- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
New fast blood test for diagnosis of deep vein thrombosis
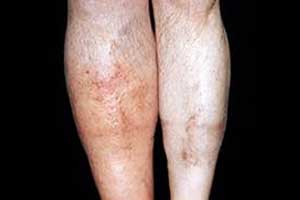
Measuring the level of a specific protein—called D-dimer (DD)—in a patient’s blood may help in the prediction of whether a time-intensive ultrasound is warranted for the testing of deep vein thrombosis (DVT).
Findings of the study, published in the journal Annals of Vascular Surgery, is significant as getting tested for DVT can disrupt a patient’s whole day. Ultrasound is typically one of the first methods used by a clinician for the diagnosing the condition in order to observe the blood vessels in a patient's legs and assess the blood flow. The procedure can take several hours and becomes onerous specifically for the rural patients, who often drive long distances to reach medical practices where the necessary equipment and personnel are available.
Albeir Mousa, professor of vascular surgery, West Virginia University, and colleagues examined the correlation between DD results alongside Wells criteria probability (WCP) score with findings on venous duplex ultrasound (VDU). They hypothesized that VDU remains overutilized in low-risk patients with negative DD and that higher DD levels may correlate with thrombus burden and location.
“Usually waiting for a venous ultrasound would be a matter of three, four, five hours. With the D-dimer test, it’s a few minutes and you’re done,” said Mousa.
Deep vein thrombosis occurs due to the formation of blood clot in a major vein, typically in the leg. This results in swelling and reddening of the patient's leg that becomes painful and feels warm to the touch. If the clot travels to the patient’s lung, it can kill lung tissue. If it doesn’t travel, it can still cause chronic abnormalities in the leg’s blood circulation.
D-dimer is a marker for the trace elements left in the bloodstream as the body works to degrade blood clots. Checking for an elevated D-dimer level is a good first-line assessment for blood clots.
Also Read: Varicose veins associated with increased risk of DVT : JAMA
For the study, the researchers retrospectively examined the patients who presented to a high-volume tertiary care center with lower limb swelling with or without associated pain for 4 consecutive years. After calculating WCP, patients were divided into low-, moderate-, and high-risk categories. Electronic DD results utilizing enzyme-linked immunosorbent assay, WCP data, and VDU analysis data were merged and analyzed based on a receiver operator characteristic curve to determine the DD cutoff point for each WCP. Abnormal DD with an average value ≥ 0.6 mg/L fibrinogen equivalent units (FEUs) was correlated to positive DVT to differentiate proximal DVT (above popliteal vein) from distal DVT (below popliteal vein).
Data of 1,909 patients were analyzed, and 239 (12.5%) patients were excluded secondary to serial repeat visits or follow-ups, surveillance screens, and if they had a previous history of DVT. The average age was 62.1 ± 16.3 years with more women (55.7%) and the majority presented with limb pain and edema (87%). DD studies were ordered and completed in 202 patients and correlated with all positive and negative DVT patient (100% sensitivity and negative predictive value, with specificity and positive predictive value of 14.9% and 15.9%, respectively).
Key Results:
- Twenty-six of 202 patients had DD that were in the normal range 0.1–0.59 mg/L (FEU), all of which were negative for DVT (100% sensitive).
- Fifty-one of 202 patients had DD values of 0.6–1.2 mg/L FEU, of which only 3 DVTs were recorded, and all of them were distal DVTs. In addition, 685 patients with WCP <1 and negative DD were sent for VDU.
- 762 patients had an unnecessary immediate VDU (Wells ≤1 and –DD) study during their initial presentation.
Our findings demonstrate that potentially 762 immediate ultrasounds could have been eliminated by using the blood test. Because it costs about $1,557 less than ultrasound imaging does, the blood test has the potential to save the hospital system more than $1 million per year, said Mousa.
“It’s a very simple sample of blood, which is sent to the lab. And usually, in 15 or 20 minutes, you have significant information that can help you take good care of the patients,” he said. “And you can send patients home quicker, with less demand on the hospital staff and the institution, yet increase patient satisfaction.”
"This study suggests that DD is still underutilized, and DD in conjunction with WCP could significantly reduce the number of unnecessary immediate VDUs. A higher value of DD (>1.2 mg/L FEU) may raise concern for proximal DVT. Concern on cost-effectiveness exists and raises the demand for a proposed algorithm to be followed," concluded the authors.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd