- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Intraocular lenses can benefit LASIK reject patients
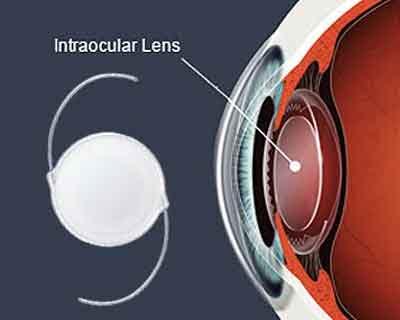
People who are unsuitable for LASIK because of moderate or extreme nearsightedness or severe astigmatism may benefit from a surgical procedure using intraocular lenses. Phakic intraocular collamer lenses, also called Phakic IOLs or ICLs, have been found safe and effective after five years, according to research presented at AAO 2016, the 120th annual meeting of the American Academy of Ophthalmology.
While laser vision correction procedures such as LASIK and photo refractive keratectomy or PRK have been successful for many patients, those who are extremely nearsighted or astigmatic often are unsuitable for these procedures. In recent years, Phakic ICL procedures were introduced to solve this problem. The technique uses lens replacements instead of lasers. To test the long-term safety and efficacy of the procedure, researchers at Iran University of Medical Sciences followed 31 people over five years to see how they fared following the procedure. They found that the Phakic ICL procedure was safe and effective for the majority of patients.
Researchers studied 60 eyes in 31 people who had Phakic ICLs to correct moderate to extreme levels of myopia or severe astigmatism. They chose people based on a number of factors, including those whose vision was stable, who were not correctable with LASIK surgery and had no eye disorders, such as glaucoma or macular degeneration.
Prior to the procedure, all of the people had 20/200 vision or worse and only 60 percent could achieve 20/40 eyesight even with glasses or contact lenses. Five years after having the procedure, the results were as follows:
•Fifty-seven percent of eyes (34 eyes) achieved 20/40 vision without the use of glasses or contact lenses.
•Another 23 percent of eyes (14 eyes) achieved it with the addition of glasses or contacts. The researchers say that this is still a positive outcome since none of the study participants could achieve 20/40 vision with glasses or contacts prior to having the procedure.
•Additionally, 20 percent (12 eyes) of recipients achieved corrected visual acuity of 20/50 to 20/120 that related to underlying retinal problems but had better vision than before surgery.
•Forty-two eyes were able to read at least one or more additional lines on the chart than they could read before the procedure when they were wearing their glasses or contact lenses.
•All of the lenses remained clear after five years, and none of the people who had the surgery lost visual acuity.
In terms of side effects and complications, researchers found two eyes needed realignment. Endothelial cell count decreased 11 percent. Endothelial cells line the inside of the cornea and help keep it clear. Over time, the loss of these cells can increase the chance of the cornea clouding and is a potential risk of any intraocular lens surgery. The 11 percent decrease is within a range that the technique is considered safe, researchers said. Further, the amount of endothelial cell lost decreased in those who received a newer design of Phakic lenses beginning in 2014, said researchers.
"The main concerns for this type of procedure are early and late complications," said Seyed Javad Hashemian, M.D., lead author of the study and director of the cataract and refractive unit at Rassoul Akram Hospital and Iran University of Medical Sciences, Tehran. "This study shows that if we have a complete pre-operative evaluation and choose those who are most likely to be the best candidates for the procedure, Phakic ICL implantation can improve quality of vision and function."
The researchers noted that larger studies should be done to verify their findings.
Long-term Outcomes and Complications of Posterior Chamber Phakic Intraocular Lens Implantation for the Correction of High Myopia and Astigmatism (5 Years Study) is being presented at AAO 2016, the 120th annual meeting of the American Academy of Ophthalmology.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd