- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Use of menopausal hormone therapy linked to microscopic colitis
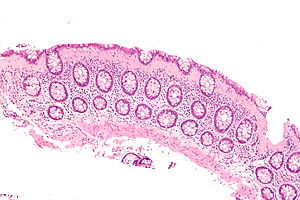
Women using menopausal hormone therapy or oral contraceptives appear to have a higher risk of developing microscopic colitis (MC), according to a new study published in the journal Gastroenterology.
Microscopic colitis is a chronic inflammatory disorder of the colon primarily affecting postmenopausal women.
Kristin E. Burke, Gastroenterology Unit, Massachusetts General Hospital, Boston, Massachusetts, U.S., and colleagues conducted the study to determine the relationship between hormonal determinants, including reproductive and menopausal factors, and risk of MC.
"Microscopic colitis is predominantly a disease of post-menopausal women, so understanding whether and how hormonal factors impact the risk of MC is key to providing insight into its pathogenesis and how it relates to other inflammatory bowel diseases," Dr. Burke told Reuters Health by email.
"Clinicians may add MC to the list of cogent reasons to avoid these classes of medications, particularly menopausal hormone therapy," she added.
The research team collected data from the 121,706 female U.S. nurses in the ongoing Nurses' Health Study (NHS) who have been returning mailed health questionnaires every two years since 1976 and the 116,684 in the ongoing NHS II who have been doing so since 1989.
Key Findings:
- The researchers found 275 cases of MC over more than 5 million person-years through 2014 in NHS and 2015 in NHS II.
- Compared with never-use of menopausal hormone therapy, past or current use was linked with a significantly higher risk for MC (adjusted hazard ratio, 1.95 and 2.64, respectively).
- Longer use was linked with increased risk (P for trend<0.0001) and longer time since discontinuation was linked with decreased risk (P for trend=0.002). The associations did not vary by disease subtype.
- Ever-use of oral contraceptives also was linked with significantly increased microscopic colitis risk.
- No associations of incident MC were found with ages of menarche, first birth, or menopause, or with parity or type of menopause.
Dr. Faten N. Aberra, an associate professor of medicine and a co-director of the Inflammatory Bowel Center at the University of Pennsylvania in Philadelphia, said by email, that, because microscopic colitis disproportionately affects older women, the findings are not very surprising.
"What's new," added Dr. Aberra, who was not involved in the study, "is that current or past use of hormonal replacement therapy (HRT) increased the risk of developing microscopic colitis, although with prior use of hormonal therapy the risk of microscopic colitis decreased the longer the women were off the medication."
"HRT containing estrogen and progesterone increased the risk more than progesterone-only therapies," she said. "Use of oral contraceptive therapy also increased the risk of developing microscopic colitis."
"Microscopic colitis is rare but can be a devastating chronic disease," Dr. Aberra noted. "It appears to have triggers (i.e., nonsteroidal anti-inflammatory drugs (NSAIDs), proton pump inhibitors (PPIs), selective serotonin reuptake inhibitors (SSRIs)), but in many patients, the triggers cannot be clearly identified. HRT may help explain the reason for some cases."
"So think of hormonal replacement therapies as risk factor for microscopic colitis," Dr. Aberra advised. "For patients diagnosed with microscopic colitis on HRT, HRT cessation should be considered in addition to screening for other pharmacologic triggers."
"In 2 large prospective cohort studies, we observed an association between exogenous hormone use and incident microscopic colitis. Further studies are needed to determine the mechanisms underlying these associations," concluded the study authors.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd