- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Problems encountered in retrograde recanalization of coronary chronic total occlusion
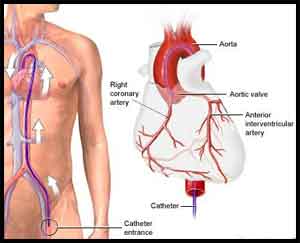
A coronary chronic total occlusion (CTO) defined as total obstruction of a coronary artery of ≥ 3 months is observed in 15-30% of the diagnostic coronary angiogram. CTOs remain quite challenging lesions for interventionists, are regarded as the last frontier due to lower success rates, and greater experience required to perform percutaneous coronary intervention (PCI) safely and effectively. Despite lack of randomized trials, successful CTO PCI improves anginal symptoms, improved left the ventricular function and reduces the need for surgical coronary artery bypass.
Despite meaningful benefit associated CTO PCI, several misconceptions prevailed: a chronically occluded artery is clinically benign; Collateral channels(CCs) are sufficient for angina relief; the area subtended by the CTO is non-viable, CTO PCI is associated with high complication rate, a lack of strong randomized data demonstrating clinical benefit. However, the relative reluctance to attempt CTO PCI is waning with improvement in the technique and technology leading to further procedural success and better outcomes.
The recognition that traditional guidewire techniques were not adequate to achieve higher procedural success rates led to development of dedicated guidewires, microcatheters, innovative methods like parallel wire technique, anchor wire, anchor balloon technique, intravascular ultrasound guidance, side branch techniques and dissection and re-entry methods played significant roles in improving the success rate via antegrade approach. Even then, the technical success rate for CTO via the antegrade approach remained suboptimal, in the range of 65%-70% worldwide. The limitations of the conventional antegrade approach are overcome by the retrograde approach that involves targeted CC crossing, retrograde lesion crossing and management of subintimal space with the use of balloon dilatation for connecting antegrade and retrograde channels.
Adoption of this technique has potentially improved the success rate of complex CTO to the extent of 90-95%. Angiographic features of blunt occlusion with a large side branch, bridging collaterals, calcification, and long CTO is no longer considered negative predictors of success while using a retrograde approach. This approach can be used after antegrade crossing failure or as an initial situation like ostial occlusions, long occlusions, heavy calcification, occlusions with ambiguous proximal cap, and occlusions with a diffusely diseased distal vessel, occlusion involving a distal major bifurcation and CTO vessels that are difficult to engage such as anomalous coronary arteries.
A retrograde approach was described in 1990 by Kahn and Hartzler. The first report of retrograde crossing via septal CC was published in 2006 that revolutionized this technique with the introduction of specialized equipment. This was further developed by the author making this approach safer, faster and more successful.
The rationale of selecting the retrograde route was established by histopathologic demonstration of communications between lumen recanalization channels and intraplaque capillaries. These channels have a branched tree-like configuration that spreads out from the proximal to the distal cap and this configuration may lead to the subintimal navigation of antegrade guidewire. The distal cap of CTO is softer, tapered and less frequently ambiguous compared to the proximal cap, better allowing the retrograde guidewire to cross the occlusion.
A retrogradely advanced guidewire can be used as a landmark for the guidewire from the antegrade approach, with the distal wire identifying the true lumen of the artery (kissing wire technique). The success rate achieved in the past with various retrograde techniques such as kissing wire, knuckle wire, and direct retrograde crossing improved with the introduction of the controlled antegrade and retrograde subintimal tracking (CART) technique where the retrogradely advanced guidewire enters a false lumen and is enlarged by inflation of the balloon, allowing the antegrade guidewire to advance to this lumen and to ultimately reach the true lumen. Reverse CART, the more reproducible and predictable technique that involved both antegrade access to the proximal cap, retrograde access to the distal cap, creation of subintimal space by antegrade balloon followed by negotiation of retrograde wire through the subintimal space into the proximal true lumen. With latest iterations described by the author such as the intravascular ultrasound-guided reverse CART, stent reverse CART, mother-child and contemporary reverse CART, the retrograde revolution broke out and its effects reverberated throughout the world.
In general, the retrograde approach carries a higher rate of complications than the antegrade one. The complications such as guidewire and balloon kinking or entrapment into the collateral channel, dissection, perforation and hematoma are exclusive to retrograde approach. In spite of various drawbacks, the retrograde (backdoor) approach is both effective and safe if performed by experienced operators in experienced centers. The author feels that patients with J-CTO score of 0–1 could be treated in any center, but those with J-CTO score ≥ 2 should be treated by an experienced CTO operator, defined as someone who has performed >300 CTOs and >50 CTOs/year, although a specific threshold is hard to define.
Dr. Debabrata Dash
The author is MD, DM, FICC, FSCAI, FCCP, FAPSC, Interventional Cardiologist at Thumbay Hospital, UAE, Department of Cardiology. He is a member Editorial Board, Cardiology at Specialty Medical Dialogues.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd