- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Neonatal intestinal obstruction - Standard Treatment Guidelines
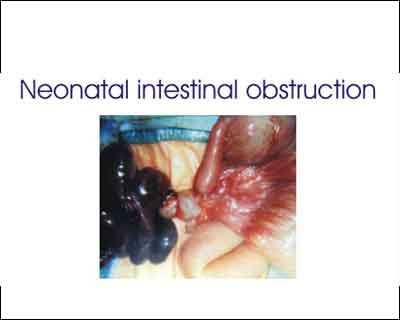
Neonatal Intestinal Obstruction (NIO) is a common condition affecting neonates and requires prompt recognition and appropriate specialist treatment to save these babies and to reduce avoidable morbidity & mortality. Intestinal Obstruction in a new born child caused by intrinsic or extrinsic factors involving the stomach / duodenum / jejunum / ileum / any part of the colon.
Ministry of Health and Family Welfare, Government of India has issued the Standard Treatment Guidelines for Neonatal intestinal obstruction. Following are the major recommendations :
Incidence of The Condition In Our Country
The Exact incidence of the condition in our population is difficult to ascertain. However it may be approximately assessed to be 14 per 1,000 live births.
Differential Diagnosis
a. Gastric Outlet Obstruction - Pyloric / Antral web /
Hypertrophic Pyloric Stenosis
b. Malrotation
c. Duodenal Atresia
d. Jejuno-ileal Atresia
e. Meconium Ileus
f. Colonic Atresia
g. Hirschprung’s Disease
h. Meconium Plug Syndrome
i. Necrotising Enterocolitis (NEC)
j. Medical conditions mimicking Neonatal intestinal
obstruction like Neonatal Sepsis with ileus,
Hypothyroidism etc.
k. Other rare conditions like intestinal duplications, intraabdominal
cysts, congenital bands etc.
Prevention And Counseling
- As this is often a congenital disease, prevention is impossible.
- However, the obstetricians at all levels need to have a high index of suspicion about the possibility of a GI
obstruction when polyhydramnios is detected on antenatal scans - When a fetus is suspected to have NIO, the counseling can be done to have a discussion with the obstetrician, the pediatrician & the pediatric surgeon and to plan the delivery to be done at a place where neonatal surgery is safely feasible.
Optimal Diagnostic Criteria, Investigations, Treatment & Referral Criteria
*Situation 1: At Secondary Hospital/ Non-Metro situation: Optimal Standards of Treatment in Situations where technology and resources are limited .
Clinical Diagnosis:
- Any child with any of the following criteria should be suspected to have NIO
- Bilious Vomiting (green colour)
- Abdominal distention
- Visible peristalsis
- Not passed meconium beyond 48 hours after birth (72 hours in preterm babies)
- Passing abnormal stool (pellets / mucus / mucus plug)
- Feed intolerance
- Upper or Lower Gastrointestinal Bleeding
Persistent Non-bilious vomiting
Investigations:
a. Plain X-Ray Abdomen (preferably erect)
b. Air contrast X-Ray - A naso-gastric tube is inserted prior to shifting the baby for the X-Ray. About 20 cc of Room air is insufflated through the naso-gastric tube and the X-Ray is taken. (This is to highlight the stomach, duodenum and the proximal jejunum and to rule out obstruction at this level.). Make sure the insufflated air is aspirated out immediately after
the X-Ray is taken and the NG tube is left for drainage
c. Ultrasonography, if indicated.
Treatment:
Standard Operating procedure
Day Care - No role for treatment on day care basis
Out Patient - No role for treatment on out-patient basis
In Patient -
Gastric Deompression
- Place a No. 8 infant feeding tube through the nasogastric route. In very small babies, orogastric
tube can be utilised if the nostrils are small. The baby should be kept nil orally. - Ensure that the tube is correctly placed in the stomach and that it is patent.
- Gently aspirate the tube hourly and connect to continuos drainage.
Maintain accurate chart to monitor the colour and volume of the aspirates
i) Temperature Maintenance
- Keep the child warm using an incubator / warmer and keeping the room ambient temperature high. A room warmer can be used in winter seasons
- Intravenous Fluids to maintain Hydration / glucose levels.
- The choice of IV fluids in the first 48 hours is 10% Dextrose @ 80 ml/ kg / day.
- After 48 hours of birth, the IV fluid of choice would be Isolyte P to be run @ 100 - 120 ml / kg / day (the rate will vary as per the gestation of the baby and other factors as determined by the pediatrician).
- The fluid should be infused using ‘Burette’ / ‘Pediatric Drip Chamber set’ in order to avoid over or under infusion. Microdrip sets with ‘dosiflow’ regulators may be used if these are not available.
- I.V. Antibiotics. Broad spectrum antibiotics to cover gram positive, gram negative and anerobic bacteria should be used. Some of the suggested combinations are:
- Ampicilin / Gentamicin / Metronidazole
- Cefotaxime / Amikacin / Metronidazole
- Co-Amoxiclav / Amikacin / Metronidazole
- The choice of the antibiotic will vary on a lot of factors and can be suitably chosen by the treating clinician .
ii. Preferable Investigations
- Serum glucose / Electrolytes
- BUN / Serum Creatinine
- Hemoglobin & Blood Counts
- Blood culture
- Ultrasonography of the Abdomen
Referral criteria:
a. Ideally, all cases of neonatal intestinal obstruction should be transferred to hospitals with level 2 / 3 Neonatal intensive care facilities.
b. However, in situations where a qualified pediatric surgeon is available, these children can be handled provided the hospital has the following facilities
- Neonatal nursery with the availability of full-time trained neonatal / pediatric nurses
- Round the clock availability of Pediatrician
- Warming system for the baby - Radiant warmer/ Incubator etc/
- Operation Theatre well equipped with Monitors for ECG / Pulse Oximetry / Baby warming systems and other facilities for operating on a small baby
- A Well Trained Anesthesiologist with adequate exposure to neonatal anesthesia
- Facilities for post-operative monitoring of the baby - warmer, multi-system monitor, resuscitation equipment etc.
c. Mode of transportation & Precautions during transfer”
- Keep the child warm using clean blankets/ thermocol boxes, cotton padding etc, Keep the NGT open & connect to continuous drainage. Strictly Avoid oral / NGT feeds
- Maintain the patency of IV line by flushing it before transportation and run fluids at the pre-determined rate if the travel is expected to last more than a few hours
- It is preferable to have a trained paramedical / medical supervision during transportation . The person should preferably be trained in basic neonatal care / neonatal resuscitation methods, handling medical equipment like those required for airway maintenance / suction etc.
*Situation 2: At Super Specialty Facility in Metro location where higher-end technology is available
Clinical Diagnosis:
- Any child with any of the following criteria should be suspected to have NIO
- Bilious Vomiting (green colour)
- Abdominal distention
- Visible peristalsis
- Not passed meconium beyond 48 hours after birth (72 hours in preterm babies)
- Passing abnormal stool (pellets / mucus / mucus plug)
- Feed intolerance
- Upper or Lower Gastrointestinal Bleeding
Persistent Non-bilious vomiting
Investigations:
Blood:
- CBC / CRP / Blood Culture
- S. Electrolytes / BUN / Creatinine
- Arterial Blood Gas
- Blood Grouping & Rh typing /
- Serum Bilirubin
- Other blood tests as deemed necessary by the neonatologist.
Imaging: (Depending on the working diagnosis)
- Plain X-Ray of Abdomen in all cases
- Air contrast X-Ray - if upper GI obstruction is suspected.
- Upper G.I. barium study - if upper GI obstruction is suspected.
- Contrast (Gastrograffin preferably) Enema - if lower GI obstruction is suspected.
- Ultrasonography of Abdomen / Pelvis
- CT scanning / MRI - in rare instances
Additional Screening for Associated anomalies may be required in select cases
- 2-D Echocardiography
- Renal Ultrasonography
- Chromosomal & Metabolic screening
- Any other as indicated
Treatment:
Standard Operating procedure
a. Out Patient - no role
b. Day Care - No role
c. In Patient:
- Initial resuscitation / Stabilisation
- IV Fluids / Antibiotics as indicated earlier
- Pre-operative Preparation - This will by and large depend on the condition of the baby and if any preexisting morbidity is present and will be handled by the neonatologist.
- Operative plan - This will depend on the diagnosis made about the level of obstruction. The possibilities include.
- Simple laparotomy + Ladd’s procedure / release of bands / Pyloromyotomy etc.
- Laparotomy + Resection anastomosis
- Laparotomy + Resection + Ileostomy / colostomy
- Laparotomy + pull-thorough
- One stage pull-through for Hirschprung’s Disease
- Laparotomy + Other procedures as per variations in the operative findings.
1. Post-operative Care - This will again have to be tailored to suit the child’s condition and requirements. The probable supportive measures will include:
- IV Fluids with possible transfusion of blood products like Packed Cells / Plasma / etc.
- IV Antibiotics- as suggested earlier and as dictated by various factors influencing the decision making process.
- Inotropic Support - Dopamine / Dobutamine/ Noradrenaline
- Ventilatory Support
- Parenteral Nutrition
- Advanced Support like peritoneal dialysis
- Vascular access
2. Some children may also require Additional Surgery like:
- Re-look laparotomy
- Definitive surgery
- Explorations for complications like anastomotic leak, adhesive obstruction / dehiscence
- Ilesotomy / colostomy closure
3. Other events during hospitalisation complicating the clinical course during hospitalisation = like renal failure, nutritional support, colostomy / ileostomy care etc.
4. Maternal support during hospitalisation including rooming in while feeding is initiated
Referral criteria :
a. Even within the metro cities, as there are several levels of hospital care available, we recommend that new born babies with surgical problem should be handled by only those hospitals with reasonably good neonatal care (level 2 & 3) facilities with the availability of qualified Pediatric Surgeon and an experienced pediatric anesthetist.
b. However, depending on the nature of the disease and the general condition of the baby, decision may be taken to handle the baby in centres with less than optimal facilities in Metro cities if there is a genuinely good cause to believe that good surgical and post-operative care can be extended to the child without much detriment to the baby
c. In any situation, after the initial resuscitation, if the general condition of the baby is poor or if there is a possible necessity of ventilatory support or specialised treatment, it will be necessary to shift the baby to a higher centre where such facilities are available, ensuring safe transportation of the baby
WHO DOES WHAT? and TIMELINES
a. Doctor
i. Pediatrician:
- Initial assessment and day to day care of the baby,
- Early involvement of a pediatric surgeon and regular co-ordination with him/ her
- taking appropriate decisions & involving the various specialists as indicated
ii. Resident / Registrar
- Periodic assessment of the patient and regular reporting to the specialists
- Carry out the orders of the Pediatrician / Pediatric Surgeon in charge of the patient
- To ensure that all the orders are properly carried out by the nursing and other paramendical personnel.
- Blood sampling and vascular access
iii. Pediatric Surgeon
- Prompt assessment of the baby on referral and to formulate an appropriate plan of action
- Co-ordinating with the anesthetist and the other Operation Theatre personnel for the proposed surgery.
- Performing the appropriate surgery and to make reasonable efforts for a smooth postoperative recovery.
- Post-operative care & Daily assessment with regard to the post-operative recovery
- Vascular access
- Take decisions with regard to the daily progress and further interventions as and when indicated
iv. Anesthetist
- Suitable pre-operative preparation
- Appropriate anesthetic care and smooth postoperative recovery
- Co-ordination with the other clinicians involved in the care of the child
v. Neonatologist
- Initial assessment and day to day care of the baby,
- Early involvement of a pediatric surgeon and regular co-ordination with him/ her
- Taking appropriate decisions & involving the various specialists as indicated
- Other specialist interventions AS AND WHEN NEEDED like :
- Vascular access
- Umbilical Venous / Arterial cannulation
- Peritoneal dialysis
- Enteral / Parenteral nutrition
a. Nurse
- Nursing care of the baby
- Following all the instructions of the attending doctors
- Close co-ordination with all the departments
- Maintaining the records of the children upto date
a. Emergency Room
- Ward
- Neonatal Intensive Care Unit
- Operation Theatre
- Post-operative Recovery
a. Technician
Guidelines by The Ministry of Health and Family Welfare :
Dr.Ramesh Santhanakrishnan, Professor and Head, Department of Pediatric Surgery, Indira Gandhi Institute of Child Health, Bangalore.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd