- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Thickened bowel walls observed in ulcerative colitis patients experiencing flares
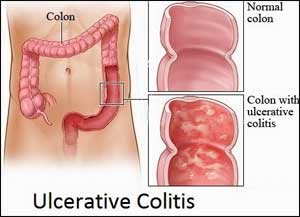
Ultrasound images showed thickening of bowel wall in the vast majority of patients with ulcerative colitis (UC) experiencing clinical flares, reported the researchers.
The TRUST&UC (TRansabdominal UltraSonography of the bowel To monitor disease activity in subjects with Ulcerative Colitis) study was led by Christian Maaser, a gastroenterologist at University Teaching Hospital in Lueneburg. It is a 37-center prospective, observational study of adults undergoing treatment for active UC. An interim analysis of the study was presented at the 2017 United European Gastroenterology Week.
Bowel-wall thickening (BWT) and an array of other sonographic parameters can improve as early as six weeks into a course of treatment for flare, according to Dr. Maaser.
“We found thickening of all three layers (of the bowel). We found mesenteric proliferation of the fat around the bowel, and increased lymph nodes,” Dr. Maaser said. Such ultrasonic evidence shows that UC is in fact not restricted to the mucosa, he added.
For the study, the patients with UC were checked for C-reactive protein, fecal calprotectin and the Simple Colitis Clinical Activity Index (SCCAI). The 176 patients in whom the SCCAI score indicated a flare then underwent ultrasound in the office, performed by the gastroenterologist.
Key Findings:
- Of the 176 patients, ultrasound revealed evidence of BWT in roughy 160 (90%), the change appeared in the sigmoid and descending colon.
- Loss of stratification in the bowel wall (20.6% of patients), mesenteric fibrofatty proliferation (40.0%), and increased color Doppler signal (56.7%), all suggesting increased disease activity.
The patients then began or escalated treatment; some 104 underwent follow-up ultrasound at six and 12 weeks.
After 12 weeks of follow-up:
- Far fewer patients showed BWT in the sigmoid (33.7% of patients vs. 87.5% at baseline; P=0.034) or transverse colon (15.4% vs. 42.3%; P=0.012), loss of haustration (33.7% vs. 54.8%), ascites (2.9% vs. 9.7%), mesenteric lymphadenopathy (14.3% vs. 31.6%), mesenteric fibrofatty proliferation (10% vs. 40%) or increased signal in color Doppler ultrasound.
- Decreased BWT also correlated with lower scores on the SCCAI.
“Color Doppler signal is an ultrasound feature that accurately detects blood flow, and can be optimized to assess small vessel [or] low flow in the wall of the bowel, reflecting the known angiogenesis [and] increased blood vessels that occurs with active inflammation,” said Kerri Novak, MD, a clinical assistant professor of medicine at the University of Calgary, in Alberta, Canada, and Dr. Maaser’s fellow IBUS co-chair.
Dr. Maaser said the team saw similar, significant numbers at the six-week mark. The study recently enrolled its last few patients; Dr. Maaser expects to present final results at this year’s UEG Week in October.
“In our clinical trial, the intestinal ultrasound (IUS) really helps you to decide at a very early time point—at week 6—if the medication actually works or it doesn’t work,” Dr. Maaser said. He added that gastroenterologists unfamiliar with IUS should take the time to watch one or two.
“Increasingly, we recognize that cross-sectional imaging is a robust surrogate for endoscopic healing” in inflammatory bowel disease, Dr. Novak said.
Although cross-sectional imaging data across multiple modalities have shown BWT to be the strongest predictor of disease activity, Dr. Novak said, few studies evaluate such imaging early in the course of therapy.
“In some individuals, early optimization of the medical therapy may further enhance or facilitate robust and durable response to therapy,” Dr. Novak said. “The timing is unclear—is it best to evaluate at six weeks? Eight? Twelve? There is published data to suggest that response at 12 weeks predicts clinical remission at 52 weeks.
“I think only ultrasound is amenable to a study like this, because people are not willing to have MR as frequently,” she added. “This is very important early data to suggest imaging reflects early healing and that BWT is the most important [parameter].”
Calling IUS safe, patient-centered and cost-effective, Dr. Novak predicted that all IBD experts will be trained in the modality within a decade.
“It’s one of the fastest-moving, most robustly compelling areas of IBD care,” she said. “This is the new frontier in gastroenterology.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd