- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Latest Clinical Practice Guidelines for SLE
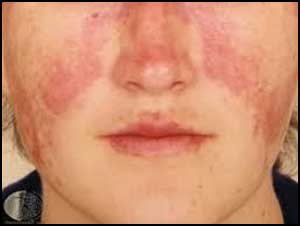
The Latin American clinical practice guidelines for systemic lupus erythematosus (SLE) covering the best pharmacologic interventions for musculoskeletal, mucocutaneous, kidney, cardiac, pulmonary, neuropsychiatric, hematological manifestations and the antiphospholipid syndrome appeared in the journal Annals of Rheumatic Disease. Systemic lupus erythematosus (SLE), a complex and heterogeneous autoimmune disease diminished quality of life and reduced life expectancy.
The recommendations were developed by two independent teams (rheumatologists with experience in lupus management and methodologists) with evidence-based research based on a selected list of questions for the clinical problems most commonly seen in Latin American patients with SLE.
Eight overarching principals and eight recommendations were formulated using the Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach.
Overarching principles
- Treatment should be individualized, specialists and generalists should work together and the active involvement of patients and their family members on the overall therapeutic plan should be emphasized.
- The therapeutic goal should be to reach and maintain remission or low-disease activity as soon as the diagnosis is made and for as long as possible.
- Treatment should include photo-protection, osteoporosis, cardiovascular, metabolic syndrome and infection prevention, psychological support and pregnancy counseling.
- Glucocorticoids (GCs), if clinically needed, regardless of patient’s disease manifestations, should be prescribed at the lowest possible dose and for the shortest period of time.
- All patients with lupus should receive antimalarials (AMs), except those who refuse them or who have absolute contraindications to take them
Recommendations by System
Cutaneous manifestations:
- Which is the best treatment for adult patients with different manifestations of cutaneous lupus?
- The panel suggests the standard of care (SOC( alone over adding other immunosuppressives (IS) in adult patients with SLE with cutaneous manifestations. It also suggests adding MTX, AZA, MMF, CsA, CYC or belimumab to patients failing to respond to SOC. Cost and availability may favor MTX and AZA.
Adult Kidney manifestations:
- Which is the best induction treatment for adult patients with lupus nephritis?
- The panel recommends AZA or MMF over CYC for maintenance in patients with SLE-related nephritis (strong recommendation). Cost and availability issues may favor AZA
Childhood-onset Lupus Manifestations:
- Which is the best induction treatment for childhood-onset lupus nephritis (cLN)?
- The panel suggests high-dose GCs plus MMF or CYC over high-dose GCs alone in patients with cLN as induction therapy. Cost and availability may favor CYC despite the risk of gonadal toxicity
- Which is the best maintenance treatment for childhood-onset lupus nephritis (cLN)?
- The panel suggests MMF or AZA over CYC for patients with cLN who responded, partially or completely, to induction therapy. Cost and availability may favor AZA
Cardiac manifestations:
- Which is the best treatment for adult patients with lupus-related acute pericarditis?
- The panel suggests SOC plus colchicine over SOC plus NSAIDs or belimumab for patients with acute SLE-related pericarditis
Pulmonary manifestations:
- Which is the best treatment for lupus-related diffuse alveolar hemorrhage (DAH)?
- The panel recommends that patients with SLE-related DAH be treated with intravenous GCs plus CYC and/or intravenous Ig and/or TPE and/or RTX over GCs alone (strong recommendation). Cost and availability may favor GC plus CYC
Neuropsychiatric manifestations:
- Which is the best treatment for adult patients with lupus-related severe, acute neuropsychiatric manifestations?
- The panel suggests using GCs plus CYC over GCs alone or GCs plus RTX for the treatment of severe neurologic manifestations in patients with SLE. Cost and availability may favor CYC
Haematological manifestations:
- Which are the best interventions for patients with severe acute lupus-related hemolytic anemia (hemoglobin ≤8 g/dL)?
- The panel suggests using high-dose GCs for patients with severe hemolytic anemia.
- Which are the best interventions for patients with severe lupus-related thrombocytopenia (platelet count ≤ 30 x10^9/L)?
- The panel suggests using high-dose GCs in patients with lupus with severe lupus thrombocytopenia.
Antiphospholipid syndrome:
- Which is the best treatment for adult patients with SLE with antiphospholipid syndrome (APS) and venous thromboembolic disease (VTD)?
- The panel recommends extended AC with vitamin K antagonist therapy for patients with APS with VTD (strong recommendation).
- Which is the best treatment for adult patients with SLE with APS and stroke?
- The panel suggests extended high-intensity (INR 3.0–4.0) over standard-intensity AC (INR 2.0–3.0) or LDA alone for patients with SLE with APS and stroke.
- Which is the best treatment for pregnant SLE women with antiphospholipid antibodies and recurrent pregnancy loss?
- The panel recommends HCQ plus LMWH plus LDA over HCQ plus LDA or adding GCs or intravenous Ig for pregnant patients with SLE with antiphospholipid antibodies and recurrent pregnancy loss (strong recommendation) based on moderate certainty of the evidence (LMWH plus LDA vs other alternatives) and very low certainty of the evidence (GCs and intravenous Ig vs other alternatives), since high certainty of harms related to GCs (increased premature delivery) and intravenous Ig (costs increase, burden related to drug administration) exists). It also suggests LMWH at a dose of 40 mg/day over UFH or higher doses of LMWH
Musculoskeletal manifestations:
- Which are the best treatment for adult patients with SLE and musculoskeletal (MSK) manifestations?
- The panel suggests SOC alone over adding other immunosuppressants (IS) in adult patients with SLE with MSK manifestations (weak recommendation based on the low certainty of the evidence). It suggests also adding either MTX, LFN, belimumab or ABT to those failing to respond to SOC (weak recommendation based on low to the moderate certainty of the evidence).

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd