- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
First AI based medical device to detect diabetic retinopathy approved
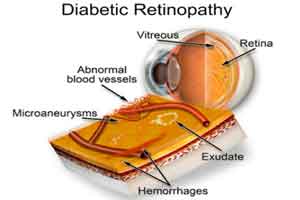
The IDx-DR device, from IDx LLC, is the first device which has been authorized for marketing by U.S. Food and Drug Administration that provides a screening decision without the need for a clinician to interpret the image or results. It can be used by healthcare providers who may not normally be involved in eye care in Primary care. It is the first medical device to use artificial intelligence to detect greater than a mild level of the eye disease diabetic retinopathy in adults who have diabetes. IDx-DR was granted Breakthrough Device designation, meaning the FDA provided intensive interaction and guidance to the company on efficient device development, to expedite evidence generation and the agency’s review of the device.
To qualify for such designation, a device must provide for more effective treatment or diagnosis of a life-threatening or irreversibly debilitating disease or condition, and meet one of the following criteria: the device must represent a breakthrough technology; there must be no approved or cleared alternatives; the device must offer significant advantages over existing approved or cleared alternatives; or the availability of the device is in the best interest of patients.
“Early detection of retinopathy is an important part of managing care for the millions of people with diabetes, yet many patients with diabetes are not adequately screened for diabetic retinopathy since about 50 percent of them do not see their eye doctor on a yearly basis,” said Malvina Eydelman, M.D., director of the Division of Ophthalmic, and Ear, Nose and Throat Devices at the FDA's Center for Devices and Radiological Health. “Today’s decision permits the marketing of a novel artificial intelligence technology that can be used in a primary care doctor’s office. The FDA will continue to facilitate the availability of safe and effective digital health devices that may improve patient access to needed health care.”
The device, called IDx-DR, is a software program that uses an artificial intelligence algorithm to analyze images of the eye taken with a retinal camera called the Topcon NW400. A doctor uploads the digital images of the patient’s retinas to a cloud server on which IDx-DR software is installed. If the images are of sufficient quality, the software provides the doctor with one of two results: (1) “more than mild diabetic retinopathy detected: refer to an eye care professional” or (2) “negative for more than mild diabetic retinopathy; rescreen in 12 months.” If a positive result is detected, patients should see an eye care provider for further diagnostic evaluation and possible treatment as soon as possible.
IDx-DR is the first device authorized for marketing that provides a screening decision without the need for a clinician to also interpret the image or results, which makes it usable by health care providers who may not normally be involved in eye care.
The FDA evaluated data from a clinical study of retinal images obtained from 900 patients with diabetes at 10 primary care sites. The study was designed to evaluate how often IDx-DR could accurately detect patients with more than mild diabetic retinopathy. In the study, IDx-DR was able to correctly identify the presence of more than mild diabetic retinopathy 87.4 percent of the time and was able to correctly identify those patients who did not have more than mild diabetic retinopathy 89.5 percent of the time.
Patients who have a history of laser treatment, surgery or injections in the eye or who have any of the following conditions should not be screened for diabetic retinopathy with IDx-DR: persistent vision loss, blurred vision, floaters, previously diagnosed macular edema, severe non-proliferative retinopathy, proliferative retinopathy, radiation retinopathy or retinal vein occlusion. IDx-DR should not be used in patients with diabetes who are pregnant; diabetic retinopathy can progress very rapidly during pregnancy and IDx-DR is not intended to evaluate rapidly progressive diabetic retinopathy. IDx-DR is only designed to detect diabetic retinopathy, including macular edema; it should not be used to detect any other disease or condition. Patients will still need to get a complete eye examination at the age of 40 and at the age of 60 and also if they have any vision symptoms (for example, persistent vision loss, blurred vision or floaters).

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd