- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Empyema Thoracis in children : Govt. of India Guideline
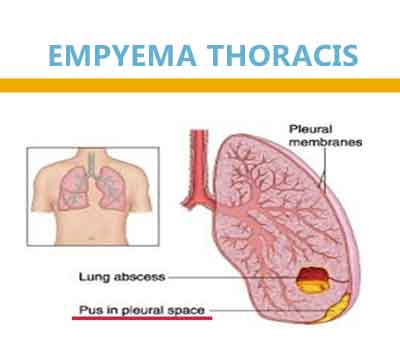
Empyema thoracis constitutes 5-10 % cases seen by a paediatrician in our country.The government of India has released its Guidelines for Empyema Thoracis in children.
‘Empyema’ is a term derived from the Greek verb ‘empyein’ ( to suppurate ) & literally refers to frank pus in the pleural space. It could be localised or free collection of purulent material in pleural space as a result of combination of inoculation of bacteria & culture medium of pleural fluid.Pleural space infection is a continuum but classically has been divided into three stages :Stage 1 or Exudative or Acute phase ( lasts upto 3 days ) : The inflammatory process associated with the underlying pneumonia leads to accumulation of clear fluid with no or low PMN invasion ,ph >7.3, normal glucose & LDH levels : termed as ‘ simple ‘parapneumonic effusion .
Stage 2 or Fibrinopurulent or Transitional phase ( 3 to 21 days ): There is deposition of fibrin in the pleural space leading to septations & formation of loculations.There ithe sincrease in white cell count , ph < 7.3, glucose < 40mgs.,LDH >3 times the normal. Thisis termed as ‘complicated ‘ parapnumonic effusion. Eventually when it becomes overt or frank pus which is termed as an ‘ empyema’.The presence of septations (fibrinous strands in pleural fluid )doesn’t necessarily mean fluid doesn’t flow freely, although separate loculations will not communicate with each other.
Stage 3 or Organisational or Chronic phase (> 3 wks . duration ): Fibroblasts infiltrate the pleural space & thin intrapleural membranes are reorganised to become thick & non elastic – the ‘peel’ or ‘rind’. These solid fibrous or leather-like peels may prevent lung reexpansion ( “trapped lung” ), impair lung function & create a persistent pleural space with potential for infection.At this stage spontaneous healing may occur or a chronic empyema may develop.
Further complications which may occur are : bronchopleural fistula , lung abscess, pneumatocele formation, empyema necessitans : perforation through the chest wall, fibrothorax etc…Video-assisted thoracoscopic surgery (VATS ) is a key hole or minimal access surgical approach. It achieves debridement of fibrinous pyogenic material, a breakdown of loculations, and drainage of pus from the pleural cavity under direct vision. It leaves threesmall scars.
Mini-thoracotomy achieves debridement and evacuation in a similar manner to VATS but it is an open procedure leaving a small linear scar along the rib line.Decortication involves an open posterolateral thoracotomy and excision of the thick fibrous pleural rind with evacuation of pyogenic material. It is a longer and more complicated procedure leaving a larger linear scar along the rib line.
Key Guidelines for Management:
SITUATION 1 :
At Secondary hospital / Non-metro situation: Optimal standards of Treatment in situations where technology& resources are limited.
Clinical Diagnosis*
Acute , recurrent or chronic presentations are common. If a child with pneumonia remains pyrexial or unwell 48 hrs. after the start of the treatment possibility of parapneumonic effusion or empyema should be suspected. Constitutional signs / symptoms viz.. lassitude, poor appetite, pallor, intermittent fever,easy fatigability, sick look with dull percussion note & decreased breath sounds on auscultation in the setting of partially treated pneumonia, PUO, Disseminated infectionse g.. Pyoderma / otitis media/ arthritis/Osteomylitis / Serosal infections etc.. Febrile response may be blunted in immunocompromised patients.*Physical findings & presentation may vary depending on type organism & duration of illness.*Inflammation of pleural space may present with abdominal pain &vomiting
INVESTIGATIONS :
1) Chest X-ray : Posteroanterior ( PA ) view
2) Ultrasound chest :Sensitive for confirmation of pleural fluid , for guided diagnostic
tapping & insertion of chest drainage tube.
3) Pleural fluid exam:
Colour, Odour, Gram staining, AFB, Bacterial culture, cytology.
Biochemistry: Ph, Sugar, LDH, Proteins.
4 ) Blood & sputum culture : if feasible
TREATMENT :
Conservative Management : Antibiotics ± Intercostal Dranaige Tube (ICD) If effusion is simple & small in quantity : can be managed with antibiotics alone .But
very close observation is necessary for development of enlarging size &/or compromise of respiratory function when prompt ICD placement is necessary.
Repeated thoracentesis has no role. If effusion is complicated or frank pus : Antibiotics + ICD
Surgical management :
Only if adequately trained personnel & blood banking facilities are available then limited thoracotomy in a situation where there is no satisfactory response (persistent fever, incomplete lung expansion ,loculations on ultrasound etc..)ie.. in stage 2 or fibrinopurulent phase.
Standard operating procedure ( SOP )
All the patients of parapneumonic effusion or empyema should be admitted in hospital i e.. no out patient or day care management to be done. Pediatric surgeon or General surgeon familiar with basic thoracic surgery along with paediatrician or respiratory physician should manage these cases. They should be monitored closely & carefully by frequent clinical assessment & room air saturation by pulse oximeter whenever child is in resp. distress. Diagnostic imaging, microbiology, pleural fluid analysis should be carried out promptly. Conservative management to be started swiftly & supported by antipyretics, analgesia, oxygen , if necessary.
Empirical antitubercular therapy should be avoided as far as possible.
Antibiotics :
Intravenous antibiotics for 10 to 14 days for community acquired pneumonia covering Gram positive cocci & anaerobes to be started empirically pending preferably c & s report. Broad spectrum coverage should be started for hospital acquired pneumonia as well as empyema following surgery, trauma & aspiration. Oral antibiotics should be continued at discharge for 1-4 wks. or longer depending on disease state.
Chest drainage tube(ICD) insertion:
Chest drains should be inserted by adequately trained personnel to reduce the risk of complications. Preferably procedure should be done in operation room or isolated / treatment room on ward. However , if need arises it can be done as a bed side procedure as well. A suitable assistant and trained nurse must be available.
Routine measurement of the platelet count and clotting studies are only recommended in patients with known risk factors. Where possible, any coagulopathy or platelet defect should be corrected before chest drain insertion. Ultrasound should be used to guide thoracocentesis or drain placement. If general anaesthesia is not being used, intravenous sedation should only be given by those trained in the use of conscious sedation, airway management and resuscitation of
children, using full monitoring equipment. . Local anaesthesia, 2% xylocaine Or .25% bupivacaine, can also be used . Large bore surgical drains should be inserted at the optimum site suggested by ultrasound, but preferentially placed in the mid axillary line through the ‘‘safety
triangle’’.
Substantial force should never be used to insert a drain. Trocar usage preferably should be avoided & should it be needed ,due to circumstances, great care is mandatory to have a guard or control on it while inserting. Chest tube should be secured well with non absorbable suture & appropriate dressing. A chest radiograph should be performed after insertion of a chest drain.All chest tubes should be connected to a unidirectional flow drainage system (such as an underwater seal
bottle) which must be kept below the level of the patient’s chest at all times. A bubbling chest drain should never be clamped. A clamped drain should be immediately unclamped and medical advice sought if a patient complains of breathlessness or chest pain.
The drain should be clamped for 1 hour once 10 ml/kg are initially removed.Patients with chest drains should be managed on wards by staff trained in chest drain
management.
When there is a sudden cessation of fluid draining, the drain must be checked for obstruction (blockage or kinking) by flushing. The drain should be removed once there is clinical resolution. A drain that cannot be unblocked should be removed and replaced by new catheter if significant pleural fluid remains.
Surgical management :
Proper planning & ensuring availability of all the trained & experienced personnel ie..surgeon, anaesthesiologist ,OT technician & nursing staff and also smooth supply of oxygen,blood ,medicines etc..is very important . Limited thoracotomy with or without rib resection by 5-7cms total incision on either side
of chest tube ,if already in situ. To ensure complete lung expansion at the end of the procedure with minimal air leak. If necrotic lung tissue is present then excision of the segment is to be done. Send debrided tissue or ‘gubbin ‘ for histopathological examination. ICD removal after complete lung expansion ,minimal or no drainage ,afebrile state & no air leak X ray chest to be done before ICD tube removal Good analgesia ( oral &/or suppositories ) & early ambulation to hasten the recovery should be practiced regularly. Antibiotics for 1-2wks. after the discharge are usually sufficient except in situation of complications.
Follow- up :
Till complete resolution of disease process & near complete lung expansion on x- ray
chest.
Evaluation of underlying condition, if any.
Referral criteria
If no satisfactory response to conservative management by 5-7 days. Initial presentation as stage 2 or 3 of an empyema Suspecting underlying immunodeficiency condition or empyema associated with non-pneumonic pathologies which also require specialist’s attention. Development of complications eg Persistent air leak.
Non availability of trained personnel at given time.
Situation 2
At Super Speciality Facility in Metro location where higher end technology is available
Clinical diagnosis*
If a child with pneumonia remains pyrexial or unwell 48 hrs. after the start of the treatment possibility of parapneumonic effusion or empyema should be suspected.
Constitutional s/s viz.. lassitude, poor appetite, pallor, intermittent fever, easy fatigability, sick look with dull percussion note & decreased breath sounds on
auscultation in the setting of partially treated pneumonia, PUO, Disseminated infections e g.. Pyoderma/otitis media /arthritis/Osteomylitis / Serosal infections etc.. Patients inadequately treated or responded to previous therapy. Complications of an empyema eg.. BPF, lung abscess, empyema necessitans etc. Patients with underlying conditions such as liver abscess, pancreatitis ,trauma , surgical or endoscopic procedure done etc with respiratory signs & symptoms.
Response may be blunted ‘absent fever’ in immunocompromised patients. *Acute , recurrent or chronic presentations are common. *Physical findings & presentation may vary depending on type of organism & duration of illness. *Inflammation of pleural space may present with abdominal pain &vomiting
Investigations
Diagnostic imaging
Posteroanterior or anteroposterior radiographs should be taken; there is no role for a routine lateral radiograph. Ultrasound may be used to confirm the presence of a pleural fluid collection, septations, to guide thoracocentesis or drain placement. Chest CT scans should not be performed routinely. It should be done once surgery is contemplated to know pleural peel thickness, loculations & their details such as number, position, size etc.; parenchymal pathology,guide for port placement if VATS is being planned .
Diagnostic microbiology
Blood cultures should be performed in all patients with parapneumonic effusion. When available, sputum should be sent for bacterial culture.
Diagnostic analysis of pleural fluid
Pleural fluid must be sent for microbiological analysis including Gram stain and bacterial culture. Aspirated pleural fluid should be sent for differential cell count.
Tuberculosis and malignancy must be excluded in the presence of pleural lymphocytosis. If there is any indication the effusion is not secondary to infection, consider an initial small volume diagnostic tap for cytological analysis, avoiding general anaesthesia/sedation whenever possible. Biochemical analysis of pleural fluid : Ph, LDH, sugar, & proteins
Diagnostic bronchoscopy
There is no indication for bronchoscopy and it is not routinely recommended. Considered only when bronchoalveolar lavage is necessary or suspected foreign body or assessing bronchial mucosal status for safe closure of br. stump when major pulmonary resection is also planned alongwith decortication .
Treatment
Conservative management (antibiotics ± simple drainage)
Effusions which are enlarging and/or compromising respiratory function should not be managed by antibiotics alone. Give consideration to early active treatment as conservative treatment results in prolonged duration of illness and hospital stay. If a child has significant pleural infection, a drain should be inserted at the outset and repeated taps are not recommended.
Antibiotics
All cases should be treated with intravenous antibiotics and must include cover for Gram positive cocci eg..Staph Aureous, Streptococci & Anarobes. Broader spectrum cover is required for hospital acquired infections, as well as those secondary to surgery, trauma, and aspiration. Where possible, antibiotic choice should be guided by microbiology results. Oral antibiotics should be given at discharge for 1–4 weeks, but longer if there is residual
disease.
Chest drains
Chest drains should be inserted by adequately trained personnel to reduce the risk of complications.
A suitable assistant and trained nurse must be available. Routine measurement of the platelet count and clotting studies are only recommended in patients with known risk factors. Where possible, any coagulopathy or platelet defect should be corrected before chest drain insertion. Ultrasound should be used to guide thoracocentesis or drain placement, when available. If general anaesthesia is not being used, intravenous sedation should only be given by those trained in the use of conscious sedation, airway management and resuscitation of children, using full monitoring equipment.
Large bore surgical drains should be inserted at the optimum site suggested by ultrasound. The usual site for ICD insertion should be in the mid axillary line in the 5th intercostal space which is in the ‘safe triangle.’ Substantial force should never be used to insert a drain. Trocar usage preferably should be avoided & should it be needed ,due to circumstances, great care is mandatory to have a guard or control on it while inserting. Chest radiograph should be performed after insertion of a chest drain. All chest tubes should be connected to a unidirectional flow drainage system (such as an underwater seal bottle) which must be kept below the level of the patient’s chest at all times.
Appropriately trained nursing staff must supervise the use of chest drain suction. A bubbling chest drain should never be clamped. A clamped drain should be immediately unclamped and medical advice sought if a patient complains of breathlessness or chest pain. Patients with chest drains should be managed on specialist wards by staff trained in chest drain management.
When there is a sudden cessation of fluid draining, the drain must be checked for obstruction (blockage or kinking) by milking / flushing. If it can not be unblocked in presence of significant pleural infection then it should be reinserted. The drain should be removed once there is clinical resolution & / or lung expansion on xray.
Intrapleural fibrinolytics
Intrapleural fibrinolytics are said to shorten hospital stay and may be used for any stage 2 empyema . There is no evidence that any of the three fibrinolytics ( Streptokinase, Urokinase, Alteplase ) are more effective than the others, but only urokinase has been studied in a randomised controlled trial . Urokinase should be given twice daily for 3 days (6 doses in total) using 40 000 units in 40 ml 0.9% saline for children weighing 10 kg or above, and 10 000 units in 10 ml 0.9%
saline for children weighing under 10 kg.
Surgery
Patients should be considered for surgical treatment if they have persisting sepsis in association with a persistent pleural collection, despite chest tube drainage and
antibiotics. Failure of chest tube drainage, antibiotics, and fibrinolytics would necessiiate surgical intervention.However, a pediatric surgeon should be involved early in the management of empyema thoracis.
If requisite skill & facilities are available then VATS debridement is preferable over open surgical procedure in stage 2 & select stage 3 empyema cases. Organised empyema in a symptomatic child may require formal thoracotomy and decortication.
Other management
Antipyretics should be given. Analgesia is important to keep the child comfortable, particularly in the presence of a chest drain. Early mobilisation , chest physiotherapy and exercise is recommended. Secondary scoliosis noted on the chest radiograph is common but transient; no specific treatment is required but resolution must be confirmed.
Standard operating procedure ( SOP )
All the patients of parapneumonic effusion or empyema should be admitted in hospital i e.. no out patient or day care management to be done. Pediatric surgeon or a surgeon well trained in pediatric thoracic surgery along with paediatrician or respiratory physician should manage these cases. CECT( Contrast Enhanced Cat Scan ) should be done if surgery is contemplated. There are no evidence based criteria to guide the decision on when a child should proceed to surgery, and consequently there is little consensus on the role of medical versus surgical management (1)
Intrapleural fibrinolytics
Intrapleural fibrinolytics shorten hospital stay and are recommended for any complicated parapneumonic effusion (thick fluid with loculations) or empyema (overt pus). There is no evidence that any of the three fibrinolytics(streptokinase,urokinase &tPA ) are more effective than the others, but only urokinase has been studied in a randomised controlled trial in children so is recommended(10 to 16)
Surgery:
The decision to involve a pediatric surgeon early in the decision making process should be encouraged and referral should not automatically mean surgery is inevitable .(1) Available procedures are: VATS, Mini thoracotomy & Decortication. A chest drain(s) is left after each procedure for further drainage of fluid/pus. A persistent radiological abnormality in a symptom-free well child is not an indication for surgery.
Role of surgical management in complex empyema
(A) Organised empyema with a thick fibrous peel
Organised empyema in a symptomatic child may require formal thoracotomy and decortication. The surgical management of an organised empyema, in which a thick fibrous peel is restricting lung expansion and causing chronic sepsis with fever, requires a formal thoracotomy with excision of the pleural rinds (decortication) to achieve proper lung reexpansion. However, if the child is asymptomatic, surgery is not necessarily indicated.(18)
(C) Bronchopleural fistula and pyopneumothorax
Different approaches have been advocated for a bronchopleural fistula related to an empyema. Most fistulae are peripheral and the majority resolve with continued chest drainage and antibiotics provided the lung shows satisfactory lung expansion. However, at times they are slow and difficult to resolve, and it has been said that
conservative management and open thoracostomies result in protracted recovery and morbidity. A more radical approach is partial decortication and muscle flap surgery to bring a blood supply to the necrotic area and help with healing the fistula. This can either be done as a staged procedure or a more aggressive one stage approach (19, 20)
Follow up
Children should be followed up after discharge until they have recovered completely and their chest radiograph has returned to near normal. Underlying diagnosis—for example, immunodeficiency –may need to be considered in selected situations. open chest tube care in select patients till tube is in situ
For monitoring of ATT
Referral to tertiary speciality centre
Non availability of skilled & experienced personnel or infrastructure necessary for management of complex situations eg. BPF, major lung resections or Thoracoscopic procedure or need of PICU facilities etc.. When respiratory paediatrician is needed to be involved early in the care of patients requiring chest tube drainage for a pleural infection & in critically ill child.
Who does what ? & Time lines :
Doctor : Pediatric Surgeon :
Does all the interventional procedures & involved in decision making regarding overall management with paediatrician. Pediatrician (Respiratory ) : Along with surgeon involved in conservative management & post operative care & preop. preparation General Surgeon : Does interventions In situation 1 only & in situation 2
maybe involved in assisting pediatric surgeon. Anaesthesiologist : Anaesthesia & pain management Junior doctor : Assisting in surgery, ICD care ,dressings & day to day ward management
b ) OT Technician: Helping anaesthesiologist & surgeon in OT & if required on ward
bedside interventions.
C ) Nursing Staff: Care & organisation of instrument trolly, medications & ICD care, suction etc. & day to day nursing care.
Time line :
Radiological clearance takes few wks. to many months. If an empyema fails to respond in 3-5 days of conservative treatment then surgical intervention should be considered to reduce morbidity. Dwelling time for fibrinolytics is 1-4 hours. There is no specific / precise time period for spontaneous closure or need for surgical intervention in BPF patients. Antibiotics are needed for 4-8 wks. ( Intravenous 2-3 wks. & oral 1-4wks.) ATT is required for 6-9 mths duration.
Guideline Developed by Dr.Rajendra Saoji, Consultant Pediatric Surgeon, Nagpur

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd