- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Guideline for Management of Acute Encephalitis Syndrome: Ministry of Health & Family Welfare
Muzaffarpur district in Bihar has seen a massive outbreak of Acute Encephalitis Syndrome or Chamki fever. The recent data estimated the death of more than 140 children in Bihar’s Muzaffarpur district due to Acute Encephalitis Syndrome.
More than 400 children with AES have been admitted to various hospitals. Most of the deaths have been attributed to low blood sugar level (hypoglycemia).
The Ministry of Health & Family Welfare of India has released guidelines for management and cure of Acute Encephalitis Syndrom.
According to the guideline, a case of AES is defined as a person of any age, at any time of year with the acute onset of fever and a change in mental status (including symptoms such as confusion, disorientation, come, or inability to talk) AND/OR new onset of seizures (excluding simple febrile seizures). Other early clinical findings may include an increase in irritability, somnolence or abnormal behavior greater than that seen with usual febrile illness.
Case definition of Acute Encephalitis Syndrome (AES)
Clinically, a case of AES is defined as a person of any age, at any time of year with the acute onset of fever and a change in mental status (including symptoms such as confusion, disorientation, come, or inability to talk) AND/OR new onset of seizures (excluding simple febrile seizures). Other early clinical findings may include an increase in irritability, somnolence or abnormal behaviour greater than that seen with usual febrile illness.
Case classification
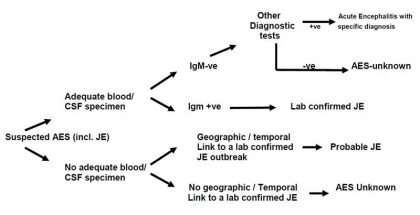
A case that meets the clinical case definition for AES i.e. suspected case should be classified in one of the following four ways see Figure 1):
- Laboratory-confirmed JE: A suspected case that has been laboratory-confirmed as JE.
- Probable JE: A suspected case that occurs in close geographic and temporal relationship to laboratory-confirmed case of JE, in the context of an outbreak.
- "Acute encephalitis syndrome" (due to agent other than JE): A suspected case in which diagnostic testing is performed and an etiological agent other than JE virus is identified.
- "Acute encephalitis syndrome" (due to unknown agent ) A suspected case in which no diagnostic testing is performed or in which testing was performed but no etiological agent was identified or in which the test results were indeterminate.
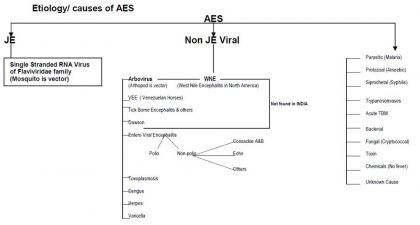
Japanese Encephalitis (JE) is a mosquito borne zoonotic viral disease is one of the causes under AES. The virus is maintained in animals and birds. Pigs and birds, particularly the birds belonging to Family Ardeidae (e.g. cattle egrets, pond herons, etc.) are the natural hosts. Pigs and wild birds are reservoir of infection and are often called as amplifier hosts in the transmission cycle, while man and horse are dead end hosts.
Similarly other virus, fungus, parasite, spirochetes, toxin etc may cause similar illness. The disease affects the central nervous system and can cause severe complications, seizures and even death. The case fatality rate of this disease is very high and those who survive may suffer with various degrees of neurological sequelae.
Children suffer the highest attack rates because of lack of cumulative immunity due to natural infection.
Meningitis, caused by bacteria, can be treated as soon as possible with antibiotics. Encephalitis, usually caused by a virus, cannot be treated with antibiotics. However, good clinical management is important to reduce the risk of disability or death from the
disease.
Clinical involvement of the Central Nervous System (CNS) is an unusual manifestation of human viral infection. The spectrum of brain involvement and the outcome of the disease are dependent on the specific pathogen, the immunological state of the host and a range of environmental factors. Although specific therapy is limited to only several viral agents, correct diagnosis, and supportive and symptomatic treatment (when no specific therapy is available) are mandatory to ensure the best prognosis.
DIAGNOSIS OF JAPANESE ENCEPHALITIS
Clinical Manifestations
- Following an incubation period, in case of viral encephalitis including JE a prodrome of fever, headache, nausea, diarrhoea, vomiting, and myalgia occurs lasting for few days (1-5 days) followed by irritability, altered behaviour, convulsions and coma.
- The progression of disease is rapid. Signs of raised intra cranial tension are commonly present in acute stage of illness.
- The patient may develop difficulty of speech and other neurological deficits like ocular palsies, hemiplegia, quadriplegia and extrapyramidal signs in the form of dystonia, choreoathetosis and coarse tremors.
- All the cases of Acute CNS involvement are reported in the syndrome of acute encephalitis i.e. all cases of Acute Encephalitis Syndrome (AES) should be reported as they have similar clinical manifestations.
- Their case management usually follows a common protocol along with situation specific treatment. Diagnosis of JE will depend on laboratory investigations.
- The case definitions and case classification in the program are given in the following paragraphs.
Case Classification:
- Laboratory-Confirmed case : A suspected case with any one of the following markers:
- Presence of lgM antibody in serum and/ or CSF to a specific virus including JE/Entero Virus or others
- Four fold difference in lgG antibody titre in paired sera
- Virus isolation from brain tissue
- Antigen detection by immunofluroscence
- Nucleic acid detection by PCR
In the sentinel surveillance network, AES/JE will be diagnosed by lgM Capture ELISA, and
virus isolation will be done in National Reference Laboratory.
Probable Cases
Suspected case in close geographic and temporal relationship to a laboratory-confirmed case of AES/JE in an outbreak
FIGURE 1 : FINAL CLASSIFICATION SCHEME FOR AES CASES
 While the above classifications are useful for clearer definitions of AES cases, for practical purposes, the two key definitions to be used are ìSuspected JE Casesî for those that meet the criteria for AES, and ìconfirmed JE casesî for those AES cases which have laboratory confirmation for JE.
While the above classifications are useful for clearer definitions of AES cases, for practical purposes, the two key definitions to be used are ìSuspected JE Casesî for those that meet the criteria for AES, and ìconfirmed JE casesî for those AES cases which have laboratory confirmation for JE.Acute Encephalitis Syndrome due to other agents
A suspected case in which diagnostic testing is performed and an etiological agent other than AES/JE is identified
Acute Encephalitis Syndrome due to an unknown agent
A suspected case in which no diagnostic testing is performed / no etiological agent is identified / test results are indeterminate
EC includes only 2 diseases. JE and Epidemic Brain Attack (EBA)/ Non JE, AES. Diagnosis: EBA can be easily differentiated from JE with the help of the following Table
Differentiation of Japanese Encephalitis and Epidemic Brain Attacks/ NON-JE, AES
| Japanese Encephalitis | Epidemic Brain Attack (EBA) or Non JE/ AES | |
| Relation to onset of Rains | About 6 weeks after onset of rains | Starts within 3 days after the onset of rains |
| Pain in abdomen | No | in 50% |
| Diarrhea | No | in 50% |
| CSF | lymphocytic pleocytosis | normal except for increased tension |
| CT scan | Thalami hypodense | Infarct in Middle cerebral artery territory |
| MRI scan | Thalami hyperintense | Infarct in Middle cerebral artery territory |
3. MANAGEMENT OF ACUTE ENCEPHALITIS SYNDROME (AES) INCLUDING JAPANESE ENCEPHALITIS
Danger Sign & Line of Treatment
Management of Acute Encephalitis Syndrome including Japanese Encephalitis is essentially symptomatic. To reduce severe morbidity and mortality, it is important to identify early warning signs and refer patents to the health facility and educate the health workers about the first line if management at the grassroots level. Chart 1 depicts what is to be done for a patient at the community level.
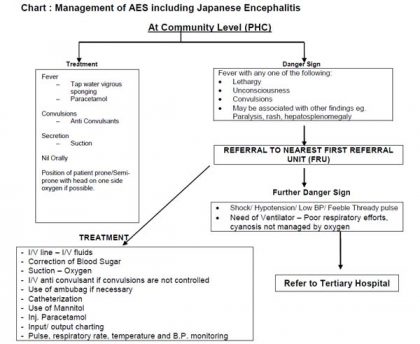
MANAGEMENT OF CASES OF AES INCLUDING JE
Treatment at the health facility, it is important to exclude other causes of CNS affliction like meningitis or cerebral malaria which require specific treatment. Treatment will depend on the condition in which the patient is received in the health facility. Since patients are likely to arrive with high-grade fever and change in mental status or convulsions proceed with the assessment of patency of the airway.
The treatment at PHC/ CHC District level or at tertiary care hospitals remains the same. Depending upon the needs of care and availability of facilities available at the center/ hospital the patients to be transferred to the nearest higher center for further management. It should be ensured before transferring the case, all the available treatment is provided to the patient. Only needy patients where such facilities are not available, to be transported. The time consumed in transportation itself is a major cause of the high mortality rate.
In all endemic areas, all the facilities including training can be arranged before hand except Ventilatory Support. All Centres should be equipped with ambu beg and oxygen in addition to other medicines and I/V cannula.
The treatment of the patients may require, as follow:-
- Management of Airways and Breathing.
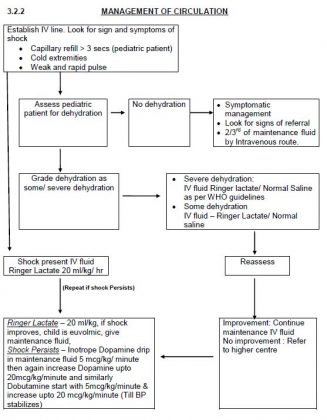
- Management of Circulation.
- Control of Convulsion and Intracranial pressure
- Control of Temperature
- Fluid and Electrolytes and Calories/ Nutrition
- General management
- Specific treatment of any for a treatable cause
- Investigations, Samples Collection & Transportation
- Reporting of a case
- Rehabilitation
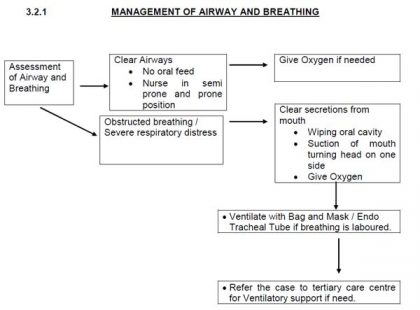
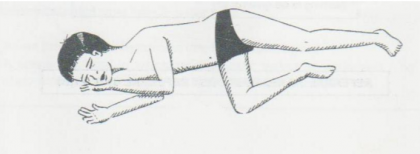
Fig 1. Position of the Patient
- Turn the patient on the prone side to reduce the risk of aspiration.
- Keep the neck slightly extended and stabilize by placing cheek on one hand.
- Bend one leg to stabilize the body position.
Indications of Ventilatory Support
- Detoriating General Condition
- Very Shallow Respiration/ Severe Respiratory Distress/ Heart Sound are Feeble
- Capillary Refilling time/ colour of Patient Not Improved
- Dusky Colour of body/ Cyanosis
- Needs continuous Bag and Mask (Ambu) respiration
- ABG Parameters
 NB: These are broad guidelines; ultimate decision regarding management will depend upon the attending physician.
NB: These are broad guidelines; ultimate decision regarding management will depend upon the attending physician.MANAGEMENT OF CONVULSIONS & I.C.T
Give anticonvulsants if there was a history of convulsions and not given earlier, or convulsions are present. Number one to three are first drug of choice, if convulsions are not controlled.
Anti Convulsants
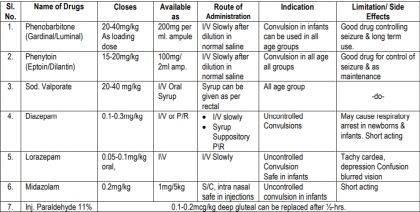
Maintenance Dose
- Phenobarbitone 3-8mg/kg/day I/V or oral
- Phenytoin 5-8 mg/kg/day I/V or oral
- Sodium Valproate 40-60mg/kg/day Oral
MANAGEMENT OF INCREASED INTRACRANIAL PRESSURE (Tension)
(Only after correction of Dehydration)
- Mannitol 20% I/V ñ 5 ml/kg in ½ hrs as 1 st dose than 2.5 ml/kg at 6 hrs. intervals upto 48 hours (8 doses).
- 2. Injection Lasix I/V ñ 1 mg /kg upto 40 mg can be given.
- 3. Glycerol solution:- Oral ñ 0.5 ml/kg mix with fruit juice can be given by nasogastric tube ñ 3 times a day
- 4. Steroids ñ are not indicated in viral encephalitis including JE
CONTROL OF TEMPERATURE
If No Rigors:-
a) Tap Water Sponging: Not only on the forehead, palms or soles, but the whole body to be wet with water and fan (ceiling/table/manual) is also on. Cold sponging is harmful.
b) If the temperature is too high ñ Cold Sponges may be kept on head, axilla, and groins.
c) Injection Paracetamol: 5mg/kg, deep intramuscular at either lateral side of the thigh or upper outer Quadrant of the hip. If the injection is not available, give Paracetamol 10- 15mg/kg maximum up to 600 mg by Nasogastric tube. Paracetamol Suppository are also available which may be used. Other antipyretic medicines e.g. nemusulide/ brufen/ meftal/ aspirin etc are not advisable, specially in children.
If chills or Rigors present :
- Donít cover patients
- Donít do water sponging
- Use Paracetamol injection, syrup, through nasogastric tube or Paracetamol suppository as advised above
MANAGEMENT OF FLUID ELECTROLYTES AND CALORIES/NUTRITION
A) Assessment of Dehydration and Management
1. Dehydration
Dehydration is classified into No/ Some/ Severe Dehydration. Since it is difficult to assess dehydration in a patient of encephalitis as the patient is lethargic and unable to drink,. therefore, skin turgor takes precedence over other signs. An objective way of classification would be as follows:
(i) Some Dehydration:
- Irritability
- Thirsty
- Sunken Eyes
- Less Tears
- Dry Mouth
- Skin Turgor Delay
(ii) Severe Dehydration:
- Floppiness
- Drowsiness/ Lethargy
- Unconscious
- Inability to Drink
(iii) Signs of shock
- Oliguria/ anuria
- Rapid and thready pulse
- Capillary filling time > 3secs
- Low Blood Pressure
Management of Dehydration:
(a) Some Dehydration:
- IV fluid Ringer lactate/ N saline 100m/kg to be given over 8 hrs.
- Where the facility for IV fluids is not available administer ORS 75m/kg in 4 hrs through nasogasrtic tube
- Reassess: if there is improvement continue with maintenance IV fluid/if no improvement is detected, switch to plan for severe dehydration
(b) Severe Dehydration
- IV fluid Ringer lactate 100ml/kg is given as per the table below Table 1:
| Rate of Fluid (Ringer Lactate) | 30ml/kg | 70ml/kg |
| < 1yr | 2 hrs | 4 hrs |
| < 1yr | 1 hrs | 5 hrs |
- Reassess: If there is improvement switch to maintenance/ if no improvement is detected or deterioration is observed infuse IV fluid more rapidly.
2. Maintenance
Maintenance fluid is administered at the following rate Table 2:
| Weight | Fluid Volume |
| 1 - 10 | 10 ml / kg |
| 11 - 20 | 1000 ml + 50cc/kg over & above 10 kg |
| 21 - 40 | 1500 ml+20cc/kg over & above 10 kg |
(B) Calories/ Nutrition
During CNS infections and convulsion and hyperphyrexia state, calories specially glucose required is increased and it should be given in form of 10% Dextrose or even 25% Dextrose may be given on arrival of the patient. A total dose of 200 mg/kg may be given. All I/V fluids with Dextrose should be continued till patient is stabilized, convulsions are controlled, no vomiting and distention of abdomen, at this time, intra gastric feeding may added and slowly I/V fluids are replaced by total nasogastric feeding.
GENERAL MANAGEMENT
Suction: Frequent suction either by mucous sucker, or suction machine to be done on an unconscious patient, so secretion may not collect in mouth to avoid aspiration and maintenance the patency of airways.
Nasogastric Aspiration: Nil orally, place a Nasogastric/ Ryles tube into stomach and do a frequent suction to avoid any vomiting and aspiration. It will also help in decompensation of stomach and decrease intra abdominal pressure. It will help in respiration.
Care of Eye, Bowel Bladder & Back:
- Eyes to be covered by wet gauge
- An antibiotic Eye ointment may be applied twice a day or liquid paraffin may be
- put in eyes to avoid drying of Cornea.
- If child does not pass stool, put a glycerine enema.
- Bed should be well maintained, dont allow to form any bed sore.
- Spirit & powder may be applied on back and on all pressure points.
- Frequent changing of patients position.
- Catheterize the patient to avoid soiling of beds.
- Physiotherapy once patient is stabilized
- Other General Nursing Care
- Treat Secondary infections by appropriate antibiotics
- Treat underlying other pathology e .g. anemia, malnutrition, etc.
TREATMENT OF SPECIFIC CAUSE IF ANY
- Herpes - Acyclovir 10 mg/kg/dose, slowly over a period of one hour 8 hourly X 21 days.
- Zoster Varicella - Acyclovir 10mg/kg/dose, 1/2hrs slowly, over a period of 1 hour 8 hourly X 2-3 weeks.
- Malaria - I/V Quinine 20 mg/kg in 5% Dextrose slowly over a period of 1hr then 10mg/kg 8 hourly. Monitor Blood Sugar and Blood Pressure.
- Meningitis (Pyogonic) - Start with inj. Ampicillin 400 mg kg 6 hourly upto 12gm/day
+
Inj. Ceftrioxone 100-150mg/kg as stat dose than in two dived doses 12 hourly
+
Steroid Change antibiotics according to C/S report and response. - TBM - Anti Tubercular Drugs (1NH, PZA, Rcin + Ethambutol + Steroids)
- Toxoplasmosis - Pyrimethamine 2mg/kg/24 hours in two divided doses X 2 days than 1mg/kg/ on alternate day.
- Amoebiasis - Metronidazole 10mg/kg I/V slowly 8 hourly X 10-14 days.
- Fungal Infection - Inj. Amphotericin B 5mg/kg/24 hours or Fluconazole oral 200-400mg/kg for 3-6 months.
- Neurocysticercosis - Albendazole oral 10/mg/kg(upto 400 mg)/day X 2
weeks.
INVESTIGATIONS, SAMPLE COLLECTION & TRANSPORTATION
Investigations
- Complete blood counts
- Peripheral blood smear-Malarial parasite
- Blood glucose, Electrolytes
- CSF and Blood for serology by lgM ELISA/ virus isolation, CSF is preferred since by the time patient presents with CNS manifestations the level of viremia in blood has decreased and there is cross reaction with other flaviviruses.
- Other test if necessary LFT/KFT/Blood Culture/X-ray/Ultrasound/ CT/MRI/ECHO/ any specific test Enzyme/ECG/EEG/Suspected Etiology
Specimen Collection
Blood(serum) and CSF specimen are to be collected. Blood specimen should be collected within 4 days after onset of illness for isolation of virus and at least 5 days after onset of illness for detection if 1g M antibodies. A second convalescent sample should be collected 10-14 days after the first sample.
Blood/Seru
i) Equipment required
- 5ml vacutainer tube(non-heparinized) with 23g needle/5ml syringe with needle
- 5ml blood collection tube if syringe and needle are used for blood collection
- Disposable gloves and face mask
- Tourniquet
- Sterlized swabs
- Sterile serum storage vial
- Specimen labels, marker pen
- Band aid
- Zip lock plastic bags
- Lab request form
- Cold box(vaccine carrier) with ice pack
- First- aid kit
ii) Collection procedure
- Collect 5ml blood in a sterile tube labelled with patient identification and date of collection.
- Keep at room temperature till clot retracts from serum.
- Blood can be stored at 4-8o celsius for 24hrs before serum is separated, do not freeze whole blood.
- Transport whole clotted blood specimen to laboratory on ice if it can reach lab in 24 hrs/centrifuge at 1000rpm for 10mins to separate the serum or if centrifuge is not available carefully remove serum with a pipette and transfer serum to a sterile vial and store at 4-8o C.
C. Transportation
- Specimen should be transported to laboratory as soon as possible, do not
wait for collection of additional specimen. - Put specimen in zip pouch/plastic bag with absorbent material(cotton/tissue)
- Use vaccine carrier/thermos flask for transport. In vaccine carrier use frozen packs along the sides and place specimen in the centre. Transport as in reverse cold chain.
- Place lab request form in a plastic bag and tape to inside of carrier
- Inform the lab about the time and manner of transportation
- Transport the serum on wet ice within 48hrs or it can be stored at 4-8o C for 7 days.
- If a delay is anticipated sera should be frozen at - 20o C and transported on
- frozen ice packs. Repeated freezing and thawing should be avoided as it affects the stability of IgM.
Lumbar Puncture & CSF Examination
All attempts should be made to collect CSF specimens for confirmation of diagnosis.
i) Collection
- Lumbar puncture is the most commonly used means of collecting
specimen - Patient is positioned on his side with knees curled up to his abdomen, occasionally it is performed with the patient sitting or bent forward.
- Skin is scrubbed and local anesthetic is injected over lower spine. Spinal needle is inserted usually between L3 and L4 vertebrae.
- Once the needle is in supra-archnoid space pressure can be measured and fluid is collected. Usually 2-3 ml of fluid is collected in a sterile screw capped bottle.
- After sample is collected, the needle is removed and area is cleaned.
- Patient is advised to lie flat for 6-8 hrs.
- Perform physical examination of CSF, indicate the findings on the laboratory requisition form and transport to the laboratory as soon as possible. Store at 4 C if delay in processing is anticipated.
ii) Storage and Transportation
- Store at 4 C as soon as possible after collection and dispatch at the earliest on wet ice in vaccine carrier/thermo flask.
- Hands carry the specimen to laboratory preferably due to urgency.
- For PCR transport specimen on dry ice.
A designated person should be responsible for storage, packing, and transportation as per national guidelines.
REHABILITATION
- Physiotherapy/ PMR
- Advice of Pediatric Neurologist
- Correction to fix deformity by Orthopaedic Surgeon
- Child Psychologist advice
- Various prosthesis
- Artificial appliances
REPORTING OF A CASE
It is very important to report all the suspected cases of AES or JE to the appropriate health authorities to prevent further spread of disease.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd