- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Research suggests Asian women less likely to receive timely follow-up after abnormal mammogram
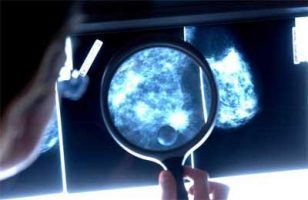
Women with an abnormal mammogram result need follow-up tests to check whether the finding indicates breast cancer, which should be treated at the earliest possible stage. In a recent study, Asian women were less likely to receive appropriate follow-up treatment after an abnormal mammogram compared with White women. Published early online in CANCER, a peer-reviewed journal of the American Cancer Society, the findings point to the need to investigate and address barriers to effective cancer prevention in Asian women.
Many population-based breast cancer studies do not include Asians, and those that do often report them as a single group. To study the relationship between breast cancer screening and outcomes in multiple Asian populations, a team led by Kim Hanh Nguyen, MPH, ScD, and Leah Karliner, MD, MAS, of the University of California, San Francisco examined information from the San Francisco Mammography Registry. Radiology facilities participating in the registry prospectively collect demographic and clinical data from women at the time of breast imaging and at each subsequent imaging visit.
The investigators examined data on 50,970 San Francisco-area women with mammogram results from 2000-2010 that indicated the need for further diagnostic imaging. Among Asian women, Vietnamese and Filipina women had the longest--and Japanese the shortest--median time to follow-up imaging tests (32, 28, and 19 days, respectively) compared with non-Hispanic White women (15 days). The proportion of women receiving follow-up tests at 30 days was lower for Asians than for non-Hispanic Whites (57 percent versus 77 percent), and these disparities persisted at 60 and 90 days for all Asian ethnic groups except Japanese women. Asian women also had a higher rate of no follow-up at one year than non-Hispanic Whites (15 percent versus 10 percent), with Filipinas having the highest percentage of no follow-up among Asian ethnic groups (18 percent).
"The reasons for these long delays may be due to linguistic, cultural and other barriers that affect patient-provider communication for disadvantaged Asian groups," said Dr. Nguyen. "More research attention is needed to understand the specific reasons for these differences."
By 2060 the projected number of US residents who will identify as Asian or Asian with another race will reach 48.6 million, or 11.7 percent of the total population. "Rather than being a monolithic group, Asians are, in fact, very diverse in nationalities, language, immigration history, education, and economic background. Recognizing differences among Asians may help clinicians develop better rapport and communication with their Asian patients, which can improve adherence to screening recommendations," said Dr. Nguyen. "The misconception of the model minority suggesting Asians are doing better than other minorities is insensitive to disparities that exist for Asians and undermines the need to address such disparities."

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd