- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
CT Volumetry as good as Scintigraphy to predict outcome in Renal Donors : Dr. Niharika Prasad
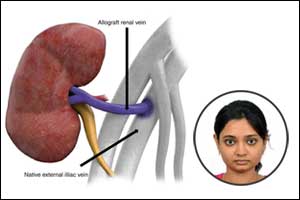
In recent times Computed Tomography (CT) Volumetry has been tried as an alternative to scintigraphy for the evaluation of pre-donation split renal function and the prediction of post-donation renal function in living kidney donors. Scintigraphy has been the traditional gold standard but is associated with few limitations.
Transplant donor’s kidney size is often cited as a predictive factor for recipient allograft function as well as donor kidney function. Recent studies have highlighted total kidney volume or cortical volume in living donor transplantation. Volumetry plays a role in determining the renal outcome in terms of kidney function (pre- and post-donation), longer-term estimated glomerular filtration rate (eGFR) decline, hypertension, proteinuria and cardiovascular events.
The concept of Volumetry has been previously described for liver transplantation such as virtual hepatectomy and residual volume calculation on computed tomography software. Its use in renal transplantation has been less described in the literature.
There are three methods for this-
- Total parenchymal three-dimensional renal volume (3DRV)
- Total parenchymal renal volume contouring (RVCt)
- Renal cortical volume (RCoV)
A study published in 2018 in the European Journal of Radiology showed a high correlation between renal cortical volume and pre and postoperative renal function in living kidney donors. Pre-donation kidney volume was measured in 105 donors using the above three methods. Automated software is used to estimate renal volume on different planes in three-dimensional method while only axial plane is used for the latter two. Scintigraphy was performed pre and post donation to measure glomerular filtration rate (mGFR). Authors concluded that ‘’cortical volumetry (RCoV) proved as best technique to use as a surrogate to scintigraphy for estimating pre-donation split renal function and predicting post-donation renal outcomes.” [1] They also claimed that this method can be used to predict subjects with an increased risk for developing chronic kidney disease after donation.
In a similar study in Germany by Halleck et al, it was found out that CT-based measurement of split cortex volume is a potentially useful tool to evaluate split renal function before donation. In 2015, a retrospective study on 75 patients concluded that preoperative renal volume can be a surrogate measure for radical nephrectomy-induced chronic kidney disease.
In another study in 2016, it was discovered that donors with the largest adjusted cortical volume were more likely to achieve an estimated glomerular filtration rate (eGFR) ≥60 mL/min/1.73 m2 over a median 24-month follow-up than those with smaller cortical volumes for a significant p-value. (<0.001) a sample of 85donors was taken in this prospective study. They followed up patients and their renal parameters over a longer postoperative period and found out that few factors need to be considered for the relationship of renal function prediction with Volumetry such as theinfluenceofageon outcomes according to kidney size groups. They concluded that kidney size corrected for BSA determined post-nephrectomy donor eGFR. Donors with larger cortical volume and length showed shorter recovery time and better function in the post-operative period.
The author is MD (Radiodiagnosis) and is Senior Resident, Dept of Radiology in All India Institute of Medical Sciences, AIIMS Patna. She is a member Editorial Board, Radiology at Specialty Medical Dialogues.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd