- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Management of Stevens–Johnson syndrome: British Association of Dermatologists' guidelines
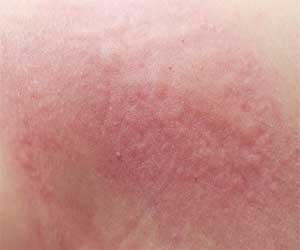
The British Association of Dermatologists has released an up‐to‐date, evidence‐based recommendations for diagnosis and management of the full spectrum of Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN) and SJS‐TEN overlap in children (0–12 years) and young people (13–17 years) during the acute phase of the disease.
The recommendations are published in the British Journal of Dermatology.
It contains recommendations on initial assessment, diagnosis, clinical assessment, stabilization, care setting, skin care, fluid replacement, immunomodulatory therapy and urogenital care as described below:
Initial assessment on presentation
- Take a detailed history from children/young people with SJS/TEN and their parents/carers with specific reference to the following:
- Symptoms suggestive of SJS/TEN including a prodromal illness (fever, malaise, upper respiratory tract symptoms); onset of a painful rash, initially on the face and chest; involvement of mucosal sites (eyes, mouth, nose, genitalia)
- Date when the rash first appeared and document the progression of the eruption
- Symptoms indicating the involvement of the genital tract including pain and urinary retention
- Symptoms indicating the involvement of the respiratory tract, i.e. cough, dyspnoea, bronchial hypersecretion, hemoptysis
- Symptoms indicating bowel involvement, i.e. diarrhea, abdominal distension
- Date when the patient developed the first symptom or sign of the disorder, e.g. sore throat, rash, skin pain, sore eyes/mouth
- Previous or ongoing medical problems; specifically, history of previous drug reactions, recurrent herpes simplex virus (HSV) infections, chest infections, diagnosis and treatment for malignancy and/or stem cell transplant.
Diagnosis and causality
- Exclude the differential diagnosis staphylococcal scalded skin syndrome (SSSS), by clinical assessment of mucosae (not involved in SSSS) and skin biopsy if any diagnostic uncertainty.
- Investigate potential infectious etiology in all patients and identify children/young people with specific clinical phenotypes more likely to be caused by respiratory infections.
- Investigate the triggering role of HSV, mycoplasma or chlamydia infections. Discuss with infectious diseases team, depending on clinical presentation and results of the infectious screen; consider targeted antibiotics as appropriate.
- Record all medicines taken and vaccinations received over the preceding 2 months, including over‐the‐counter and complementary/alternative therapies.
- Immediately discontinue* any potential culprit drug causing SJS/TEN.
Clinical assessment: prognostic indicators
- Identify high‐risk children/young people, e.g. those with likely drug trigger and underlying diseases associated with a worse prognosis (malignancy and previous stem cell transplant).
- Consider calculating SCORe of TEN (SCORTEN) to give a prognostic indicator.
- Perform a full physical examination
- Within 24 h of diagnosis, arrange an examination of the eyes by an ophthalmologist experienced in ocular surface diseases in children/young people
Stabilization
- Assess airway by a pediatric anesthetist or pediatric intensivist and consider intubation if clinical signs support this, especially if a transfer is planned. Ensure immediate availability of appropriate equipment for difficult intubation.
- Consider the involvement of ear, nose and throat team for further airway assessment.
- Initiate early discussion with a pediatric intensivist if respiratory symptoms are present, with rapid transfer to a pediatric intensive care unit (PICU) where fiber-optic bronchoscopy could be considered.
- Establish peripheral venous access; where possible, insert the cannula through nonlesional skin; commence appropriate intravenous fluid resuscitation if clinically indicated; beware of hyponatraemia. Accurately record fluid intake and output and balance.
- Record weight and repeat at frequent intervals as required clinically (no less than weekly).
- Ascertain whether the child/young person can maintain adequate hydration and nutrition orally; if this is not possible, insert a nasogastric tube and institute nasogastric feeding immediately.
- Insert a urinary catheter if urogenital involvement is causing significant dysuria or retention; a urinary catheter should also be used in patients with significant skin loss to permit accurate output monitoring and assist with fluid replacement.
Care setting
- Ensure care is developmentally appropriate and facilities are in place to support both the patient and their relevant carers.
- Seek telemedicine advice from a specialist SJS/TEN center to support local expertise.
- Admit without delay to a PICU or burn center with an on‐site PICU that has experience in treating the following scenarios and has the facilities to manage extensive skin loss.
- Barrier nurse in a side room controlled for humidity, on a pressure‐relieving mattress, with the ambient temperature between 25 °C and 28° C.
Fluid replacement
- Monitor fluid balance carefully and catheterize if clinically indicated.
- Establish adequate intravenous fluid replacement; fluid replacement can be guided by urine output and other endpoint measurements (see R29). Fluid replacement should be adjusted daily with careful monitoring of sodium levels.
- Encourage* or increase oral administration of fluids progressively with an improvement of mouth involvement.
Nutrition
- Provide nutrition early and throughout the acute phase, either by mouth or nasogastric/nasojejunal feeding if adequate oral intake is precluded by buccal mucositis.
- Involve a paediatric dietician to advise on nutritional requirements.
- Perform a nutritional screen, as stipulated by local policy, within 24 h of admission, including measurement of weight and assessment of refeeding risk.
- Measure weight weekly (minimum) or if the clinical situation changes to support monitoring of nutritional interventions.
Skin care
- Handle the skin carefully and reduce shearing forces to minimize the extent of epidermal detachment.
- Limit epidermal trauma by avoiding the use of sphygmomanometer cuffs, adhesive electrocardiogram (ECG) leads, adhesive dressings and identification wrist tags.
- Involve physiotherapy for mobilization, those needing respiratory support and in those who are immobile and in need of passive exercises.
- Administer systemic antibiotics only if there are clinical signs of systemic infection. The choice of systemic antibiotic should be guided by local microbiological advice.
- Consider amniotic membrane transplantation in the presence of conjunctival, epithelial defects or damage.
- Apply an ocular lubricant, e.g. preservative‐free sodium hyaluronate or carmellose eye drops or preservative‐free ophthalmic ointment, every 1–2 h when there is defined ocular involvement during the acute phase.
Urogenital care
- Consider catheterization of both boys and girls if required to reduce pain on passing urine and for assessment of fluid balance.
- Apply a greasy emollient (WSP ointment or 50/50 WSP/LP) to the urogenital skin and mucosae every 2–4 h during the acute phase.
- Ensure appropriate management of genital mucosae taking note of issues such as developmental differences in prepubertal girls and relevant child protection issues.
- Consider clobetasol propionate 0·05% ointment applied to tampon or vaginal applicator inserted into the vagina. An alternative for younger children may be hydrocortisone foam pessaries.
Immunomodulatory therapy
- If immunomodulatory therapy is instituted, e.g. IVIg, administer* under the supervision of a specialist skin failure MDT in the context of clinical research and/or case registry.
For detailed recommendations follow the link: https://doi.org/10.1111/bjd.17841
British Association of DermatologistsBritish Journal of Dermatologycarmellose eye dropschlamydiaclobetasol propionateDiagnosisemollientepidermal detachmenteye dropsfluid replacementHSVimmunomodulatory therapyInfectionsmanagementMycoplasmaprodromal illnessSJSsodium hyaluronatesphygmomanometer cuffsstaphylococcal scalded skin syndromeStevens-Johnson SyndromeToxic Epidermal Necrolysis
Source : With inputs from British Journal of DermatologyNext Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd