- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Regional Anaesthesia- Current Practices, Newer Techniques
There has been a lot of advancement in the practice of regional anaesthesia in last few decades especially after the introduction of ultrasound-guided regional anaesthesia (UGRA). Dr. Christopher Wahal of Department of Anesthesiology,at Duke University School of Medicine, North Carolina, USA and associates after examining all relevant literature have written a review article on Advances in regional anaesthesia in Indian Journal of Anaesthesia.The authors have lucidly explained a current practice, newer techniques, and outcomes including Advances in ultrasound-guided regional anaesthesia and introduction of newer long-acting local anaesthetics. They have reviewed some of the newer regional anaesthetic techniques, long-acting local anaesthetics and adjuvants, and discussed available evidence for key outcomes such as cancer recurrence and safety with ultrasound guidance.The article has been Published in Indian journal of anaesthesia.
Regional Anaesthesia for Chest Wall Surgery
- Paravertebral blocks (PVBs) can result in better post-operative analgesia with decreased opioid consumption, decreased length of stay and related side effects compared patient-controlled analgesia (PCA). However, not every patient may be a candidate for a PVB, particularly in the setting of anticoagulation or coagulopathy, and associated risks of pneumothorax, spinal cord trauma, neuraxial block and hypotension.
- PECS blocks are novel plane blocks that involve infiltration of local anaesthetic between the muscles of the thoracic wall. The PECS I block is a superficial block performed between the pectoralis major and pectoralis minor muscles and targets the medial and lateral PECS, ideally suited for superficial procedures such as the placement of breast expanders.
- The modified PECS block or PECS II deposits local anaesthetic between the pectoralis minor and serratus anterior muscles at the level of the third rib and targets the lateral branches of the third to sixth intercostal nerves in addition to the long thoracic and thoracodorsal nerves.This provides more complete analgesia of the breast along the dermatomes of T2 to T4 and is ideal for wider breast excisions, mastectomies and procedures involving axillary dissections.
Other methods like the serratus plane block have been described but not found superior to PVB in both quality of analgesia and opioid consumption for radical mastectomy.
Advances in Regional Anaesthesia for Shoulder Surgery
- Interscalene brachial plexus has been the gold standard but a significant number of patients develop hemidiaphragmatic paralysis (HDP) due to unilateral phrenic nerve blockade sometimes requiring respiratory monitoring. This is particularly important in patients with severe pulmonary disease and obese individuals. Lowering the local anaesthetic volume and deposition lateral to the brachial plexus is an attractive alternative, but this does not completely eliminate the risk.
- Other options are a combination of supraclavicular brachial plexus approach with suprascapular nerve block and infraclavicular block in combination with suprascapular nerve block, four individual nerve blocks to avoid HDP.But these procedures need further research and validation before putting them to practice.
- Recently, costoclavicular approach to brachial plexus has been described the benefits of which are similar to supraclavicular block, the risk of pneumothorax and sparing of lower trunk nerves is lower. This block is particularly useful for vascular, wrist and hand surgeries.
Regional Anaesthesia for Abdominal Wall Surgery
For those patients who may not be ideal candidates for neuraxial anaesthesia, truncal blocks are an attractive multimodal approach to pain control for a variety of abdominal surgeries.
Transversus abdominis plane block-
- Transversus abdominis plane (TAP) infiltration is an increasingly popular option for both ambulatory and inpatient abdominal procedures and provides analgesia to the parietal peritoneum and anterior abdominal wall. TAP blocks have become safe after the introduction of an ultrasound-guided approach which has allowed for real-time visualisation of the needle as well as local anaesthetic spread.
- This block is appropriate for incisions that are largely below the level of the umbilicus. The oblique subcostal approach can be used for the upper abdominal surgeries. With this approach, the needle is inserted near the xiphoid and advanced inferolaterally to deliver local anaesthetic in the TAP along the costal margin. This method can be combined with the posterior approach to provide even wider analgesic coverage.
- There is no consensus on ideal volume or concentration of local anaesthetic, with clinical studies using volumes from 10 to 30 mL per side. This is a field block in an anatomic plane where spread of local anaesthetic is the primary driver of analgesic effect,therefore, it is important in TAP block that the deposition of local anaesthetic occurs in the correct plane and the spread is visualised in real time.
Rectus sheath block
- Rectus sheath blocks provide analgesia for umbilical and other midline surgical incisions by blocking the terminal branches of the T9 to T11 intercostal nerves.
- The rectus sheath blocks have been successfully used for a variety of abdominal surgeries, including umbilical and inguinal hernia repair, laparoscopic cholecystectomy, laparoscopic appendectomy and pyloromyotomy.
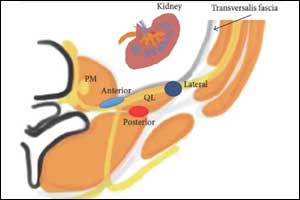
Quadratus lumborum block
- Quadratus lumborum QL blocks provide visceral analgesia due to more medial spread into lumbar paravertebral space.
- It is important to note that all patients receiving QL blocks are at risk of developing quadriceps weakness (and falls) secondary to blockade of lumbar plexus.
- Local anaesthetic deposited in the plane between the QL muscle and the medial layer of the thoracolumbar fascia can provide relief of somatic pain in the upper and lower abdomen.
- Due to the more dorsal injection point and potential spread to the paravertebral space, QL blocks can cover more extensive dermatomes for a significantly longer duration of analgesia as compared to TAP blocks.
Erector spinae plane block
- Erector spinae plane (ESP) block is an interfascial plane block that entails deposition of local anaesthetic deep to erector spinae muscle adjacent to transverse processes. A single injection of 20 ml of 0.5% ropivacaine at T5 level (3 cm from the midline) can result in sensory blockade from T3 to T9 over posterior thorax and T3 to T6 anterolateral thoracic area by blocking the ventral and dorsal rami of the thoracic spinal nerves.
- The most common indication is acute post-thoracotomy pain and chest wall trauma, but bilateral lower thoracic injection at T8 levels have been successfully used for the effective analgesia for open abdominal and bariatric surgeries.
- The efficacy of ESP block for incisional pain remains to be confirmed in larger clinical studies. Currently, very few case reports have been reported in the literature.
Regional anaesthesia for knee surgery: Adductor canal block
- Femoral nerve block (FNB) has become a common and highly effective method to control post-operative pain associated with total knee replacements . It also avoids risks associated with epidural anaesthesia and does not prohibit deep vein thrombosis prophylaxis.
- In recent years, the adductor canal block (ACB) has become an attractive alternative to FNB due to its quadriceps-sparing activity to facilitate early rehabilitation programme.
- Further studies are needed with a more standardised definition of site of the ACB, the current research suggests that ACB offers an improvement in quadriceps function compared to FNB with non-inferior pain control.
- In most patients for complete analgesia obturator nerve block should be considered.
- Surgeons often perform periarticular local infiltration intraoperatively with good results, avoiding the need for sciatic nerve block.[37]Alternatively, pre-operative ultrasound-guided injection of the capsule with 15-20 mL of long-acting local anaesthetic can be accomplished.
Long-Acting Local Anaesthetics
- The advent of long-acting local anaesthetics may provide an opportunity to decrease or even eliminate the use of nerve catheters.
- liposomal bupivacaine has been shown to increase the duration of action as well as decreased peak plasma concentrations compared to plain bupivacaine.
- It has been shown to significantly reduce pain in the first 72 h post-operatively, decrease opioid requirements and improve patient satisfaction compared to placebo in haemorrhoidectomy, bunionectomy, local infiltration analgesia of the knee and other surgical site infiltration.
- Liposomal bupivacaine is currently approved for local infiltration only.
Adjuvants to Regional Anaesthesia
- It not always feasible to send patients home with indwelling peripheral nerve catheters, there is still a need for methods to increase the duration of analgesia with single-shot peripheral nerve blocks.
Perineural dexamethasone
- Dexamethasone is believed to work by reducing release of inflammatory mediators and by inhibiting potassium channel-mediated discharge of C-fibres.
- A studies has shown that the dexamethasone-treated group had both a longer duration of sensory and motor blockade compared to control.
- Recent studies have examined whether intravenous dexamethasone provides similar block prolongation compared to perineural administration.Both dexamethasone groups showed statistically significant longer time to first toe movement compared to placebo, while only the perineural group showed a significantly longer analgesia duration.
Perineural dexmedetomidine
- Dexmedetomidine, an α2 agonist, which has eight times more affinity for α2 than α1(compared to clonidine)[43] can prolong sensory block. When compared with a placebo in posterior tibial block dexmedetomidine (1 μg/kg) showed a statistically significant increase in duration of sensory blockade in the dexmedetomidine group by a mean 5.3 h. However, the study group showed a statistically significant lower blood pressure starting at hour 1 and lasting until hour 8 after the block.
- Despite a number of studies that have shown no negative effects of perineural injection of dexmedetomidine, the IV route of administration is the only route approved by the FDA.
Evidence for Ultrasound-Guided Regional Anaesthesia
- Although it has not been shown that ultrasound meaningfully affects the incidence of peripheral nerve injury, the growing use of ultrasound technology in regional anaesthesia does have several possible advantages in comparison to nerve stimulator or landmark techniques.
- The use of ultrasound leads to faster sensory block onset, fewer vascular punctures, faster performance time and fewer needle passes in upper extremity blocks.
- In supraclavicular blocks, ultrasound guidance has decreased the frequency of pneumothorax though caution is still mandated during this procedure.
- UGRA also reduces but does not eliminate the incidence and severity of hemidiaphragmatic paresis through the use of decreased local anaesthetic volumes.
- In lower extremity blocks, ultrasound improves onset of sensory block and performance time.
- Importantly, registry data indicates that UGRA significantly reduces the incidence of local anaesthetic systemic toxicity by up to 65% compared to other nerve localisation methods.
- These safety implications may further encourage more anaesthesia practitioners to employ ultrasound technology in their practice.
Regional Anaesthesia and Cancer Recurrence
- Cancer recurrence and survival after primary surgery is impacted by a number of different factors, including the response of the immune system.A number of studies that show conflicting results with respect to superiority of use of regional anaesthesia versus opioid use in cancer recurrence rates.
- Various studies have been published evaluating the effect of regional anaesthesia on a number of different cancer types. In a recent systematic review and meta-analysis, a total of 20 studies were evaluated, and they found perioperative regional anaesthesia use was associated with improved overall survival but not with reduced cancer recurrence
Enhancing Safety in Regional Anaesthesia
Intraneural injection
- The controversial method of intraneural/intrafascicular injection to enhance onset and duration of block is generally not advisable because of potential neurotoxicity and consequent histological changes in peripheral nerves.
- Whether these changes result in clinical neurological deficit is not clearly understood. Histological nerve injury has been demonstrated when minimum stimulating current is <0.2 mA, but this does not reliably predict the distance of the needle tip from the nerve, and therefore may not confirm intraneural placement.
- Ultrasound guidance reveals nerve expansion predicting histologic injury when intraneural injection is placed; again this does not always translate to functional injury.
Injection pressure monitoring
- In order to mitigate the risk of nerve injury due to unintentional intrafascicular injection various safety techniques such as real-time visualisation by ultrasound guidance, stimulation technique and injection pressure monitoring device are used.
- The ideal method to enhance safety appears to be a combination of all the three methods.
- Although injection pressure monitoring devices are easily available and inexpensive, their widespread use is not observed in routine clinical practice.
The practice of regional anaesthesia has advanced rapidly in recent years with the application of ultrasonography resulting in significant improvement in quality of nerve blocks and patient satisfaction. Although adjuvants such as dexamethasone have shown prolongation of duration of block their widespread use in routine practice has not been observed. While regional anaesthesia is effective for the adequate management of acute pain, its beneficial effect on the development of chronic pain and cancer recurrence needs further research.
For further reference log on to :

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd