- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
NICE sore throat guideline: antimicrobial prescribing
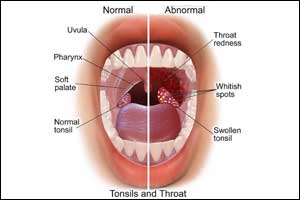
NICE has released its new guidelines for managing acute sore throat and antimicrobial prescribing.All people with acute sore throat should be aware that acute sore throat (including pharyngitis and tonsillitis) is self‑limiting and often triggered by a viral infection of the upper respiratory tract.Its symptoms can last for around 1 week, but most people will get better within this time without antibiotics, regardless of cause (bacteria or virus).It is therefore important that clinicians should assess and manage children under 5 who present with fever as outlined in the NICE guideline on fever in under 5s.They may use FeverPAIN or Centor criteria to identify people who are more likely to benefit from an antibiotic and manage in line with recommendations below.If at any time symptoms worsen rapidly or significantly alternative diagnoses such as scarlet fever or glandular fever should be considered.
Key Recommendations:
People who are unlikely to benefit from an antibiotic (FeverPAIN score of 0 or 1, or Centor score of 0, 1 or 2):
- Do not offer an antibiotic prescription
- As well as the general advice mentioned above, give advice about:
- an antibiotic not being needed
- seeking medical help if symptoms worsen rapidly or significantly, do not start to improve after 1 week, or the person becomes systemically very unwell
- See the evidence and committee discussion on no antibiotic.
People who may be more likely to benefit from an antibiotic (FeverPAIN score of 2 or 3)
- Consider no antibiotic prescription with advice or a back-up antibiotic prescription, taking account of:
- evidence that antibiotics make little difference to how long symptoms last (on average, they shorten symptoms by about 16 hours)
- evidence that most people feel better after 1 week, with or without antibiotics
- the unlikely event of complications if antibiotics are withheld
- possible adverse effects, particularly diarrhoea and nausea
- When a back-up antibiotic prescription is given, as well as the general advice in recommendation , give advice about:
- an antibiotic not being needed immediately
- using the back-up prescription if symptoms do not start to improve within 3 to 5 days or if they worsen rapidly or significantly at any time
- seeking medical help if symptoms worsen rapidly or significantly or the person becomes systemically very unwell
People who are most likely to benefit from an antibiotic (FeverPAIN score of 4 or 5, or Centor scoreof 3 or 4)
- Consider an immediate antibiotic prescription (see recommendation for choice of antibiotic), or a back-up antibiotic prescription with advice (see recommendation ), taking account of:
- the unlikely event of complications if antibiotics are withheld
- possible adverse effects, particularly diarrhoea and nausea
- When an immediate antibiotic prescription is given, as well as the general advice in recommendation , give advice about seeking medical help if symptoms worsen rapidly or significantly or the person becomes systemically very unwell
- See the evidence and committee discussion on back-up antibiotics and choice of antibiotic
People who are systemically very unwell, have symptoms and signs of a more serious illness or condition, or are at high-risk of complications
- Offer an immediate antibiotic prescription (see recommendation for choice of antibiotic) with advice or further appropriate investigation and management
- Refer people to hospital if they have acute sore throat associated with any of the following:
- a severe systemic infection (see the NICE guideline on sepsis)
- severe suppurative complications (such as quinsy [peri-tonsillar abscess] or cellulitis, parapharyngeal abscess or retropharyngeal abscess or Lemierre syndrome)
- See the evidence and committee discussion on choice of antibiotic
Self-care
All people with acute sore throat
- Consider paracetamol for pain or fever, or if preferred and suitable, ibuprofen.
- Advise about the adequate intake of fluids.
- Explain that some adults may wish to try medicated lozenges containing either a local anaesthetic, a non-steroidal anti-inflammatory drug (NSAID) or an antiseptic. However, they may only help to reduce pain by a small amount.
- Be aware that no evidence was found on non-medicated lozenges, mouthwashes, or local anaesthetic mouth spray used on its own.
- See the evidence and committee discussion on self-care
Choice of antibiotic
- When prescribing an antibiotic for acute sore throat:
- follow table 1 for adults aged 18 years and over
- follow table 2 for children and young people under 18 years
| Antibiotic* | Dosage and course length for adults† |
| First choice | |
| Phenoxymethylpenicillin | 500 mg four times a day or 1000 mg twice a day for 5 to 10 days |
| Alternative first choices for penicillin allergy or intolerance3 | |
| Clarithromycin | 250 mg to 500 mg twice a day for 5 days |
| Erythromycin | 250 mg to 500 mg four times a day or 500 mg to 1,000 mg twice a day for 5 days |
| * See BNF for appropriate use and dosing in specific populations, for example, hepatic impairment, renal impairment, pregnancy and breastfeeding. † Doses given are by mouth using immediate-release medicines, unless otherwise stated. ‡ Erythromycin is preferred in women who are pregnant. | |
| Antibiotic§ | Dosage and course length for children and young peoplel |
| First choice | |
| Phenoxymethylpenicillin | 1 to 11 months, 6 mg four times a day or 125 mg twice a day for 5 to 10 days 1 to 5 years, 125 mg four times a day or 250 mg twice a day for 5 to 10 days 6 to 11 years, 250 mg four times a day or 500 mg twice a day for 5 to 10 days 12 to 17 years, 500 mg four times a day or 1,000 mg twice a day for 5 to 10 days |
| Alternative first choices for penicillin allergy or intolerance¶ | |
| Clarithromycin | 1 month to 11 years: Under 8 kg, mg/kg twice a day for 5 days 8 to 11 kg, 6 mg twice a day for 5 days 12 to 19 kg, 125 mg twice a day for 5 days 20 to 29 kg, 18 mg twice a day for 5 days 30 to 40 kg, 250 mg twice a day for 5 days or 12 to 17 years, 250 mg to 500 mg twice a day for 5 days |
| Erythromycin | 1 month to 1 year, 125 mg four times a day or 250 mg twice a day for 5 days 2 to 7 years, 250 mg four times a day or 500 mg twice a day for 5 days 8 to 17 years, 250 mg to 500 mg four times a day or 500 mg to 1000 mg twice a day for 5 days |
| § See BNF for children for appropriate use and dosing in specific populations, for example hepatic impairment and renal impairment l The age bands apply to children of average size and, in practice, the prescriber will use the age bands in conjunction with other factors such as the severity of the condition and the child’s size in relation to the average size of children of the same age. Doses given are by mouth using immediate‑release medicines, unless otherwise stated ¶ Erythromycin is preferred in young women who are pregnant | |
- See the evidence and committee discussion on choice of antibiotic and antibiotic course length
Terms used in the guideline
People with a sore throat caused by streptococcal bacteria are more likely to benefit from antibiotics. FeverPAIN or Centor criteria are clinical scoring tools that can help to identify the people in whom this is more likely
FeverPAIN criteria
- F ever (during previous 24 hours)
- P urulence (pus on tonsils)
- A ttend rapidly (within 3 days after onset of symptoms)
- Severely I nflamed tonsils
- N o cough or coryza (inflammation of mucus membranes in the nose)
Each of the FeverPAIN criteria score 1 point (maximum score of 5). Higher scores suggest more severe symptoms and likely bacterial (streptococcal) cause. A score of 0 or 1 is thought to be associated with a 13 to 18% likelihood of isolating streptococcus. A score of 2 or 3 is thought to be associated with a 34 to 40% likelihood of isolating streptococcus. A score of 4 or 5 is thought to be associated with a 62 to 65% likelihood of isolating streptococcus
For more details click on the link : https://www.nice.org.uk/guidance/ng84

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd