- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Long Limb Trauma: Fracture Neck of Femur (Intra-capsular) - Standard Treatment Guidelines
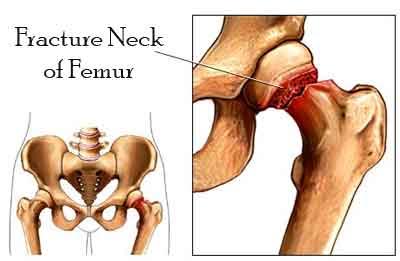
Fracture neck of femur is still the unresolved fracture as evident by the number of procedures available and practiced, thus none is universally applicable and the surgeon has to select one which would be ideal in a given situation. The treatment varies with the age of the patient, the level of the fracture and the displacement of the fragments. Also, the duration of the fracture is a major deciding factor. If union of the fracture is not likely to be achieved then what alternative method should be adopted which will suit the patient, keeping in mind his age, lifestyle, profession and economic status. Majority of our patients are not covered by health insurances, hence all the expenditure has to be born by the patient himself. It is therefore desirable on the part of treating orthopedic surgeon to choose a method which these patients can afford.
Fracture neck femur is commonly seen in old people but in our country quite a good number of patients are young adults. It is infrequent in children.
Fracture neck femur whether intra-capsular or extra-capsular can be diagnosed and differentiated by clinical examination and confirmed by the roentgenograms. Any underlying pathologic condition like metastasis or osteoporosis if present can also be identified on roentgenograms.
The Ministry of Health and Family Welfare has issued the Standard Treatment Guidelines Critical Care for Long Limb Trauma: Fracture Neck of Femur (Intra-capsular) . Following are the major recommendations:
Fracture neck femur intra-capsular can be divided as per the following classifications:
(A) Garden Classification
- Type 1 is a stable fracture with impaction in valgus.
- Type 2 is complete fracture but non-displaced.
- Type 3 is displaced (often rotated and angulated) with varus displacement but still has some contact between the two fragments.
- Type 4 is completely displaced and there is no contact between the fracture fragments.
(B) According to the site of fracture
- Subcapital
- Transcervical
- Basicervical
Usually caused by trivial fall in the elderly due to presence of osteoporosis, however metastasis from malignancies can also lead to the pathologic fractures.
The aim of treatment is to achieve union of the fracture and a durable hip joint afterwards. Principles of management include:
a. Osteosynthesis
i. Screws, Moore’s Pins etc
ii. DHS, Blade Plate
iii. Internal Fixation + Fibular Grafting
iv. Muscle pedicle Graft + Internal Fixation
b. Osteotomy
i. Pauwels valgus osteotomy
ii. Mcmurray’s osteotomy
c. Arthroplasty
i. Hemiarthroplasty
ii. Total Hip Replacement
iii. Excision Arthroplasty
The following points should be considered.
1. Age of the patient : Based on the age the following groups should be made.
a. 1-16 years before the closure of the upper femoral epiphysis
b. 16-50 years young adults
c. 50-60 years middle age group
d. Above 60 years (old age)
2. Site of fracture :
a. Sub-capital
b. Transcervical
c. Basicervical
3. Displacement of fragments:
a. Undisplaced fractures
b. Displaced fractures
4. Duration of fracture:
a. 1-21 days – Fresh
b. More than 21 days – Neglected fracure
Management : Primary health centre level : The doctor on duty should recognise the features of fracture and disloction. Only first aid including the splintage and intravenous drip should be given. In open fractures Tetanus toxoid can be given. There is no need to waste time in preparation of medico-legal formalities. The injured should be referred to the higher centre earliest feasible causing no further harm.
Community health centre and Civil hospital level: (Non Metro Hospital)
1. Investigations : X-rays of the pelvis including both hip and knee joint and of other areas if required, General Investigations and specific if required according to the status of the health of the patient.
2. Treatment :
Fresh Fracture :
Age 1-16 years when growth plate is intact
The implant used for internal fixation either should not cross the epiphyseal plate or the implant causing least possible damage should be used.
Sub-capital and transcervical fractures should be fixed with multiple Kirschner (K) wires or Moore’s pins after closed reduction in valgus.
Basicervical fractures can be fixed either by K wires, Moore’s pins or cancellous/cannulated lag screws. When screws are used they should not cross the preferably epiphyseal plate.
Age 16-50 years
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. If closed reduction fails open reduction is done followed by any of the above procedures.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Closed reduction and fixation with Lag screws or DHS. If closed reduction fails then open reduction and internal fixation (ORIF) with lag screws or DHS.
Age 50-60 years :
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient. If closed reduction fails open reduction and fixation with any of the methods described above may be done or hemi/excision arthroplasty may be offered according to the need and requirement of the patient.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient. If closed reduction fails open reduction and fixation with any of the methods described above may be done or hemi/excision arthroplasty may be offered.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Closed reduction and fixation with Lag screws or DHS. If closed reduction fails then open reduction and internal fixation (ORIF) with lag screws or DHS. Hemi/excision arthroplasty may be offered.
Physiologic Age above 60 years:
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
3. Referral Criteria for Metro hospital
a. Polytrauma patient.
b. Patient with co-morbid conditions requiring multiple speciality care.
c. Patients requiring Joint replacement.
d. Non unions / Neglected fractures ie fractures more than 3 weeks duration.
e. Pathological fractures.
f. Suspected HIV positive cases.
g. Fractures associated with any condition requiring higher investigations like CT Scan, MRI etc.
Metro hospital level :
1. Investigations : X-rays of the pelvis including both hips and knee and of other areas if required, General Investigations and specific if required according to the presence of any co-morbidity. Special investigations like MRI/CT scan if required.
2. Treatment :
Fresh Fracture :
Age 1-16 years when growth plate is intact
The implant used for internal fixation either should not cross the epiphyseal plate or the implant causing least possible damage should be used.
Sub-capital and transcervical fractures should be fixed with multiple Kirschner (K) wires or Moore’s pins after closed reduction in valgus.
Basicervical fractures can be fixed either by K wires, Moore’s pins or cancellous/cannulated lag screws. When screws are used they should not cross the preferably epiphyseal plate.
Age 16-50 years
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. If closed reduction fails open reduction is done followed by any of the above procedures.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Closed reduction and fixation with Lag screws or DHS. If closed reduction fails then open reduction and internal fixation (ORIF) with lag screws or DHS.
Age 50-60 years :
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient. If closed reduction fails open reduction and fixation with any of the methods described above may be done or hemi/excision arthroplasty may be offered according to the need and requirement of the patient.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws
Displaced : Closed reduction and fixation with Lag screws. Valgus osteotomy and fixation with double angled blade plate can also be done to convert shearing forces into compression forces. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient. If closed reduction fails open reduction and fixation with any of the methods described above may be done or hemi/excision arthroplasty may be offered.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Closed reduction and fixation with Lag screws or DHS. If closed reduction fails then open reduction and internal fixation (ORIF) with lag screws or DHS. Hemi/excision arthroplasty may be offered.
Physiologic Age above 60 years:
Sub-capital fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Transcervical fractures :
Undisplaced : Internal fixation with 2-3 cancellous/cannulated lag screws. Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
Basicervical fractures :
Undisplaced : Internal fixation with Dynamic Hip Screw (DHS)
Displaced : Arthroplasty including hemi or excision may be done according to the need and requirement of the patient.
3. Referral Criteria for Metro hospital
a. Polytrauma patient.
b. Patient with co-morbid conditions requiring multiple speciality care.
c. Patients requiring Joint replacement.
d. Non unions / Neglected fractures ie fractures more than 3 weeks duration.
e. Pathological fractures.
f. Suspected HIV positive cases.
g. Fractures associated with any condition requiring higher investigations like CT Scan, MRI etc.
Fracture More Than 3 Weeks Duration
Osteosynthesis in such fractures has a high failure rate. Internal fixation has to be combined with some type of bone graft or osteotomy particularly in young patients in whom it is desirable to preserve the patient’s own femoral head. In patients above the physiologic age of 60 years arthroplasty is the preferred treatment whether unipolar, bipolar, total hip or excision is as per the affordability and requirement of the lifestyle of the patient and condition of the hip joint (Osteoarthrosis).
Age 1-16 years :
Mc Murray’s osteotomy and POP one and a half spica may be tried. Abduction osteotomy and internal fixation with angled paediatric blade plate. Care should be taken not to damage the epiphyseal plate. If the gap between the fragments is more than 1 cm free fibula with a screw may be tried but the chances of damage to the epiphyseal plate are very high leading to limb length discrepancy and deformity of head later on.
Age 16-55 years :
In this age group patients own hip should be joint should be preserved. Osteosynthesis is carried out aiming at union of fracture and obtaining a durable hip joint. The results of various procedures depend upon the changes which have already taken place at the site of fracture with passage of time. These changes are:
a) Fracture surfaces get smoothened out.
b) There is progressive absorption of the neck of femur resulting in increase in the gap between the fragments and decrease in the size of the proximal fragment.
c) The head of the femur may start showing signs of avascular necrosis.
A good quality X-ray of pelvis including both hip joints in as identical position as possible should be taken. CT scan or MRI of pelvis can be extremely useful in accurately measuring the gap between the fragments and the size of the proximal fragment. Sometimes the absorption of the proximal fragment is more marked in the centre than the periphery giving it the shape of a cup or moon. This may not be clearly seen on routine. AP view X-ray of the hip and can be better appreciated on CT scan or MRI. Avascular necrosis of the head of the femur may be seen earlier on MRI / CT scan than on plain X-ray of the hip.
Based on these changes the fracture can be allocated to one of the following 3 stages.
Stage I
a) Fracture surfaces are still irregular (Fresh)
b) The size of proximal fragment is 2.5 cm or more
c) Gap between the fragments is 1 cm or less
d) Head of the femur is viable. There is no sign of avascular necrosis on X-ray picture or MRI or CT Scan.
Stage II
a) Fracture surfaces are smoothened out
b) The size of the proximal fragment is 2.5 cm or more
c) The gap between the fragments is more than 1 cm but less than 2.5 cm
d) The head of the femur is viable. If either of the feature a or c is present it is allocated to stage II.
Stage III
a) Fracture surfaces are smoothened out
b) The size of the proximal fragment is less than 2.5 cms
c) The gap between the fragments is more than 2.5 cms
d) The head of the femur shows signs of avascular necrosis If any of the feature b, c or d is present the fracture is allocated to stage III.
Treatment
Stage I: In this stage, the success rate of various procedures aimed at osteosynthesis is very high. The procedures which are useful are:
1. Closed reduction and internal fixation with one screw and double fibular graft or 2 screws and one fibular graft. If the neck of the femur is narrow then one screw and one fibular graft may be given.
2. Closed/open reduction Vascularised fibular graft along with screw/k-wire
3. Closed reduction or open reduction and bone muscle pedicle graft based on quadratus femoris or sartorius or tensor fascia femoris can be used.
4. Abduction osteotomy and osteosynthesis with double angled blade plate. This procedure is particularly useful when the fracture is situated more near the base and length of proximal fragment is 3.5 cms or more.
5. McMurrays osteotomy with one and half POP hip spica.
Stage II : In this stage when the fracture surfaces are smoothened out (as in case of established nonunion) and the gap between the fragments is more than 1 cm various methods of osteosyntehsis which have given good results are
1. Closed reduction and internal fixation with one screw and double fibular graft or 2 screws and 1 fibular graft.
2. Open reduction, freshening of fracture surfaces and internal fixation with 2 screws and one free fibular graft.
3. Closed/open reduction Vascularised fibular graft along with screw/k-wire
4. Open reduction and internal fixation with multiple screws and bone muscle pedicle graft based on quadratus femoris or sartorius or tensor fascia femoris.
5. Other methods of treatment which can be useful (although they will not achieve union of fracture but improve the function of hip) are
a. McMurrays osteotomy
b. Osteotomy with internal fixation
c. Bachelor's or Girdlestone procedure
Stage III : In this stage when the size of the proximal is less 2.5 cms, it cannot give good hold to the implant as well as the graft or there is a gap of more than 2.5 cm between the fragments or femoral head is showing signs of avascular necrosis, chances of union are less. Osteosynthesis is likely to have very high failure rate. The treatment options available are
1. Total hip arthroplasty if the patient can afford and his life style permits. It may preferably be non-cemented or may be cemented.
2. Bipolar or hemi arthroplasty
3. McMurray's osteotomy
4. Subtrochantric osteotomy with internal fixation
5. Excision hip Girdlestone's or Bachelor's procedure
6. Patient may be left alone if the patient is poor and cannot afford treatment or is unfit for surgery. He can start walking with the support of a walker or crutches. Later on he can walk with the support of stick or even without than in about 3-4 months time. They are often able to squat or sit in cross legged position (Budha position).
After the age of 55 years
1. Replacement arthroplasty : if the patient can afford or his life style permits. It may be total hip replacement or bipolar or hemi-arthroplasty.
2. Osteosynthesis if the patient wants it and is prepared to wait for 5 - 7 months for independent walking. This should be carried out only in stage I and stage II.
3. Excision hip (Girdlestone procedure or Bachelor's procedure)
4. Osteotomy with internal fixation
5. Leave him alone.
There are rough guidelines to help the orthopaedic surgeon to manage fracture neck of femur in different age groups and fracture at different levels of neck for fresh as well as neglected cases. The decision regarding the choice of operative procedure rests with the surgeon depending upon the patient's requirements, his life style, profession and financial position. It also depends upon the training of the Orthopaedic surgeon and facilities available to him. Use of free fibular graft/vascularised fibula in addition to internal fixation with screws particularly where there is posterior comminution improve the chances of union and may be carried out in such cases. If the reduction of the fracture is less than anatomical but otherwise satisfactory addition of free fibular graft can improve the chances of union.
If the patient is suffering from a generalized disease like diabetes mellitus, congestive heart failure, chronic kidney or liver disease, malignancy etc., or is taking steroids adversely affecting the chances of union of fracture, replacement arthroplasty may be a better option even in younger.
Guidelines by The Ministry of Health and Family Welfare :
Group Head Coordinates of Development Team Dr. P.K. DAVE, Rockland Hospital, New Delhi Dr. P.S. Maini, Fortis Jessa Ram Hospital, New Delhi
Reviewed By
Dr. V.K. Sharma, Professor Central Instiute of Orthopaedics, Safdarjung Hospital, New Delhi

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd