- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Recent Advances in Technology in Diabetes Management- Dr V Mohan
There have been tremendous advances in the management of diabetes over the past few years. This is mostly due to the new technologies being introduced. These technologies are most commonly seen with respect to needles and injections used in insulin delivery apart from devices that help manage blood glucose levels better.
1. Better insulin Pens:
Conventionally, insulin used to be administered using syringes and insulin vials. In the past, the needles were long and painful and moreover, the insulin vial had to be kept in a refrigerator. Later more patient friendly insulin pens were introduced. Insulin pens eliminated the need for drawing up a dose in a syringe. The ability to dial up the desired dose led to greater accuracy and reliability, especially when using low doses in small children. The sensory and auditory feedback linked with the dial mechanism on many pens also helped patients with visual impairment. Pen devices are also more compact, portable and easier to grip. Moreover, as they are insulated, it is not necessary to keep the pen in a refrigerator all the time. This makes life much easier especially for busy people who travel a lot. However, Insulin pens are more costly than insulin vials and hence is a boon for those who can afford to use them.
2. Advances in Insulin Delivery Devices
a. Insulin pumps
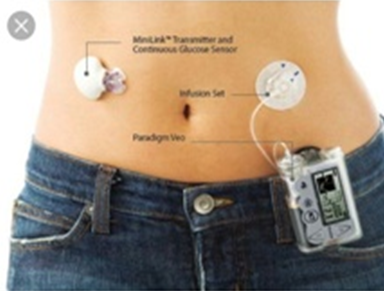
All patients with type 1 diabetes and many with type 2 diabetes require insulin therapy to control their blood glucose levels. Despite the tremendous advances made in insulin therapy over the past three decades, glycemic control remains suboptimal in the majority of patients on insulin. One of the reasons for this is that the currently used insulin regimens do not exactly mimic the physiological secretion of insulin from the beta-cells of the pancreas. The insulin pump represents an attempt to provide insulin in a more physiological manner to patients with diabetes, avoiding the 'peaks' and 'troughs' in blood insulin levels seen when using multiple subcutaneous injections.
The insulin pump (see figure above) consists of a subcutaneous cannula inserted into the interstitial space (usually of the anterior abdominal wall), a connecting tubing and a small pager-sized, battery operated pump which has the insulin reservoir as well as a microchip that controls insulin delivery according to pre-programmed rates.
Currently, insulin pumps are expensive with the basic model costing of about Rs. 1.5 lakhs in India while the more sophisticated pumps cost up to Rs. 4 or 5 lakhs.
b. Artificial Pancreas:
These are ultra modern insulin pumps with in-built glucose sensors. The ultimate Artificial Pancreas (under development now) would be able to automatically deliver the correct doses based on the blood sugars and switch off the delivery if the sugars are low or increase the rate of delivery if the sugars are high! However, true artificial pancreas is not yet commercially available.
3. Use of technology in monitoring glucose levels:
a. Blood glucose meters
Blood glucose meters have been used in clinical practice for decades and have become part and parcel of treatment of all people with diabetes. The latest glucose meters provide results that are comparable in accuracy to the venous plasma glucose estimations, at comparable or even lower costs.
b. Continuous Glucose Monitoring (CGM)
Today we have devices which can continuously monitor the glucose levels using sensors applied to the body. These are particularly useful for those who have fluctuating glucose levels.
c. Ambulatory Glucose Profile (AGP)
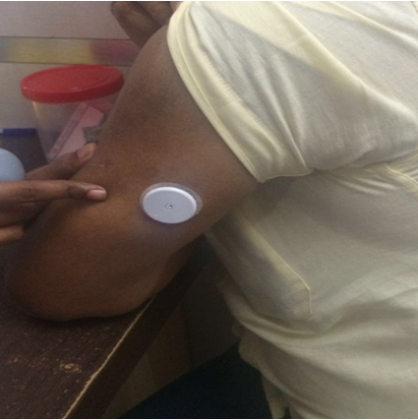
The FreeStyle LibreTM device made by Abbott consists of a small sensor which is worn continuously by the patient for the duration of the profiling (up to 14 days). The glucose values recorded by the sensor are wirelessly transmitted to a reader (usually kept with the healthcare provider) and downloaded in the form of graphs using proprietary software. The graphs provide glucose curves for each of the 14 days, as well as a "modal day" curve prepared by collapsing the readings from 14 days into a single curve. This is called as Ambulatory Glucose Profile (AGP).
The AGP is an improvement upon the original continuous glucose monitoring system in its longer duration of recording (upto 14 days) and in that, there is no need of calibrating with a capillary glucose meter. It is also far less expensive. The AGO is a useful educational and motivational tool for patients in addition to helping the clinician plan and titrates antidiabetic drug regimens more accurately.
Other Continuous Glucose Monitors (CGM)
There are CGM devices made by other companies like Medtronics and Dexcom which are also widely in use.
4. Use of mobile phones (mHealth/mDiabetes):
Today smartphones are ubiquitous and hence are used in healthcare. Mobile health technology is making health care more accessible and more flexible, places more power in the hands of patients, and is contributing to greater efficiency of medical practices. Various apps are now available to measure your diet, exercise and track your body weight glucose levels, blood pressure, cholesterol, etc. You can also communicate the results to your doctor or health care provider making remote monitoring possible.
5. Use of Telemedicine:
Telemedicine has transformed into a complex integrated service used in hospitals, private physician offices, and other healthcare facilities. It has been used to overcome distance barriers and to improve access to medical services that would often not be consistently available in distant rural communities eg. in villages which would otherwise remained inaccessible.
6. Precision Diabetes:
At Dr Mohan's Diabetes Specialities Centre, over the last several years we have developed algorithms by which a precise diagnosis of diabetes can be made. Applying the principles of 'Precision Diabetes', it is possible to very accurately classify a patient, determine the type of diabetes he or she has and then decide the type of treatment that this patient is likely to respond to.
Conclusions
This review is a summary of the latest technologies now available in the management of diabetes. It is to be remembered that any device or technology, is only as good as the person who uses it. The success of these technological advances will rely significantly on the willingness of patients and doctors to adopt them and to utilize them to the fullest.
Dr V. Mohan is the Chairman and Chief of Diabetology at Dr Mohan's Diabetes Specialities Centre at Chennai in South India which is a WHO Collaborating Centre for Non-communicable Diseases Prevention and Control and IDF Centre of Excellence in Diabetes Care.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd