- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Unique presentation of SJS in patient treated with TMP-SMX
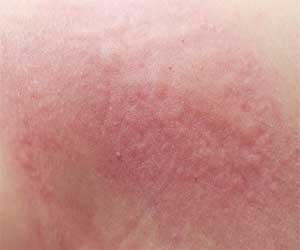
A recent case report published in the American Journal of Case Reports describes a rare presentation of a 27-year-old female patient with Stevens-Johnson syndrome (SJS) involving mucocutaneous desquamation and vaginal pain following re-exposure to trimethoprim-sulfamethoxazole (TMP-SMX). She had a history of polycystic ovary syndrome (PCOS).
Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are causes of rare but life-threatening emergencies characterized by desquamation of the skin and mucosa. As SJS most commonly presents with skin rash followed by mucosal involvement. In this case report, the authors present a case of vulvovaginal lesions as the initial presentation with progression to SJS after re-exposure to the culprit drug.
The patient was presented to the clinical office complaining of dysuria, was diagnosed with a urinary tract infection and was prescribed TMP-SMX. After taking 4 doses of her medication, she presented to the emergency department (ED) complaining of left labial swelling and pain. She was diagnosed with left vulvovaginitis and was told to discontinue TMP-SMX since her urine cultures were negative. Two days later, the patient returned to the ED complaining of worsening vaginal pain and vulvar lesions but was discharged with a sitz bath and supportive care and urged to follow-up at the clinical office. At her follow-up appointment, she was reinitiated on TMP-SMX due to “concerns of vulvar cellulitis with a possible underlying abscess.”
The patient had new lip swelling, periorbital swelling, facial swelling, and formation of thick white plaque on her tongue and mouth after receiving 2 doses of TMP-SMX. She also developed an erythematous papular pruritic rash on her hands, arms, soles of the feet bilaterally and papules were noted on the legs (up to thighs), feet, and abdomen.
The patient also experienced early vesicle formation, skin sloughing, significant erythema and edema in her genital region, a fever of 102°F, plaques on her tongue, and a painful maculopapular skin rash. The patient was diagnosed with SJS and transferred to the burn unit/ICU where she received intravenous immunoglobulin, supportive care, as well as wound care. She was discharged 11 days after being admitted to the hospital.
Interesting features of this patient case included quick onset and development of SJS (6-12 hours vs 6 days to 2 weeks) as well as the unique presentation of the patient (vaginal pain/ mucocutaneous desquamation).
"This report shows that although SJS is a rare diagnosis, providers should consider SJS as a possible differential diagnosis as a cause of vaginal lesion after exposure to drugs,” concluded the authors.
For further reference follow the link: 10.12659/AJCR.912123

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd