- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Eye-dwelling bacteria help mice fight off invading pathogens
The surface of the eye is one of the most inhospitable environments for microbes in the mammalian body, because tears are loaded with anti-microbials. However, some microbes can live on this sparsely populated tissue and may play a key role in preventing eye infection. NIH researchers reporting in the journal Immunity found that Corynebacterium mastitidis dwells on the eyes of laboratory mice, and that mice with Corynebacterium could fend off invading pathogenic microbes better than mice without it.
"People have been finding bacterial DNA on the human eye but no one has presented experimental proof that these bacteria actually live there," says senior co-author Rachel Caspi, an immunologist at the National Eye Institute, National Institutes of Health (NIH). "For all we know, these bacteria may have 'crash landed' on the eye and were killed by the anti-microbials in tears or patrolling immune cells. Finding a bug that persists there long term was a bit of a surprise. We were looking for it but not necessarily expecting it."
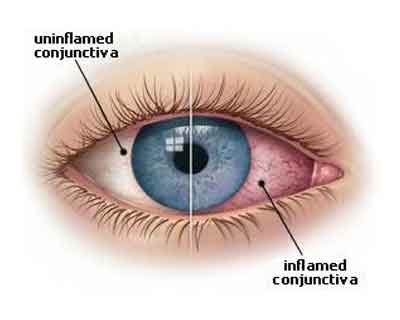
The NIH investigation began with a strain of lab mice that develop nasty bacterial conjunctivitis also known as "pink eye" where the thin mucous membranes that line the inside of the eyelid and cover the whites of the eyes, or "conjunctiva," become inflamed. These mice lack an immune molecule called IL-17, which summons immune cells to areas of infection. The researchers hypothesized that in common strains of mice, a commensal microbe on the surface of the eye might be setting off an IL-17 response to protect from harmful infection.
To find out which bacterial species lived on the eyes of their mice, the researchers swabbed samples from the conjunctiva of their mice across a petri dish and waited to see what grew, but even so, they would have missed Corynebacterium mastitidis if not for luck. "We accidentally forgot a Ppetri dish in the anaerobic chamber for a week," says first author and NIH postdoc Anthony St. Leger. "Only then did we discover this slow growing bug."
Further experiments established that the Corynebacterium could cause immune cells from the conjunctiva to release IL-17.Tears from mice with Corynebacterium living in their conjunctivae were more deadly to the pathogens Candida albicans and Pseudomonas, both of which can cause loss of vision when they infect the eye. When the researchers directly inoculated eyes of mice not harboring pathogenic bacteria, those mice also began producing higher levels of IL-17, leading the researchers to conclude that Corynebacteria mastitidis was helping the mice maintain immunological balance in the eye. When the newly colonized mice were exposed to Candida and Pseudomonas, they were able to resist the infection.
These results challenge the notion that the surface of the eye doesn't have any full-time microbial residents. "We know that C. mastitidis must be a 'permanent resident' as opposed to a 'guest' because it has to be instilled onto the eye, or acquired from the mother in infancy. It does not transfer from one adult mouse to another in the same cage, even after weeks of co-housing," says St. Leger.
"By virtue of being there, this commensal stimulates a level of local tissue immunity that keeps it under control, and at the same time it also prevents pathogenic agents from getting a foothold. But if your immune system is either over-reactive or under-reactive, so that the response to the commensal is abnormal, you can get in trouble," says Caspi.
Human studies are finding abundant Corynebacterium DNA sequences in samples from healthy people's eyes, but some strains of Corynebacterium may also cause eye infections in the immunocompromised and the elderly and one study found that a strain of Corynebacterium mastitidis can be an opportunistic pathogen on human skin.
The researchers' next steps will include finding out more about how these and other bacteria stimulate the local immune response and looking for other bacteria that may also live on the eye. "We don't think that C. mast is the only commensal. This is a proof of concept," says Caspi. "There's no question in our minds that other commensals will also be found at the ocular surface."

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd