- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Delhi doctors report a rare case of 'Pancake' Kidney
Dr Manu Vats, General Surgery, Maulana Azad Medical College, New Delhi, India, and colleagues have reported a rare case of 'Pancake' Kidney. The case is published in the journal BMJ Case Reports.
A "pancake kidney" occurs due to the fusion between top and bottom of the kidneys, resulting in one big, fused kidney instead of two separate, kidney-bean-shaped organs.

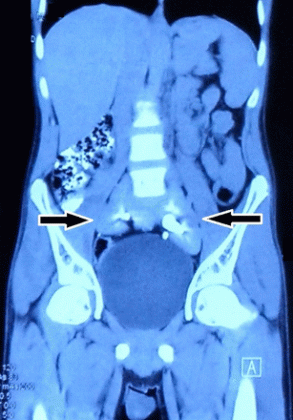
CECT abdomen coronal section showing fused ‘pancake’ kidney in the pelvis (solid arrows). CECT, contrast-enhanced CT.
Credits: BMJ Case Reports 2018
According to history, an 18-year-old man presented to the emergency department with signs and symptoms of acute intestinal obstruction. He had a previous history of exploratory laparotomy for intestinal obstruction 8 years ago. His abdominal examination revealed a healthy transverse scar in the right lumbar region extending to the umbilical region, abdominal distension and no tenderness or guarding. The patient was managed conservatively by nasogastric tube decompression and intravenous fluids support. A contrast-enhanced computed tomography (CECT) of the abdomen was done. The patient responded well to the conservative management, and the intestinal obstruction was relieved.
His computed tomography (CT) scan revealed something completely unrelated to the man's gut problems: He had a rarely encountered condition called "pancake kidney."
The most extreme form of renal fusion is the pancake kidney (PK), which contributes to less than 10% of all renal fusion anomalies. There is a characteristic extensive fusion of the superior and inferior poles of both kidneys across the entire medial aspect with the isthmus being absent. The pelvis is anteriorly placed, and the ureters remain uncrossed. Each collecting system drains its respective half of the kidney and does not communicate with the opposite side. Such kidney may also be referred to as a pancake, disc, doughnut, cake or a shield kidney.
Patients with PK are usually asymptomatic but may present with features of urinary tract infection, fever, and vague lower abdominal pain as they are more predisposed to urinary stasis and obstruction.
Pancake kidney forms during embryological development, Steven Chang, an assistant professor of surgery in the division of urology at Brigham and Women's Hospital in Boston, told Live Science. Normally, when the kidneys form, these two developing structures ascend to a location in the body that's closer to the mid-spine, with one kidney migrating to either side of the spine, he said.
The pancake kidney can't get to a location in the body as high up as the mid-spine, Chang said. Instead, the fused kidney settles into a lower position, located closer to the pelvis, Chang said. In the Indian man's case, his pancake kidney sat right above his bladder.
A pancake kidney isn't the only variety of kidney abnormality, however. A more common, but still rare, the condition occurs when the two developing kidneys fuse together at the bottom — but not at the tops — creating a U-shape. This is known as a "horseshoe kidney," Chang said.
People can live their whole lives with a pancake kidney and never know they have it, Chang said.
Indeed, in the man's case, doctors weren't looking for a pancake kidney, and it wasn't causing any problems. (The reason that the man went to the hospital, an intestinal obstruction, was successfully treated, and wasn't related to his oddly shaped kidney.)
But there's no need to treat a pancake kidney by surgically separating the mass into two kidneys, especially if a person has normal kidney function as this young man did, Chang said. This type of surgery would be difficult, and the risks would outweigh the benefits, he noted.
Carry Home points
Pancake kidney is an extremely rare congenital renal fusion disorder.
The diagnosis of pancake kidney is usually an incidental one, and unless the patient is symptomatic, a conservative approach is pursued.
Individuals with pancake kidney have a higher incidence of neoplasms; therefore, periodic regular follow-up is advisable.
For further reference follow the link 10.1136/bcr-2018-226751

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd