- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Positive airway pressure lowers death in obese sleep apnea patients: JAMA
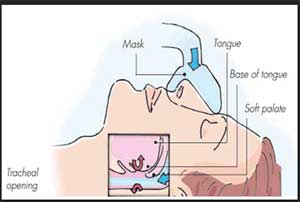
DELHI: Positive airway pressure (PAP) is a mode of respiratory ventilation used in the treatment of sleep apnea. A new study published in the journal JAMA Otolaryngology-Head & Neck Surgery has found that PAP therapy is associated with lower risk of death in patients with obesity and severe obstructive sleep apnea compared with nonprescription of PAP.
According to the study, prescription of PAP therapy was associated with a 62% lower risk of all-cause mortality compared with nonprescription of PAP, independent of major confounders.
The association of positive airway pressure with reduced mortality in patients with obstructive sleep apnea (OSA) remains uncertain. Quentin Lisan, Paris Descartes University, Faculty of Medicine, Paris, France, and colleagues conducted the study to investigate this association (between PAP therapy and mortality) in OSA obese patients.
This multicenter, population-based cohort study evaluated data from the Sleep Heart Health Study (SHHS), a long-term observational cohort study that included participants between 1995 and 1998, with a mean follow-up of 11.1 years. They matched some 80 obese patients with OSA who were prescribed positive airway pressure to 310 who were not. Of 392 study participants, 316 (80.6%) were men, and mean (SD) age was 63.1 (11.0) years.
Also Read: Soon at PGI Chandigarh: Tongue pacemaker for sleep apnea patients
Key findings of the study include:
- Ninety-six deaths occurred; 12 among the prescribed-PAP group and 84 among the nonprescribed-PAP group, yielding crude incidence rates of 12.8 vs 24.7 deaths per 1000 person-years.
- In Cox multivariate analysis, the hazard ratio (HR) of all-cause mortality for prescribed PAP therapy was 0.38.
- After propensity matching, the HR of all-cause mortality for prescribed PAP therapy was 0.58.
- According to survival curves, the difference in mortality appears 6 to 7 years after initiation of PAP therapy.
Also Read: Regular use of CPAP in sleep apnea may slow down memory loss in elderly
"Positive airway pressure prescription is associated with reduced all-cause mortality, and this association appears several years after PAP initiation. If replicated, these findings may have strong clinical implications," concluded the authors.
For detailed study log in to 10.1001/jamaoto.2019.0281

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd