- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
New glaucoma drugs cause effective & lasting reduction in IOP
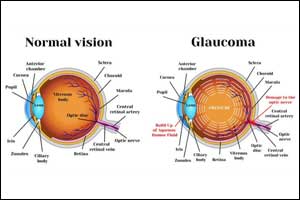
Dr. Naj Sharif, Texas Southern University, Houston, and associates have found that Two novel ocular hypotensive agents netarsudil and latanoprostene bunod (LBN) greatly reduce intraocular pressure, with lasting results in various animal models of glaucoma and in humans.The study has been Published in Journal of Ocular Pharmacology and Therapeutics.
The Special Issue entitled "Pre-Clinical Research in Drug/Device Discovery and Development," is led by Co-Guest Editors Naj Sharif, PhD, Santen Incorporated, Emeryville, CA, Sunny Ohia, PhD, Texas Southern University, Houston, and Thomas Yorio, PhD, University of North Texas Health Center, Forth Worth.
Featured in the issue is the article "Discovery and Preclinical Development of Netarsudil, a Novel Ocular Hypotensive Agent for the Treatment of Glaucoma" coauthored by Casey Kopczynski, Aerie Pharmaceuticals, Durham, NC and colleagues from National Defense Medical Center, Taipei City, Taiwan and Duke University School of Medicine, Durham. Netarsudil is a rho-associated protein kinase (ROCK) inhibitor that lowers intraocular pressure by increasing the outflow of fluid through the trabecular meshwork, the primary drainage route.
LBN, applied topically, reduces pressure in the eye of patients with open-angle glaucoma or ocular hypertension via two mechanisms, latanoprost-mediated increase in unconventional outflow and nitric oxide-mediated increase in conventional outflow. Based on a comprehensive review of nonclinical studies and a phase 2 clinical study of LBN, Megan Cavet and Heleen DeCory, Bausch + Lomb, highlight the benefits of this dual-action drug for glaucoma in the article "The Role of Nitric Oxide in the Intraocular Pressure Lowering Efficacy of Latanoprostene Bunod: Review of Nonclinical Studies".
In the article entitled "Intravitreal, Subretinal, and Suprachoroidal Injections: Evolution of Microneedles for Drug Delivery," Rachel Hartman and Uday Kompella, University of Colorado Anschutz Medical Campus, Aurora, review the development of microneedles that have a length of less than a millimeter and are able to target injectable therapeutics to previously unreachable areas of the eye, including closer to the retina. The authors note that improvements in the design of needles or intraocular drug delivery, including those with smaller diameters and lengths and with controlled bevel angles, will likely improve overall safety and acceptance of injected ophthalmic drug products and allow for a broader range of periocular, subretinal and suprachoroidal routes of delivery.
Takayoshi Masuoka, Juana Gallar, and Carlos Belmonte, Universida Miguel Hernancez-CSIC, Alicante, Spain and Kanazawa Medical University, Uchinada, Ishikawa, Japan, present a new study demonstrating the ability of amitriptylene, a voltage-gated sodium channel blocker, to reduce the activity of cold thermoreceptors, which contribute to the unpleasant sensations of pain in dry eye disease. They show that the effect differs in intact versus tear-deficient corneas.
"Outstanding preclinical research and industry/academia collaborations to rapidly and safely move forward vision-saving technologies are featured in this special issue," says Editor-in-Chief W. Daniel Stamer, PhD, Joseph A. C. Wadsworth Professor of Ophthalmology and Professor of Biomedical Engineering, Duke University, Durham, NC.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd