- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Subcutaneous methotrexate outcome in patients with psoriasis: Lancet Study
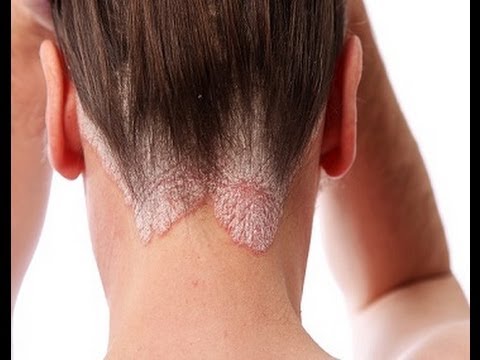
Methotrexate is one of the most commonly used systemic drugs for the treatment of moderate to severe psoriasis; however, high-quality evidence for its use is sparse and limited to use of oral dosing. Authors Richard B Warren el al aimed to assess the effect of an intensified dosing schedule of subcutaneous methotrexate in patients with moderate to severe plaque-type psoriasis. The study entitled An intensified dosing schedule of subcutaneous methotrexate in patients with moderate to severe plaque-type psoriasis (METOP): a 52 week, multicentre, randomised, double-blind, placebo-controlled, phase 3 trial was published in The Lancet, 21 December 2016.
A prospective, multicentre, randomised, double-blind, placebo-controlled, phase 3 trial (METOP) was conducted at 16 sites in Germany, France, the Netherlands, and the UK. Eligible patients were aged 18 years or older, had a diagnosis of chronic plaque psoriasis for at least 6 months before baseline, had currently moderate to severe disease, and were methotrexate treatment-naive. Participants were randomly assigned (3:1), via a computer-generated random number sequence integrated into an electronic data capture system, to receive either methotrexate at a starting dose of 17·5 mg/week or placebo for the first 16 weeks, followed by methotrexate treatment of all patients up to 52 weeks (methotrexate–methotrexate vs placebo–methotrexate groups). Dose escalation to 22·5 mg/week was allowed after 8 weeks of methotrexate treatment if patients had not achieved at least a 50% reduction in baseline Psoriasis Area and Severity Index score (PASI), with corresponding volume increases in placebo injections. Treatment was combined with folic acid 5 mg/week. Group allocation was concealed from participants and investigators from the time of randomisation until an interim database lock at week 16, and was open label from week 16 onwards, with no masking of participants or investigators. The primary efficacy endpoint was a 75% reduction in PASI score (PASI 75) from baseline to week 16.
Between Feb 22, 2013, and May 13, 2015, the authors randomly assigned 120 patients to receive methotrexate (n=91) or placebo (n=29). At week 16, a PASI 75 response was achieved in 37 (41%) patients in the methotrexate group compared with three (10%) patients in the placebo group (relative risk 3·93, 95% CI 1·31–11·81; p=0·0026). Subcutaneous methotrexate was generally well tolerated; no patients died or had serious infections, malignancies, or major adverse cardiovascular events. Serious adverse events were recorded in three (3%) patients who received methotrexate for the full 52 week treatment period.
The reserchers concluded a favourable 52 week risk–benefit profile of subcutaneous methotrexate in patients with psoriasis. The route of administration and the intensified dosing schedule should be considered when methotrexate is used in this patient group
A prospective, multicentre, randomised, double-blind, placebo-controlled, phase 3 trial (METOP) was conducted at 16 sites in Germany, France, the Netherlands, and the UK. Eligible patients were aged 18 years or older, had a diagnosis of chronic plaque psoriasis for at least 6 months before baseline, had currently moderate to severe disease, and were methotrexate treatment-naive. Participants were randomly assigned (3:1), via a computer-generated random number sequence integrated into an electronic data capture system, to receive either methotrexate at a starting dose of 17·5 mg/week or placebo for the first 16 weeks, followed by methotrexate treatment of all patients up to 52 weeks (methotrexate–methotrexate vs placebo–methotrexate groups). Dose escalation to 22·5 mg/week was allowed after 8 weeks of methotrexate treatment if patients had not achieved at least a 50% reduction in baseline Psoriasis Area and Severity Index score (PASI), with corresponding volume increases in placebo injections. Treatment was combined with folic acid 5 mg/week. Group allocation was concealed from participants and investigators from the time of randomisation until an interim database lock at week 16, and was open label from week 16 onwards, with no masking of participants or investigators. The primary efficacy endpoint was a 75% reduction in PASI score (PASI 75) from baseline to week 16.
Between Feb 22, 2013, and May 13, 2015, the authors randomly assigned 120 patients to receive methotrexate (n=91) or placebo (n=29). At week 16, a PASI 75 response was achieved in 37 (41%) patients in the methotrexate group compared with three (10%) patients in the placebo group (relative risk 3·93, 95% CI 1·31–11·81; p=0·0026). Subcutaneous methotrexate was generally well tolerated; no patients died or had serious infections, malignancies, or major adverse cardiovascular events. Serious adverse events were recorded in three (3%) patients who received methotrexate for the full 52 week treatment period.
The reserchers concluded a favourable 52 week risk–benefit profile of subcutaneous methotrexate in patients with psoriasis. The route of administration and the intensified dosing schedule should be considered when methotrexate is used in this patient group
Next Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd