- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Recurrent hemifacial oedema
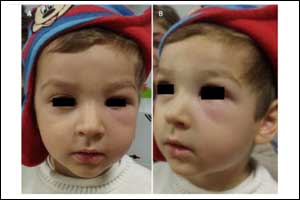
The case of Recurrent hemifacial oedema has been published in BMJ Case Reports.
A 3-year-old boy, with no relevant family/personal history, presented at the emergency department due to recurrent left hemifacial erythematous oedema and feverish peak. The mother reported two similar episodes in the previous months, interpreted as periorbital cellulitis, with resolution with systemic antibiotic and oral corticosteroid. She denied fever, weight loss or other constitutional symptoms.
At examination presented skin paleness; soft, non-tender swelling and erythema of the left periorbital region (Figures 1); shotty, non-tender, well defined, smooth generalised lymphadenopathy (cervical, submaxillary, axillary, inguinal); firm and non-tender splenomegaly palpable 2 cm below the costal margin. Ophthalmological examination and funduscopy were normal.
Laboratory tests revealed a normocytic and normochromic anaemia (haemoglobin of 8.4 g/dL), leucocytosis (28100 WBC/μL) with 77% of lymphocytes, 137.000/μL platelets, normal liver function enzymes and negative serology for Epstein-Barr virus. Peripheral blood smear revealed 44% of blasts; flow cytometry was compatible with B cell acute lymphoblastic leukaemia (ALL). Abdominal ultrasound identified homogeneous hepatosplenomegaly and visceral lymphadenopathies; chest X-ray was normal.
Ophthalmological and periorbital manifestations have been frequently reported during the evolution of ALL (as much as 90%), either by leukaemic infiltration or secondary to haematological derangements (such as anaemia, thrombocytopenia, leucopenia and hyperviscosity). Recurrent hemifacial oedema has not been described as a presenting symptom of ALL; however, it has been reported in the superior vena cava syndrome. The authors hypothesise that the unilateral and fluctuating character of the oedema may have been related to lymph node compression of peripheral lymphatic or vascular structures. Corticosteroid treatment might have contributed to the transient remission in the previous episodes.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd