariably accompanied by vaginal bleeding and fetal distress or death. Wide use of ultrasound, particularly transvaginal u/s using colour Doppler has made it possible to diagnose the condition during the antenatal period with a higher degree of accuracy.
A recent systematic review demonstrated that the accuracy of ultrasound in the prenatal detection of Vasa previa is high when performed transvaginally and combined with color Doppler, with a median prenatal detection rate of 93% and specificity between 99% and 100%. In two prospective studies with a total of 33,795 patients including 11 cases of Vasa previa, second-trimester transvaginal color Doppler detected all cases of Vasa previa, with 100% sensitivity and 99.0%–99.8% specificity.
Diagnostic criteria for Vasa previa using transvaginal ultrasound include the presence of a linear sonolucent area over the internal os of the cervix. Blood flow can be demonstrated through these umbilical vessels with color Doppler. Differential diagnoses include funic presentation and normal cord loop. Thus it may be necessary to attempt to shift the position of the umbilical cord by gently tapping with the ultrasound transducer over the area in question or by adjusting the maternal position and ascertaining that the vessel is not displaced with maternal movement.
Can Vasa previa be diagnosed in labour before it is too late to save the baby? The author feels that it can be possible in normal labour or when the patient is induced for labour. Usually membrane ruptures when the cervix is 3-4cm dilated. One has to keep in mind the condition and be alert about the rare possibility of Vasa previa when pulsating vessels felt running across the bulging membranes. Should Vasa previa be suspected this way, the woman should be transferred immediately to the operating room for a further careful clinical assessment. Should Vasa previa be diagnosed in this setting, an immediate Caesarean section will result in a healthy baby.
If Vasa previa is diagnosed antenatally, cesarean section delivery should be planned before the onset of labor, preferably by 35-36 weeks of gestation to avoid spontaneous rupture of membrane. In such cases early hospitalization and administration of corticosteroids for lung maturity may be needed. Though there is no consensus about the gestational age of delivery, cesarean section delivery at 35–36 weeks’ gestation to avoid the risk of membrane rupture and fetal death has been considered justifiable in most situations. In case of Vas previa bleeding though the safest and quickest form of delivery is usually an immediate cesarean, it is important for the surgeon to be aware of the position of the fetal vessels before surgery to avoid lacerating them when making the uterine incision.
Summary
Looking for umbilical cord insertion in all patients and screening for Vasa previa in patients with risk factors when performing ultrasound scans have made it possible to diagnose Vasa previa in the second and third trimesters. Prenatal diagnosis allows appropriate planning and delivery by cesarean to avoid rupture of fetal vessels and exsanguinations. Health professionals caring for pregnant women must be aware of the risk factors, diagnosis, and management of Vasa previa.
References
- Oyelese KO, et al. Vasa previa: an avoidable obstetric tragedy. Obstet Gynecol Surv. 1999; 54(2):38-45.
- Lee W, et al. Vasa previa: prenatal diagnosis, natural evolution, and clinical outcome. Obstet Gynecol. 2000; 95(4):572-576.
- Catanzarite V, et al. Prenatal sonographic diagnosis of Vasa previa: ultrasound findings and obstetric outcome in ten cases. Ultrasound Obstet Gynecol. 2001; 109-115.
- Monie IW. Velamentous Insertion of the Cord in Early Pregnancy. Am J Obstet Gynecol. 1965; 93:276-281.
- Oyelese Y, et al. Second trimester low-lying placenta and in-vitro fertilization? Exclude Vasa previa. J Matern Fetal Med. 2000; 9(6):370-372.
Dr.S.K.Basu-MD, FICS, FICOG, FARSI is consultant Obstetrician & Gynaecologist at Rural Medical Centre,New Delhi.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd