- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Scientists uncover potential mechanism for HPV-Induced skin cancer
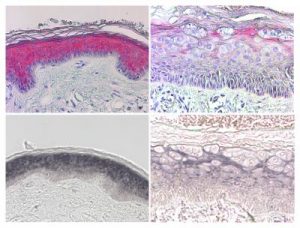
Scientists have identified a molecular pathway by which some types of human papilloma virus (HPV) might increase the risk of skin cancer, particularly in people with the rare genetic disorder epidermodysplasia verruciformis (EV). The novel pathway is described in PLOS Pathogens.
Some HPV types of the genus known as beta-HPV infect skin cells and can increase the risk of non-melanoma skin cancer, especially in people with weakened immune systems or EV. Previous research has suggested that a type of HPV protein called E6 underlies this increased cancer risk, but the molecular mechanisms by which E6 proteins may act are unclear.
To better understand the role of E6 proteins in skin cancer, a team led by Sigrun Smola, professor and chair of the Institute of Virology, Saarland University, Germany, focused on HPV infection in EV patients. EV makes people particularly vulnerable to infection with beta-HPV strains, so the disease provides a useful opportunity to study beta-HPV infection mechanisms.
The research team obtained samples of skin lesions from EV patients; some of these lesions tested positive for infection with HPV8, a type of beta-HPV. Molecular analysis revealed that the HPV8-infected lesions expressed significantly lower levels of microRNA-203, a known regulator of skin cell growth and differentiation. The HPV8-infected lesions also had higher levels of p63, a protein that is regulated by microRNA-203 and has been associated with cancer development.
Lab experiments with human skin cells performed predominantly by Anna Marthaler, PhD, then revealed molecular links between these microRNA-203/p63 effects and HPV8 infection. The results suggested that HPV8’s E6 protein suppresses expression of C/EBPα, a protein that is known to play a key role in curbing the development of sun-induced skin cancer.
Additional analysis showed that C/EBPα directly regulates microRNA-203 and is in turn regulated by the protein p300, a known target of E6 proteins. The researchers also showed that HPV8-infected skin lesions from EV patients had significantly lower levels of C/EBPα and microRNA-203 than did non-lesional skin cells.
Overall, these findings suggest the existence of a previously unknown molecular pathway involving p300, C/EBPα, and microRNA-203 that helps to maintain normal skin cell proliferation and differentiation. HPV8’s E6 protein appears to disturb the normal function of this pathway in EV patients, potentially paving the way for skin cancer.
“Our findings are particularly exciting because we now better understand how beta-HPV infection can contribute to UV-induced skin carcinogenesis,” the authors explain. “This discovery opens new avenues for therapeutic interventions against skin cancer.”
epidermodysplasia verruciformisHPVHuman Papilloma Virusjournal PLoS PathogensPLOS Pathogensskin cancer
Next Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd