- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Device based treatment of hypertension: Recent advances EuroPCR 2018
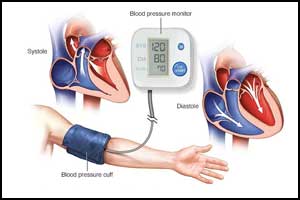
At EuroPCR 2018, two important studies will be presented on renal denervation for hypertension treatment which will be simultaneously published in The Lancet. These studies will be significant in providing biological proof of principle of a device-oriented approach to lower blood pressure by modulating renal nerve activity.
Hypertension is on the rise continuously and is reaching epidemic levels with more than 1 billion people affected by it globally. Its control rates remain unacceptably low despite the availability of many effective and safe drugs and best efforts of clinicians for management of the condition.
Adherence to antihypertensive medications is the foundation for achieving hypertension control. Nonadherence to medication is a growing concern and often leads to adverse outcomes. The hypertensive patients become non-adherent in the first year after initiation of drug treatment and about 20% are completely non-adherent. According to some previous research, the adherence worsens even more with the increasing number of anti-hypertension medications a patient is taking.
The concept of device-based treatments remains promising and is under careful investigation in lieu of the challenges encountered in finding viable solutions to hypertension and non-adherence to the medications. The continued evolution of the devices and techniques themselves, along with a deepening understanding of patient selection have the potential to lead us to new insights into possible treatment options for this disease.
During the ESC Congress last year, important data were presented which demonstrated statistically significant and clinically meaningful reductions in blood pressure following renal denervation (RDN) in patients not taking anti-hypertension medications, either throughout medication washout or in the treatment of newly diagnosed hypertensives. Also, an ambulatory blood pressure monitoring (ABPM) analysis, presented at the 2017 ACC Scientific Sessions, showed that renal denervation is “always on”, even during high-risk periods such as in the early morning hours, when a drug’s effect may be subsiding or absent.
The studies include:
- The prospective, randomized, sham-controlled SPYRAL HTN-ON MED study investigated renal denervation using a radiofrequency device in the presence of antihypertensive drugs, confirming the effectiveness of blood pressure lowering in combination with pharmacotherapy (1-3 drugs). Eighty patients were randomized and followed through six months. Office and 24-hour ambulatory BP decreased significantly from baseline to six months in the renal denervation group (24-hour SBP -9.0 mmHg, 24-hour DBP -6.0 mmHg, office SBP -9.4 mmHg and office DBP -5.2 mmHg).
- The prospective, randomized, sham-controlled RADIANCE-HTN SOLO study used an ultrasound catheter to achieve renal denervation. A total of 146 were randomized to renal denervation (n=74) or sham procedure (n=72). Using this device, the investigators have now documented significant changes in office and ambulatory blood pressure following renal denervation, but not in the sham-treated patients (baseline-adjusted difference between groups: -6.3 mmHg). The primary efficacy and safety endpoints of this trial were met.
For any therapy to be effective it is critical to understand which patient will – or will not – respond favorably to the technique. The data being presented during EuroPCR 2018 should inspire new approaches to answering these questions. While there are some interesting hypotheses and views in the community, for the moment we look forward to continued preclinical and clinical investigations and research which will hopefully allow us to further define patient selection for RDN. Other unanswered questions concern procedural parameters for successful renal denervation or whether the proven blood pressure-lowering effects are sustainable at long-term follow-up.
In conclusion, despite decades of effort to control hypertension through lifestyle adjustment and medication, the challenge remains. There is a huge unmet need. New approaches are critical and needed in order to increase control rates and reduce patient risk.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd