- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Hydrocortisone,fludrocortisone combo reduces mortality in septic shock
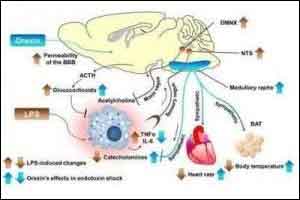
Septic shock is characterized by dysregulation of the host response to infection, with circulatory, cellular, and metabolic abnormalities.Dr. Djillali Annane and colleagues conducted a double-blind, randomized trial to evaluate whether therapy with hydrocortisone plus fludrocortisone can modulate the host response and improve the clinical outcomes of patients with septic shock.The researchers found that combination treatment with hydrocortisone plus fludrocortisone reduces 90-day all-cause mortality in patients with septic shock.The study has been published in New England Journal of Medicine.
The researchers randomized 1,241 patients in a two-by-two factorial design to receive hydrocortisone-plus-fludrocortisone therapy, drotrecogin alfa (activated), the combination of the three drugs, or their respective placebos. The primary endpoint was 90-day all-cause mortality. Secondary endpoints included mortality at intensive care unit (ICU) discharge and hospital discharge and at day 28 and day 180, and the number of days alive and free of vasopressors, mechanical ventilation, or organ failure.Following the withdrawal of drotrecogin alfa (activated) from the market, the trial continued with a two-group parallel design. Analysis compared patients who received hydrocortisone plus fludrocortisone with those on placebo.
The 90-day mortality rate were 43.0 percent (264 of 614 patients) in the hydrocortisone-plus-fludrocortisone group and 49.1 percent (308 of 627 patients) in the placebo group (p=0.03). The relative risk of death in the hydrocortisone-plus-fludrocortisone group was 0.88 (95 percent CI, 0.78–0.99).
The researchers found mortality was significantly lower with hydrocortisone–fludrocortisone vs placebo at ICU discharge (35.4 percent vs 41.0 percent; p=0.04), hospital discharge (39.0 percent vs 45.3 percent; p=0.02) and day 180 (46.6 percent vs 52.5 percent; p=0.04), but not at day 28 (p=0.06).
The hydrocortisone-plus-fludrocortisone group showed a significantly higher number of vasopressor-free days to day 28 (17 vs 15 days; p<0.001) and a number of organ-failure-free days (14 vs 12 days; p=0.003) compared with the placebo group.
On the other hand, no between-group differences were observed in the number of ventilator-free days (11 days in the hydrocortisone-plus-fludrocortisone group vs 10 days in the placebo group; p=0.07) and in the rate of serious adverse events, although hyperglycaemia was more common with hydrocortisone-plus-fludrocortisone treatment.
The authors concluded that septic shock, 90-day all-cause mortality was lower among those who received hydrocortisone plus fludrocortisone than among those who received placebo. The present data suggest that 7-day treatment with a 50-mg intravenous bolus of hydrocortisone every 6 hours and a daily dose of 50 μg of oral fludrocortisone may help lower mortality at day 90 and at ICU and hospital discharge in adults with septic shock, researchers said.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd