- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Latest Management of Kidney Stones- Minimally- invasive PCNL with High-power LASER

Management of Kidney Stones i.e nephrolithiasis witnessed a revolution in the 1980s due to the advent of shock-wave lithotripsy (Chaussey, 1980) and percutaneous nephrolithotomy (Fernstrom and Johannson, 1976; Smith, Alken, Marberger, Wickham, 1980-84). The success of these new revolutionary techniques can be gauged by the fact that in most well-equipped Urology centers in the world open surgery for kidney stones has now been practically relegated to a thing of the past. For removal of renal calculi, there are several minimally-invasive treatment options available today, including Extracorporeal Shock Wave Lithotripsy (ESWL), the Percutaneous Nephro Lithotripsy (PCNL) and Retrograde Intrarenal Surgery (RIRS).
Choosing an appropriate treatment necessitates a balance between stone clearance and morbidity related to the procedure. ESWL is a low-risk procedure, but has a high retreatment rate and often leads to persistent residual stones. Retrograde intra-renal surgery (RIRS) can minimize the risks associated with bleeding and visceral injury, but sometimes the complexity of pelvi-caliceal anatomy may impact its success rate. In addition, the overall stone-free rates of RIRS are only marginally different from ESWL. High cost and poor durability of the flexible ureteroscope also limits its application, especially in socio-economic settings of developing countries such as Indian sub-continent.
Percutaneous nephrolithotripsy (PCNL) is based on the creation of a direct percutaneous renal access to the pelvi-calyceal system of the kidney, followed by fragmentation and removal of the stone. It has been well established by now that PCNL can achieve a higher stone-free rate as compared to other modalities, over a shorter treatment period in most patients. However, the biggest limitation of PCNL is its relatively higher morbidity, including complications like bleeding and injury. Since there is now enough evidence suggesting that decreasing the tract size for PCNL could decrease bleeding and morbidity, recent efforts to decrease the complications of PCNL have focused on reducing access size, leading to the development of several ‘Minimally-invasive’ percutaneous approaches.
‘Minimally-invasive PCNL’ approach utilizes nephroscopes of 7-12 F size, with Amplatz sheath size being reduced to 11-15F, as opposed to 24-30 F sizes sheaths used in the conventional PCNL (Fig 1). Reducing the sheath size from 30 F to 11 F effectively reduces the cross-sectional surface area of the tract to one-eighth, thereby significantly reducing the tissue trauma as well as the risk of bleeding-related complications.
 Fig 1: Minimally- invasive PCNL Sheaths (11-15F) compared to conventional sheath
Fig 1: Minimally- invasive PCNL Sheaths (11-15F) compared to conventional sheathFragmentation of stone is done by high-power Lumenis Holmium Laser lithotripsy (Fig 2). Lumenis 100 watt high power holmium lasers allow quick and effective fragmentation of stones of all types and densities. With experience, full potential and benefits of the laser in percutaneous lithotripsy can be achieved using a judicious combination of energy and frequency. Whereas higher power (Joules) with lower frequency results in disintegration of stone in large fragments, choosing lower power settings with high-frequency results in the production of fine fragments or ‘dusting’ effect. Since fragments are cleared spontaneously as they are fragmented under the water-jet effect, the procedure is very fast and efficient.
 Fig 2: Holmium Laser Machine (100 watts)
Fig 2: Holmium Laser Machine (100 watts)Indications: Minimally-invasive PCNL is technically feasible, safe, and efficacious alternative for small volume renal calculus disease with an advantage of high stone-free rates and lower complication rates. This procedure offers an alternative to ESWL and RIRS for the management of kidney stones in the smaller (up to 1.5 – 2.0 cm) range. The indications for this minimally invasive PCNL approach are moderate-sized stones as an alternative to ESWL or RIRS, lower pole stones which are not amenable to RIRS, diverticular renal stones, and stones refractory ESWL.
Procedure: A detailed medical history, physical examination, urinalysis, urine culture, complete blood count, serum biochemistry, coagulation test, kidney urinary bladder X-ray (KUB), renal ultrasonography (US), and intravenous urography (IVU) or computed tomography (CT) are performed on all patients. Patients who have positive urine cultures are treated with appropriate antibiotics pre-operatively.
The basic steps of mini PCNL remain the same as the conventional PCNL. The procedure is mostly done under epidural, spinal or general anesthesia, but can be done under intravenous sedation and local anesthesia as well. After retrograde ureteric catheterization with a 5 or 6Fr open-ended ureteric catheter, the patient is placed prone under a C-arm image intensifier, and an 18-gauge needle is placed, under fluoroscopic and ultrasonic guidance, through the flank into the kidney into the calyx through which access is desired. A guide wire of .035 or .038 size is passed through the needle, and the tract is dilated by passing a Teflon or metal dilator over the guide wire. Unlike conventional PCNL, only a single-step dilatation is required in most cases (Fig 3). Dilatation proceeds under fluoroscopic control and the 15 F Amplatz sheath is passed over the dilator, to provide direct access to the collecting system. The nephroscope is passed through the sheath to visualize the inside of the collecting system.
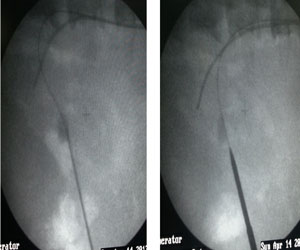 Fig 3: Mini PCNL steps
Fig 3: Mini PCNL stepsThe calculus is then fragmented by holmium-YAG laser using a 365micron end-firing fiber with the settings of 10–50W under direct visualization. The maintenance of the vision and irrigation is provided by a pulsed perfusion pump controlled by the surgeon. One additional feature of this technique is spontaneous expulsion of stone fragments through the sheath as they are broken up, under influence of the turbulence produced by the irrigation fluid (Fig 4), as opposed to the conventional PCNL, where each fragment requires to be manually extracted.
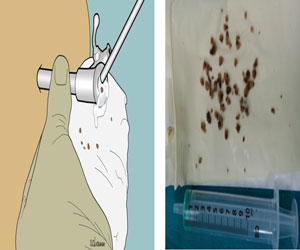 Fig 4: Spontaneous expulsion of fragments
Fig 4: Spontaneous expulsion of fragmentsAt the end of the procedure, the collecting system accessible to the telescope combined fluoroscopy is examined for any remaining fragments. Most of these procedures are ‘tubeless’ as no nephrostomy tube is routinely placed except for those requiring a second-look nephroscopy. No double-J stent is routine placed at the end of the procedure except for patients with edema or obstruction at pelvi-ureteric junction or ureter. Only the ureteric catheter, which was initially placed, is left indwelling overnight; to be removed along with the Foley catheter before discharge from the hospital.
The comparatively smaller tract in minimally-invasive PCNL, as opposed to standard PCNL, allows the procedure to be significantly less painful in the post-operative period, with significantly less tissue trauma and faster recovery. Majority of the patients are discharged the next day after the procedure.
Routine KUB x-ray is done in all patients before discharge from hospital on postoperative day 1 to assess for residual stone fragments. NCCT is done at 2 to 4 week follow up to assess the stone-free status in all patients. The composition of the stones of all patients is analyzed by infrared spectroscopy (FTIR), and appropriate long term prophylaxis advised accordingly.
Advantages:
- As mentioned, the biggest USP of this procedure is its minimal invasiveness, leading to reduced post-operative pain and need for analgesia, along with a shorter period of convalescence as compared to conventional PCNL.
- The advantages of using Laser for stone fragmentation are many. Laser lithotripsy is very efficient in fragmenting stones of all varieties and densities with equal ease, in a controlled fashion, without pushing the stone and causing stone migration. The thin laser fibre is ideally suited to use through the miniature endoscopic instruments.
- With proper case selection, the operating time can be kept quite short, comparable with conventional PCNL. It is definitely shorter than RIRS for a comparably sized stone. The entire procedure is finished invariably in a single sitting.
- Due to the use of a small calibre nephroscope allowing free flow of irrigation fluid, the intra-renal pressure is kept low during the operative procedure, thus avoiding hazards associated with high intra-renal pressure as generated in RIRS, eg. extravasation, fluid absorption, post-operative pyrexia, flank pain, etc.
- The vast majority of these cases are done truly and completely ‘Tubeless’, with no nephrostomy tube or DJ stent left indwelling. This further reduces the post-operative pain and discomfort and eliminates the need for a second procedure for stent removal.
- The hospital stay of the patients is shorter than conventional PCNL. Almost all patients leave hospital within 48 hours, the average hospital stay being only about 24+4 hours. Readmission rates for secondary procedures are very low.
- The risk of bleeding, both intra-operatively and post-operatively, is significantly minimized. Blood transfusion is almost never required. The much-dreaded complication of arterio-venous fistula formation and recurrent secondary hemorrhage is also significantly reduced, if not completely eliminated.
- The cost of the procedure, including the cost of disposables and maintenance of the equipment is quite low, comparable to conventional PCNL, as opposed to procedures like RIRS, which require high expenditure on disposables, accessories and cost of frequent repair/ replacement of equipment.
However, the limits of the minimally-invasive PCNL are that the operative time taken to fragment large, especially staghorn stones will be much longer than that of the standard PCNL. Thus standard PCNL is still required for large stone burden cases, especially for stones larger than 2 cm, multiple or staghorn stones.
Conclusion: When conventional therapies reach their limits, Minimally-invasive PCNL expands the treatment range for percutaneous removal of kidney stones. Compared with ESWL and RIRS, this approach offers higher stone-free rates without increasing complication rates.
This is the latest and most advanced procedure for kidney stone where the patient leaves the hospital completely stone-free and tube-free in less than 48 hours, something which cannot be claimed after other minimally invasive options like ESWL or RIRS on a routine basis.
The study is jointly contributed by Dr. Madhu Sudan Agrawal MS, MNAMS, MCh (Urology) Chairman, Urology Department, Global Rainbow Hospital, Agra, India Formerly: Professor, S. N. Medical College & Hospital, Agra, India, and Dr. Dilip Kumar Mishra M.S., M.R.C.S. (UK), F.R.L.S. (Japan), F.I.C.S.(USA), M.Ch.(Urology) Consultant Urologist, Global Rainbow Healthcare, Agra & Pushpanjali Hospital & Research Centre, Agra, India.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd