- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
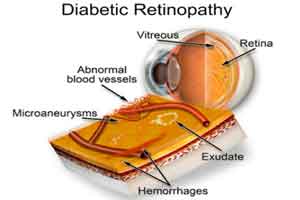
Diabetic Retinopathy- Standard Treatment Guidelines
Diabetes Mellitus (DM) has established itself as a pandemic disease, projected to affect 438 million people by the year 2030.The exponential growth in the incidence and identification of systemic diabetes has projected diabetic retinopathy as one of the leading causes of visual loss globally.
Diabetic retinopathy (DR) is one of the most frequent causes of blindness worldwide. In India DR which was the 17th cause of blindness but has now ascended to the 6 th position. Diabetic retinopathy screening is directed towards improving health care services for persons with diabetes and diabetic retinopathy. It is symptomless in its early stage; screening is the only way to identify these patients to prevent them from going blind. The number of DR patients’ increase with increase in the diabetic population, especially in developing countries where there is resource scarcity. Timely treatment can prevent vision loss which means that all of the diabetics have to be regularly examined for DR.
The Ministry of Health and Family Welfare has issued the standard treatment Guidelines for Diabetic Retinopathy. Following are the major recommendations:
Case definition:
Diabetic Retinopathy is primarily a microvascular disease. For all practical purpose fundus changes like micro aneurysms, hard exudates and hemorrhages in diabetic patients are to be considered as diabetic retinopathy until proved otherwise. The most common cause of visual loss in diabetic patients is due to macular edema (DME) and advanced diabetic retinopathy (Vitreous hemorrhage and Retinal detachment).
Incidence of the condition in our country
Diabetic retinopathy is the leading cause of blindness among adults in the developing countries and is emerging as an important cause of blindness in the developing countries next to cataract. The longer the duration of diabetes higher is the incidence of developing diabetic retinopathy. In India, there is a paucity of data on the prevalence of DR in type 1 diabetes mellitus, as a registry for prevalence of type 1 diabetes is only recently being set up in the country. The prevalence of diabetic retinopathy in India, according to various population based studies is in between 17.6% to 34.1%. An earlier study done in a clinic-based population reported an overall prevalence of 14 per cent of DR in a diabetic population examination. Of these, non proliferative diabetic retinopathy (NPDR) accounted for 6 per cent, macular oedema accounted for 4 per cent and proliferative diabetic retinopathy accounted for rest of the 4 per cent.
Differential Diagnosis
Diabetic retinopathy may present like or coexist with other conditions and hence one needs to be careful with making a diagnosis. The following disorders may also present similary and hence they have to be ruled out.
1. Hypertensive retinopathy
2. Vascular occlusive disorders
3. Inflammatory chorio retinopathy
4. Radiation retinopathy
5. Age related macular degeneration
Prevention And Counselling
- All the diabetic patients are the potential candidates for vision impairment. Strict control of blood glucose level and other risk factors like hypertension, hypercholesterolemia, anaemia will retard the development and progression of DR..
- Screening of all “known diabetic patients” for DR at their primary point of contact, by physicians/diabetologists as most of the diabetic patients come to the ophthalmologists only after experiencing considerable vision loss will detect early cases.
- All pregnant women with diabetes should have dilated eye examinations during each trimester of their pregnancy to check for retinopathy
- Educating the community for regular eye check up and having good healthy diet, exercises and avoiding smoking goes a long way in preventing progression of diabetic retinopathy.
Optimal Diagnostic Criteria, Investigations, Treatment and Referral Criteria
At Super speciality Hospital
Clinical Diagnosis:
History taking: Diabetic retinopathy often has no early warning signs. Patients usually presents with painless loss of vision. A thorough and complete history taking regarding past duration of diabetes, treatment history, family history and history of associated risk factors is essential. Waiting for the diabetic to present with visual problems is not a good strategy. Many patients retain normal eyesight or experience a minimal (and sometimes unnoticeable) reduction of vision even in the presence of sight-threatening disease (diabetic maculopathy, proliferative disease). It is for this reason that screening for DR is mandatory. Sometimes, the patients may become aware of a problem (whether or not they are known diabetics) as in :
A painless gradual reduction of central vision may be associated with any of the types of DR. The most common cause is diabetic macular oedema. Painless and gradual visual loss is also associated with coexistent cataract formation (diabetic or otherwise).
- Haemorrhages result in the sudden onset of dark, painless floaters which may resolve over several days.
- Severe vitreous haemorrhage may obscure the vitreous altogether resulting in a painless visual loss.
- An acute attack of glaucoma precipitated by rubeosis iridis is the one situation where the patient will present with acute pain; urgent referral is essential.
Examination: a complete and comprehensive examination using a direct ophthalmoscope, indirect ophthalmoscope and slit lamp with 90 dioptre lens is essential for diagnosing and staging diabetic retinopathy. Careful staging and appropriate management goes a long way in preventing visual loss due to diabetic retinopathy.
International clinical diabetic retinopathy disease severity scale 5 levels for Diabetic Retinopathy – none, mild, moderate, severe and proliferative
| Proposed Disease Severity Level | Findings Observable upon Dilated Ophthalmoscopy |
| No Apparent retinopathy | No abnormalities |
| Mild non-proliferative diabetic retinopathy | Microaneurysms only |
| Moderate non-proliferative diabetic retinopathy | Microaneurysms . dot shaped haemorrhages and hard exudates but less than severe NPDR |
| Severe non-proliferative diabetic Retinopathy | Any of the following : More than 20 intra-retinal hemorrhages in each of 4 quadrants Definite venous beading in 2+quadrants Prominent IRMA in 1+ quadrant And no signs of proliferative retinopathy |
| Proliferative diabetic retinopathy | One or more of the following: Neovascularization of the Disc or else where Vitreous / preretinal hemorrhage |
International clinical diabetic retinopathy disease severity of diabetic macular edema
2 Major levels, with subcategories for diabetic macular edema
| Proposed Classification | Findings Observable upon Dilated Ophthalmoscopy |
| Diabetic Macular Edema Absent | No retinal thickening or hard exudates in posterior pole |
| Diabetic Macular Edema Present | Some retinal thickening or hard exudates in posterior pole |
Diabetic macular edema is classified into three types based on FFA findings:
- Focal exudative maculopathy
- Diffuse exudative maculopathy
- Ischaemic maculopathy.
Term clinically significant macular edema(CSME) is considered ,if one of the following criteria are present on :
- Retinal edema or Thickening of the retina at or within 500µ of the centre of the fovea.
- Hard exudates at or within 500 µ of the centre of fovea associated with adjacent retinal thickening
- Retinal thickening of size 1DD, at least a part of which is within 1DD of the foveal centre.
Advanced diabetic eye disease.
- Vitreous and preretinal haemorrhages occur as new vessels grow forward from the retina and enter the vitreous where they bleed easily.
- Haemorrhages appear as reddish/dark opacities; preretinal or subhyaloid haemorrhages.
- Retinal detachment.
- Rubeosis iridis .
Investigations:
Visual acuity test: This is done as a baseline investigation. Amsler’s grid evaluation is also useful to monitor macular disease
Fundus examination with direct and indirect ophthalmoscope. The direct ophthalmoscope examination is essential for both community setting and general physicians. Indirect ophthalmosopy is done in case of advanced diabetic retinopathy.
Slit lamp biomicroscopy with 78D or 90D is gold standard for diagnosis of diabetic maculopathy.
Fundus photography and Digital Retinal Screening Programs: Systematic programs for the early detection of eye disease including diabetic retinopathy are becoming more common, where all people with diabetes mellitus are offered retinal screening at least annually. This involves digital image capture and transmission of the images to a digital reading center for evaluation and treatment referral.
Fluorescein Angiography
This is a magnified photography of the retina involving the use of an injectable dye. It helps to classify the condition and to record changes in the retinal blood vessels. It is also useful to rule out the ischemia of the macular region. The first angiogram is usually done during the first evaluation. Subsequent angiograms may be done to assess the progression of diabetic retinopathy and to decide on the mode of treatment
Treatment:
Medical Care
Glucose control: One of the clinical trials, the Diabetes control and complications trial (DCCT) has found that intensive glucose control in patients with insulin dependent diabetes mellitus (IDDM) has decreased the incidence and progression of diabetic retinopathy. Glycosylated hemoglobin levels of 6- 7% are ideal to prevent or at the very least to minimize the long-term complications of DM, including DM retinopathy.
Surgical Care
Laser photocoagulation is the standard technique for treating diabetic retinopathy. In general, it is advised for patients with high-risk PDR, CSME, or neovascularization of the anterior chamber angle. Either argon or diode laser can be used for photocoagulation. Laser photocoagulation techniques can be classified as panretinal, focal, or grid. Panretinal photocoagulation, also referred to as scatter photocoagulation, is used for the treatment of proliferative diabetic retinopathy. It may be done in more than one session. Focal and grid photocoagulation are used for the treatment of diabetic macular edema.
Diabetic Maculopathy :
Argon laser photocoagulation:
Indications:
- All eyes with CSMO should be considered for laser photocoagulation irrespective of the level of visual acuity because treatment reduces the risk of visual loss by 50%.
- Pre-treatment FFA is useful to delineate the area of leakage and to detect ischaemic maculopathy which carries a poor prognosis.
Focal treatment – burns are applied to microaneurysms and microvascular lesions in the centre of rings of hard exudates located 500 -3000µm from the centre of macula .The spot size is 50 - 100 µm , exposure time 0.1 sec with sufficient power to obtain gentle whitening or darkening of the lesions.
Grid treatment – burns are applied to areas of diffuse retinal thickening more than 500 µm from the centre of the macula and 500 µm from the temporal margin of the optic disc.the spot size is 100 µm and exposure time is 0.1 sec giving a very light intensity burn.
Proliferative Diabetic Retinopathy:
Panretinal photocoagulation:
Laser treatment is aimed at inducing involution of new vessels and preventing visual loss.
Indications:
- PDR with HRCs
- Neovascularisation of irirs
- Severe NPDR associated with :
o Poor compliance for follow up
o Before cataract surgery/YAG capsulotomy
o Renal failure
o Pregnancy
o One-eyed patient
The recommended therapy is 1200-2000 burns 500µm in diameter delivered through the goldmann lens or the same number of 200 µm burns delivered through volk lens. The burns should be intense enough to whiten the overlying retina,which usually requires a power of 200 – 600mW and duration of 0.1 second.
Treatment of Diabetic Retinopathy
| Proliferative Retinopathy | Clinically Significant Macular Oedema Retinal microaneurysms | Clinically Significant Macular Oedema Retinal thickening & areas of non-perfusion | |
| Type of laser | Argon green | Green or yellow (577) argon laser | Green or yellow (577) argon laser |
| Spot size | 200-500µm | 50 - 100µm | 100µm |
| Power | 0.2 - 0.8 watts | 0.1 - 0.3 watts | 0.1 - 0.3 watts |
| Duration | 0.2 seconds | 0.1 seconds | 0.05 - 0.1 seconds |
| End point | Faint white burn at level of retinal pigment epithelium (RPE) | Faint whitening of RPE or darkening of microaneurysm | Very faint white burn at level of retinal pigment epithelium (RPE) |
| How to treat | Do not overlap burns Do not treat within temporal arcades Do not treat within one disc diameter of optic disc Do not treat within two disc diameters temporal to fovea | Apply burns directly to microaneurysms | Place burns at least one burn width apart, to make a grid which includes the area of retinal thickening Do not treat within 500m of fovea at first session |
| Number of burns | Approximately 2,000 | Variable | Variable |
| Number of sessions | Two sessions. Treat the lower half of the retina first (1,000 burns) | One | One |
| Other | Topical steroids and mydriatic after treatment |
| Signs of resolution | New vessels regressing Reduced blood flow in new vessels More fibrous tissue Less beading of retinal veins | Less retinal thickening/exudate | Less retinal thickening |
| Indications for retreatment | Fresh new vessels on the optic disc or elsewhere in the fundus Failure of new vessels to regress | Significant macular oedema after 3 months | Significant macular oedema after 3 months |
| Retreatment | Between previous burns, avoiding retinal vessels | Do not retreat areas lying in the macular-papular bundle | Treat to within 100m of the edge of the foveal avascular zone |
Standard Operating procedure
a.In Patient – No need
b. Day Care – Not applicable
c.Out Patient Procedure:
- Screening, diagnosis and disease management.
- Providing treatment for diabetic retinopathy with lasers and other medical treatment.
Referral criteria:
If the patients are requiring further investigations/treatment such as vitrectomy, Retinal detachment surgery is referred to the tertiary level eye care provider.
At Super Specialty Hospital
Clinical Diagnosis:
History taking: Diabetic retinopathy often has no early warning signs. Patients usually presents with painless loss of vision. A thorough and complete history taking regarding past duration of diabetes, treatment history, family history and history of associated risk factors is essential. Waiting for the diabetic to present with visual problems is not a good strategy. Many patients retain normal eyesight or experience a minimal (and sometimes unnoticeable) reduction of vision even in the presence of sight-threatening disease (diabetic maculopathy, proliferative disease). It is for this reason that screening for DR is mandatory. Sometimes, the patients may become aware of a problem (whether or not they are known diabetics) as in :
A painless gradual reduction of central vision may be associated with any of the types of DR. The most common cause is diabetic macular oedema. Painless and gradual visual loss is also associated with coexistent cataract formation (diabetic or otherwise).
- Haemorrhages result in the sudden onset of dark, painless floaters which may resolve over several days.
- Severe vitreous haemorrhage may obscure the vitreous altogether resulting in a painless visual loss.
- An acute attack of glaucoma precipitated by rubeosis iridis is the one situation where the patient will present with acute pain; urgent referral is essential.
Examination: a complete and comprehensive examination using a direct ophthalmoscope, indirect ophthalmoscope and slit lamp with 90 dioptre lens is essential for diagnosing and staging diabetic retinopathy. Careful staging and appropriate management goes a long way in preventing visual loss due to diabetic retinopathy.
International clinical diabetic retinopathy disease severity scale 5 levels for Diabetic Retinopathy – none, mild, moderate, severe and proliferative
| Proposed Disease Severity Level | Findings Observable upon Dilated Ophthalmoscopy |
| No Apparent retinopathy | No abnormalities |
| Mild non-proliferative diabetic retinopathy | Microaneurysms only |
| Moderate non-proliferative diabetic retinopathy | Microaneurysms . dot shaped haemorrhages and hard exudates but less than severe NPDR |
| Severe non-proliferative diabetic Retinopathy | Any of the following : More than 20 intra-retinal hemorrhages in each of 4 quadrants Definite venous beading in 2+quadrants Prominent IRMA in 1+ quadrant And no signs of proliferative retinopathy |
| Proliferative diabetic retinopathy | One or more of the following: Neovascularization of the Disc or else where Vitreous / preretinal hemorrhage |
International clinical diabetic retinopathy disease severity of diabetic macular edema
2 Major levels, with subcategories for diabetic macular edema
| Proposed Classification | Findings Observable upon Dilated Ophthalmoscopy |
| Diabetic Macular Edema Absent | No retinal thickening or hard exudates in posterior pole |
| Diabetic Macular Edema Present | Some retinal thickening or hard exudates in posterior pole |
Diabetic macular edema is classified into three types based on FFA findings:
- Focal exudative maculopathy
- Diffuse exudative maculopathy
- Ischaemic maculopathy.
Term clinically significant macular edema(CSME) is considered ,if one of the following criteria are present on :
- Retinal edema or Thickening of the retina at or within 500µ of the centre of the fovea.
- Hard exudates at or within 500 µ of the centre of fovea associated with adjacent retinal thickening
- Retinal thickening of size 1DD, at least a part of which is within 1DD of the foveal centre.
Advanced diabetic eye disease.
- Vitreous and preretinal haemorrhages occur as new vessels grow forward from the retina and enter the vitreous where they bleed easily.
- Haemorrhages appear as reddish/dark opacities; preretinal or subhyaloid haemorrhages.
- Retinal detachment.
- Rubeosis iridis .
b) Investigations: Same as situation 1. Some additional investigations help in explaining prognosis and planning the surgery (example Optical Coherence Tomography(OCT)
c) Treatment:
General Management Recommendations:
| Level of Retinopathy | Evaluation | Treatment Strategies |
| Fluorescein Angiography | PRP | Focal | Follow-up (months) | |
| Mild NPDR | ||||
| No macular edema | No | No | No | 12 |
| Macular edema | No | No | No | 4-6 |
| CSME | Yes | No | Yes | 2-4 |
| Moderate NPDR | ||||
| No macular edema | No | No | No | 6-8 |
| Macular edema (not CSME) | No | No | No | 4-6 |
| CSME | Yes | No | Yes | 2-4 |
| Severe NPDR |
| No macular edema | No | Rarely | No | 3-4 |
| Macular edema (not CSME) | No | Occasionally after focal | Occasionally | 2-3 |
| CSME | Yes | Occasionally after focal | Yes | 2-3 |
Standard Operating procedure:
The operating procedures like vitrectomy, retinal detachment surgeries and other intravitreal medications are done for those cases of advanced retinal detachment which have been referred from secondary eye care.
Surgical treatment in advanced diabetic eye disease:
Laser photocoagulation allows effective treatment of moderate to severe PDR .Some eyes can progress to tractional retinal detachment and vision loss. Standard laser cannot be performed in eyes with vitreous hemorrhage precluding visualization of the retina.
Pars plana vitrectomy is the main method of treating severe complications of PDR. The diabetic retinopathy vitrectomy study ( DRVS) showed that early vitrectomy was beneficial for patients with visual acuity of 6/120 or better and having one of the following: (1) severe neovascularization and fibrous proliferation; (2) fibrous proliferation and moderate vitreous hemorrhage; or (3) moderate neovascularization, severe fibrous proliferation, and moderate vitreous hemorrhage.
Role of vitrectomy:
The most common indications for diabetic vitrectomy are :
1. Severe nonclearing vitreous haemorrhage,
2. Traction retinal detachment recently involving the macula,
3. Combined traction and rhegmatogenous detachment,
4. Progressive fibrovascular proliferation,
5. Rubeosis iridis and vitreous haemorrhage, with opacity preventing adequate laser.
The DRVS study concluded that:
1. Early vitrectomy provides a greater chance for prompt recovery of visual acuity in eyes with recent severe vitreous haemorrhage.
2. For patients with IDDM, in whom severe vitreous haemorrhage occurred after a shorter duration of diabetes, early vitrectomy provides a greater chance of recovering good visual acuity
3. DRVS findings support early vitrectomy in eyes known or suspected to have very severe PDR as a means of increasing the chance to restoring or maintain good vision.
4. Vitrectomy for traction retinal detachment or macular traction: Progressive tractional RD threatening or involving the macula must be treated without delay.
Other medications that are being used in clinical practice and in clinical trials include intravitreal bevacizumab (Avastin) and ranibizumab (Lucentis), These medications are VEGF antibodies and antibody fragments, respectively. They can help to reduce diabetic macular edema and also neovascularization of the disc or retina
Out Patient
- Diagnosis and disease management
- Investigations for diabetic retinopathy
- Fluorescein angiography
- Photography-scan ultrasonography
- Lasers for diabetic retinopathy
In Patient:
- Advanced diabetic retinopathy
- Patient who need surgical treatment
- Patient with neovascular glaucoma, complicated cataract and other ocular complication secondary to diabetes has to be admitted for further management.
Who does what? And timelines
Doctor
- history taking, clinical examination ,treatment plan
- Follow up schedule
- Need additional skills in indirect ophthalmoscopy,
- Interpretation of Fluorescein angiography.
- Handling retinal laser photocoagulation
- Surgical management of DR.
Nurse
- Assist in conducting diagnosis and examination of patient and preparing them for treatment.
- Attend and assist in diabetic retinopathy screening camps.
Technician
- Undergo additional training in fundus photography and fluorescein angiography
- FFA - Indications, technique complications-Basic ultrasonography
Resources Required
| Situation | Human Resources | Investigations | Drugs & Consumables | Equipment |
| 1 Seconday level | 1)Ophthalmologist – 1 2)Nurse - 1 3)Technician - 1 4)Counsellor - 1 5)Field coordinator - 1 | 1)FFA 2)USG 3) Blood sugar | 1) Fluoresceing dye 2) Antiangiogenic injections 3) Mydriatics 4) Neeles | 1) FFA including retinal camera & imagenet - 1 2) Ultrasonography 3) Indirect ophthalmoscope with 20D lens-1 4) Frequency double YAG laser with endolaser probe/slit lamp delivery with all accessories- 1 |
| 2. Tertiary level | 1)Ophthalmologist – 2 2)Retina specialist - 2 3)Nurse - 3 4)Technician – 1 5)Counsellor - 2 6)Field coordinator - 1 | 1) FFA 2) USG 3) OCT 4) Blood sugar | 1) Fluoresceing dye 2) Antiangiogenic injection 3) Irigating solution 4) Intraocular gas and silicon oil 5) Mydriatics 6) Needle s and syringes 7) Suture materials | 1) FFA including retinal camera & imagenet - 1 2) Ultrasonography-1 3) Indirect ophthalmoscope with 20D lens -1 4) Frequency double YAG laser with endolaser probe/slit lamp delivery with all accessories- 1 5) OCT – 6)ERG – 1 Surgical equipment: 1. Vitrectomy console 2. VR surgical instrument 3. Surgical operating microscope with CCTV attachment and observerscope–1 |
Guidelines Developed Ministry of Health and Family Welfare-
Group Head Coordinator of Development Team Dr. Venkatesh Prajna Chief- Dept of Medical Education, Aravind Eye Hospitals, Madurai

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd