- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Topical Tranexamic acid reduces risk of rebleeding in epistaxis
A probable reduction was found in the risk of re-bleeding with the use of either oral or topical tranexamic acid in addition to usual care in adult patients with epistaxis, compared to placebo with usual care, according to a systematic review and meta-analysis published in Cochrane.
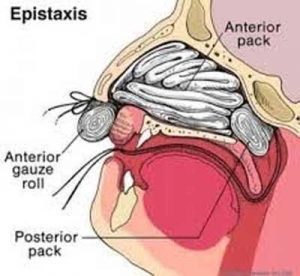
Epistaxis (nosebleed) most commonly affects children and the elderly. The majority of episodes are managed at home with simple measures. In more severe cases medical intervention is required to either cauterize the bleeding vessel or to pack the nose with various materials.
Read Also: Topical Tranexamic acid is more effective than Nasal Packing for Epistaxis
Burton and his associates performed a meta-analysis to determine the effects of tranexamic acid (oral, intravenous or topical) compared with placebo with no additional intervention or any other hemostatic agent in the management of patients with epistaxis.
The investigators extracted the data from existing literature which included randomized controlled trials (RCTs) of tranexamic acid (in addition to usual care) compared with usual care plus placebo, usual care alone or usual care plus any other hemostatic agent, to control epistaxis in adults or children. Six studies met the inclusion criteria.
The primary outcomes were control of epistaxis: re-bleeding (as measured by the proportion of patients re-bleeding within a period of up to 10 days) and significant adverse effects (seizures, thromboembolic events). Secondary outcomes were control of epistaxis as measured by the time to stop initial bleeding (the proportion of patients whose bleeding is controlled within a period of up to 30 minutes) and severity of re-bleeding.
The key analysis included were:
- Three studies measured re-bleeding within 10 days. The researchers found that fewer patients who were given either oral or topical tranexamic acid had further episodes of re-bleeding following an initial nosebleed compared to those treated with usual care.
- The time to stop initial bleeding (control of bleeding within 30 minutes) was measured in four studies. In three studies the proportion of patients whose bleeding stopped within 10 minutes was significantly higher in the group receiving topical tranexamic acid compared to the group receiving a different drug (topical epinephrine and lidocaine or phenylephrine). In the other study, there was no significant difference at 30 minutes when topical tranexamic acid was compared with placebo.
- No studies reported the proportion of patients requiring any further intervention(e.g. repacking, surgery).
- Only one study of oral tranexamic acid reported the proportion of patients requiring a blood transfusion and there was no evidence of a difference between the groups.
Read Also: Epistaxis – Standard Treatment Guidelines
- Length of hospital stay was reported in two studies. One study reported a significantly shorter stay in the oral tranexamic acid group, while the other found no evidence of a difference.
- Five studies mentioned recording "adverse effects". None found any difference between the groups in the occurrence of minor adverse effects(e.g. mild nausea and diarrhea, 'bad taste' of gel).
- In one study patient did develop superficial thrombophlebitis (inflammation and a blood clot in a vein near the surface of the skin) of both legs following discharge, but the study did not report in which treatment group this happened. No serious adverse event was seen in any of the studies.
“Overall, the risk of bias in the six studies was low. We graded the quality of the evidence for the main outcome (control of epistaxis: re-bleeding within 10 days) as moderate, which means that further research is likely to have an important impact on our confidence in the estimate of the effect and is likely to change the estimate, ”write the authors.
For full information log on to https://www.cochrane.org/CD004328/ENT_tranexamic-acid-help-treat-nosebleeds-epistaxis

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd