- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Enhanced MRI of brain and spine must for early diagnosis of Bing–Neel syndrome
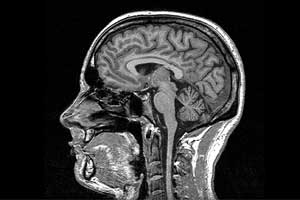
Bing–Neel syndrome (BNS) is a rare neurological complication of Waldenström’s macroglobulinemia. Aikaterini Fitsiori, University Hospital of Strasbourg, Strasbourg, France, and colleagues conducted a study to describe the spectrum of radiological manifestations of this syndrome and their prevalence in order to facilitate its early diagnosis.
Findings of the study published in the journal European Radiology, demonstrate that diagnosis of BNS remains challenging. Central nervous system MRI findings in the setting of known or suspected Waldenström’s macroglobulinemia appear to be highly suggestive of BNS and appropriate imaging protocols are required for their depiction.
For the study, the researchers retrospectively examined the medical records of twenty-four patients with BNS that diagnosed between 1994 and 2016 in eight centers in France, as well as the corresponding literature, focusing on imaging studies. Recorded data were statistically analyzed and radiological findings described.
The mean age of our patients was 62.4 years (35-80 years). The vast majority of patients were men, with a male to female ratio of 9:1. Findings included parenchymal or meningeal involvement or both.
Key Findings:
- The most common finding was leptomeningeal infiltration, either intracranial or spinal, with a prevalence reaching 70.8%.
- Dural involvement was present in 37.5% of patients.
- In 41.7% (10/24) of patients, there was parenchymal involvement with a higher prevalence of brain comparing to medullar involvement (33.3% and 23.1% respectively).
- A high T2 signal of the parenchyma was identified in 41.7% of patients and high signal in diffusion was evident in 25% of them.
- Intraorbital or periorbital involvement was also detected in four cases.
A proposition regarding the appropriate imaging protocol completed the study.
"Diagnosis of Bing-Neel syndrome remains challenging and recent expert recommendations include MRI in the diagnostic criteria for the syndrome," wrote the authors. "The most common radiological manifestations of BNS are leptomeningeal/dural infiltration or parenchymal involvement of brain or spinal cord, but many atypical forms may exist with various presentations."
"Appropriate imaging protocol for BNS should include enhanced MRI studies of both brain and spine," concluded the authors.
For further reference log on to https://doi.org/10.1007/s00330-018-5543-7

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd