- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
KDOQI clinical practice guideline for hemodialysis adequacy
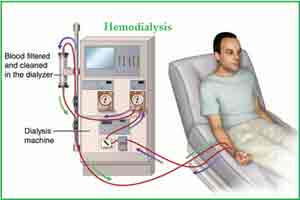
With the rising burden of CKD in the country, importance of Dialysis interventions cannot be undermined. At the same time, Interventions that can improve outcomes in dialysis are urgently needed. Attempts to improve outcomes have included initiating dialysis at higher glomerular filtration rates, increasing dialysis frequency and/or duration, using newer membranes, and employing supplemental or alternative hemofiltration
In November 2015, The National Kidney Foundation in the US produced clinical practice guidelines through the NKF Kidney Disease Outcomes Quality Initiative (NKF KDOQI). The guideline focused on answering the following main questions
(1) In patients with advanced chronic kidney disease (CKD), does initiating dialysis therapy earlier (as defined by higher glomerular filtration rate [GFR] at dialysis therapy initiation) improve outcomes?
(2) In hemodialysis patients, does more frequent hemodialysis (>3 times a week) improve outcomes compared to less frequent hemodialysis?
(3) In hemodialysis patients, does extended hemodialysis duration (>4.5-hour sessions) improve outcomes compared to usual-length hemodialysis duration?
(4) Do patients with extended (longer) or more frequent hemodialysis have greater blood pressure and volume control compared with patients with shorter or less frequent dialysis?
(5) In hemodialysis patients, do high-flux membranes improve patient outcomes when compared to low-flux hemodialysis?
Following are its major recommendations
Guideline 1: Timing of Hemodialysis Initiation
Patients who reach chronic kidney disease (CKD) stage 4 (glomerular filtration rate [GFR] <30 mL/min/1.73 m2), including those who have imminent need for maintenance dialysis at the time of initial assessment, should receive education about kidney failure and options for its treatment, including kidney transplantation, peritoneal dialysis (PD), hemodialysis in the home or in-center, and conservative treatment. Patients' family members and caregivers also should be educated about treatment choices for kidney failure.
The decision to initiate maintenance dialysis in patients who choose to do so should be based primarily upon an assessment of signs and/or symptoms associated with uremia, evidence of protein-energy wasting, and the ability to safely manage metabolic abnormalities and/or volume overload with medical therapy rather than on a specific level of kidney function in the absence of such signs and symptoms.
Guideline 2: Frequent and Long Duration Hemodialysis
In-center Frequent Hemodialysis
The Work Group suggests that patients with end-stage kidney disease be offered in-center short frequent hemodialysis as an alternative to conventional in-center thrice weekly hemodialysis after considering individual patient preferences, the potential quality of life and physiological benefits, and the risks of these therapies. (2C)
The Work Group recommends that patients considering in-center short frequent hemodialysis be informed about the risks of this therapy, including a possible increase in vascular access procedures (1B) and the potential for hypotension during dialysis. (1C)
Home Long Hemodialysis
Consider home long hemodialysis (6-8 hours, 3 to 6 nights per week) for patients with end-stage kidney disease who prefer this therapy for lifestyle considerations.
The Work Group recommends that patients considering home long frequent hemodialysis be informed about the risks of this therapy, including possible increase in vascular access complications, potential for increased caregiver burden, and accelerated decline in residual kidney function. (1C)
Pregnancy
During pregnancy, women with end-stage kidney disease should receive long frequent hemodialysis either in-center or at home, depending on convenience.
Guideline 3: Measurement of Dialysis: Urea Kinetics
The Work Group recommends a target single pool Kt/V (spKt/V) of 1.4 per hemodialysis session for patients treated thrice weekly, with a minimum delivered spKt/V of 1.2. (1B)
In patients with significant residual native kidney function (Kru), the dose of hemodialysis may be reduced provided Kru is measured periodically to avoid inadequate dialysis.
For hemodialysis schedules other than thrice weekly, the Work Group suggests a target standard Kt/V of 2.3 volumes per week with a minimum delivered dose of 2.1 using a method of calculation that includes the contributions of ultrafiltration and residual kidney function.
Guideline 4: Volume and Blood Pressure Control: Treatment Time and Ultrafiltration Rate
The Work Group recommends that patients with low residual kidney function (<2 mL/min) undergoing thrice weekly hemodialysis be prescribed a bare minimum of 3 hours per session. (1D) Consider additional hemodialysis sessions or longer hemodialysis treatment times for patients with large weight gains, high ultrafiltration rates, poorly controlled blood pressure, difficulty achieving dry weight, or poor metabolic control (such as hyperphosphatemia, metabolic acidosis, and/or hyperkalemia).
The Work Group recommends both reducing dietary sodium intake as well as adequate sodium/water removal with hemodialysis to manage hypertension, hypervolemia, and left ventricular hypertrophy. (1B) Prescribe an ultrafiltration rate for each hemodialysis session that allows for an optimal balance among achieving euvolemia, adequate blood pressure control and solute clearance, while minimizing hemodynamic instability and intradialytic symptoms.
Guideline 5: Hemodialysis Membranes
The Work Group recommends the use of biocompatible, either high or low flux hemodialysis membranes for intermittent hemodialysis. (1B)
You can read the full guidelines by clicking on the following link :
http://www.ajkd.org/article/S0272-6386(15)01019-7/pdf

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd