- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
IWGDF guidance on PAD Management in diabetic foot ulcer patients
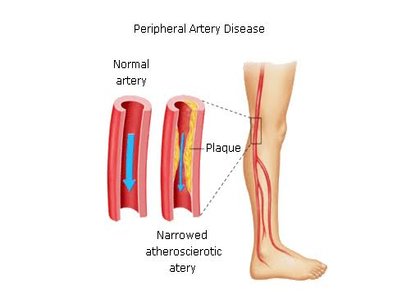
Peripheral artery disease (PAD) is a narrowing of the arteries other than those that supply the heart or the brain. When narrowing occurs in the heart it is called coronary artery disease while in the brain it is called cerebrovascular disease. Peripheral artery disease most commonly affects the legs, but other arteries may also be involved. The classic symptom is leg pain when walking which resolves with rest, known as intermittent claudication. Up to 50% of cases of PAD are without symptoms.
International Working Group on the Diabetic Foot IWGDF has guidance on the diagnosis, prognosis and management of peripheral artery disease in patients with foot ulcers in diabetes. Following are its major recommendations :
Key Recommendations
- Examine a patient with diabetes annually for the presence of peripheral artery disease (PAD); this should include, at a minimum, taking a history and palpating foot pulses. (GRADE strength of recommendation: strong; quality of evidence: low)
- Evaluate a patient with diabetes and a foot ulcer for the presence of PAD. Determine, as part of this examination, ankle or pedal Doppler arterial waveforms; measure both ankle systolic pressure and systolic ankle brachial index (ABI). (strong; low)
- We recommend the use of bedside non‐invasive tests to exclude PAD. No single modality has been shown to be optimal. Measuring ABI (with <0.9 considered abnormal) is useful for the detection of PAD. Tests that largely exclude PAD are the presence of ABI 0.9–1.3, toe brachial index ≥0.75 and the presence of triphasic pedal Doppler arterial waveforms. (strong; low)
- In patients with a foot ulcer in diabetes and PAD, no specific symptoms or signs of PAD reliably predict healing of the ulcer. However, one of the following simple bedside tests should be used to inform the patient and healthcare professional about the healing potential of the ulcer. Any of the following findings increases the pre‐test probability of healing by at least 25%: a skin perfusion pressure ≥40 mmHg, a toe pressure ≥30 mmHg or a transcutaneous oxygen pressure (TcPO2) ≥25 mmHg. (strong; moderate)
- Consider urgent vascular imaging and revascularisation in patients with a foot ulcer in diabetes where the toe pressure is <30 mmHg or the TcPO2 <25 mmHg. (strong; low)
- Consider vascular imaging and revascularisation in all patients with a foot ulcer in diabetes and PAD, irrespective of the results of bedside tests, when the ulcer does not improve within 6 weeks despite optimal management. (strong; low)
- Diabetic microangiopathy should not be considered to be the cause of poor wound healing in patients with a foot ulcer. (strong; low)
- In patients with a non‐healing ulcer with either an ankle pressure <50 mmHg or ABI <0.5, consider urgent vascular imaging and revascularisation. (strong; moderate)
- Colour Doppler ultrasound, computed tomography angiography, magnetic resonance angiography or intra‐arterial digital subtraction angiography can each be used to obtain anatomical information when revascularisation is being considered. The entire lower extremity arterial circulation should be evaluated, with detailed visualisation of below‐the‐knee and pedal arteries. (strong; low)
- The aim of revascularisation is to restore direct flow to at least one of the foot arteries, preferably the artery that supplies the anatomical region of the wound, with the aim of achieving a minimum skin perfusion pressure ≥40 mmHg, a toe pressure ≥30 mmHg or a TcPO2 ≥25 mmHg. (strong; low)
- A centre treating patients with a foot ulcer in diabetes should have the expertise in and rapid access to facilities necessary to diagnose and treat PAD; both endovascular techniques and bypass surgery should be available. (strong; low)
- There is inadequate evidence to establish which revascularisation technique is superior, and decisions should be made in a multidisciplinary team on a number of individual factors, such as morphological distribution of PAD, availability of autogenous vein, patient co‐morbidities and local expertise. (strong; low)
- After a revascularisation procedure for a foot ulcer in diabetes, the patient should be treated by a multidisciplinary team as part of a comprehensive care plan. (strong; low)
- Patients with signs of PAD and a foot infection are at particularly high risk for major limb amputation and require emergency treatment. (strong; moderate)
- Avoid revascularisation in patients in whom, from the patient perspective, the risk–benefit ratio for the probability of success is unfavourable. (strong; low)
- All patients with diabetes and an ischaemic foot ulcer should receive aggressive cardiovascular risk management including support for cessation of smoking, treatment of hypertension and prescription of a statin as well as low‐dose aspirin or clopidogrel. (strong; low)
To view full Guideline log on to : DOI: 10.1002/dmrr.2698
Cardiovascular RiskClopidogrelCoronary artery diseasediabetesdiabeticdiabetic foot ulcerDiagnosisfoot ulcerperipheral artery diseaserevascularisationvascular imaging
Next Story
NO DATA FOUND

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd