- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
2018 ACC Expert consensus on Tobacco Cessation
American College of Cardiology (ACC) has released its 2018 Expert Consensus on decision Pathway on Tobacco Cessation Treatment. They have appeared in the Journal of the American College of Cardiology.
Tobacco use, especially cigarette smoking, is a major risk factor for cardiovascular morbidity and mortality and is the leading preventable cause of death worldwide. Comprehensive tobacco cessation treatment is a critical component of the clinical care for individuals with or at risk for cardiovascular diseases. Comprehensive tobacco cessation treatment is a critical component of the clinical care for individuals with or at risk for cardiovascular diseases.
Pathway for Tobacco Cessation Treatment
The figure summarizes the 2018 ACC Expert Consensus Decision Pathway for Tobacco Cessation Treatment
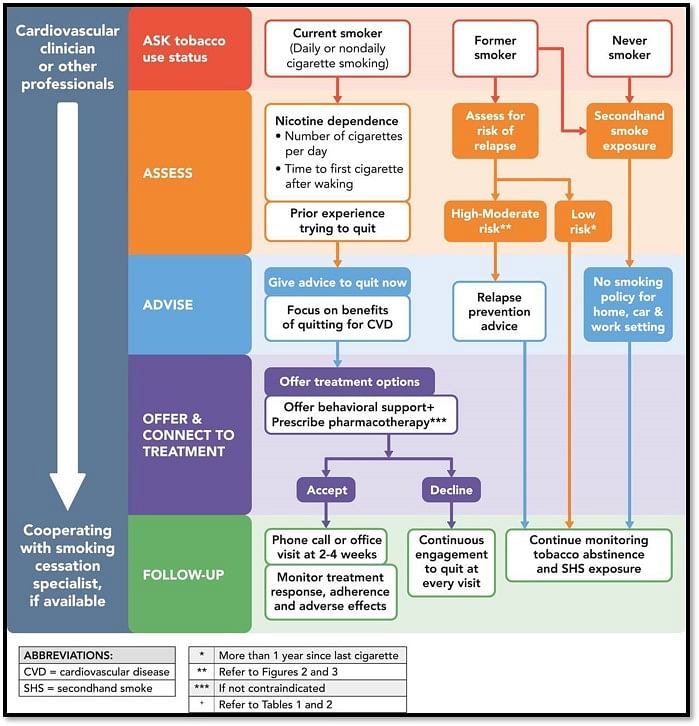 Image Source: JACC
Image Source: JACCQuestions to Assess a Smoker's Degree of Nicotine Dependence
0: 10 or fewer
1: 11–20
2: 21–30
3: ≥ 31
How soon after waking up do you smoke your first cigarette of the day?
0: After 60 minutes
1: 31–60 minutes
2: 6–30 minutes
3: within 5 minutes
Level of nicotine dependence is computed by adding the scores together as follows:
0-2 = low nicotine dependence
3-4 = moderate nicotine dependence
5- 6 = high nicotine dependence
Treatment Algorithm for a Former Smoker
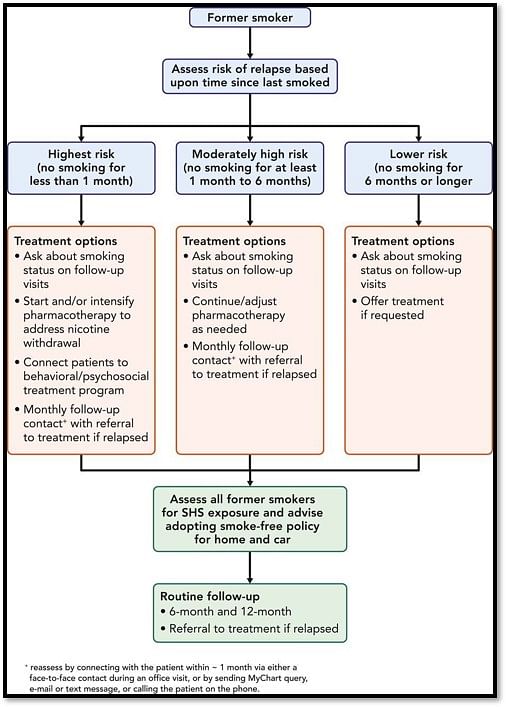 Image Source: JACC
Image Source: JACCPathway for Tobacco Cessation Treatment
A team-based system of care that recognizes cigarette smoking as a chronic relapsing substance use disorder caused by addiction to nicotine has been recommended.

Key points are :
- An estimated 6 million deaths each year are attributable to tobacco use. In particular, cigarette smoking carries the highest risk for cardiovascular disease (CVD) events. Although tobacco use has been in decline over the past several decades, an estimated 30 million people in the United States currently smoke.
- Those who do not smoke but are exposed to second-hand smoke are at a 25-30% increased risk for CVD events, which translates into an estimated 33,000 deaths from heart disease each year. Smoke-free policies have reduced exposure to second-hand smoking in public areas; however, most of the second-hand smoking exposure is in the home. Providers are recommended to assess nonsmoking patients for exposure to second-hand smoke.
- All smokers, regardless of the duration and intensity of smoking, can benefit from smoking cessation. No one is too old to not benefit from quitting. Even those with established CVD can experience health benefits associated with smoking cessation.
- Providers are key to assisting patients who smoke to quit. They should ask all patients about tobacco use, advise smokers to quit, assess a smoker's readiness to quit, and assist smokers to quit. Hospitals are recommended to assess smoking status in all admitted patients, offer treatment to hospitalized smokers, and provide treatment at time of discharge.
- Current evidence suggests the combination of pharmacotherapy (i.e., nicotine replacement, bupropion, and varenicline) with behavioural interventions (i.e., cognitive behaviour therapy, motivational interviewing) are most effective for smoking cessation. Tobacco cessation programs are cost-effective. E-cigarettes may reduce cigarette smoking among current smokers; however, the long-term risk of e-cigarettes is not known. Ultimately, cessation of all combustible tobacco products is recommended.
For further reference log on to :
DOI: 10.1016/j.jacc.2018.10.027

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd