- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Contrast Ultrasound distinguishes gastric cancer from benign lesions
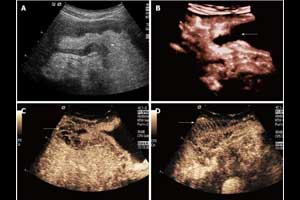
Gastrointestinal endoscopy and endoscopic ultrasound are the traditional methods used for evaluating gastric lesions, Lu said. The drawbacks of these techniques are that they are invasive. Conventional ultrasound might seem like a good solution, but it doesn't easily visualize these lesions. That's where the role of contrast ultrasound comes in. Dr.Man Lu, PhD, of the University of Electronic Science and Technology of China in Chengdu has presented a research at the American Institute of Ultrasound in Medicine (AIUM) meeting and shown that giving a double dose of ultrasound contrast in the form of both oral and injectable agents improves the modality's diagnostic performance for characterizing gastric lesions.
The technique, which Chinese researchers have dubbed double-contrast enhanced ultrasound (DCUS), combines CEUS enhancement characteristics with quantitative perfusion. It shows promise as a tool for distinguishing gastric cancer and gastrointestinal stromal tumors (GISTs) from benign lesions.
"[DCUS] uses an oral contrast agent to displace air, which produces distention and allows for clearer visualization of the multilayered echo pattern of the gastric wall," said presenter Dr. Man Lu, Ph.D., of the University of Electronic Science and Technology of China in Chengdu.
Benign from malignant
"CEUS offers real-time perfusion and provides a vascular characterization of lesions or organs of interest," Dr. Man Lu said.
She and colleagues wondered if adding DCUS could further improve the performance of CEUS in the task of characterizing gastric lesions. DCUS involves patients taking an oral contrast agent, which causes the ultrasound lumen to appear as a homogenous acoustic window, according to Lu. The patients are then given a second contrast dose, this time of an injectable agent.
The study included 107 patients with pathology-confirmed gastric lesions who underwent both DCUS and regular CEUS before surgery. The researchers analyzed a variety of perfusion parameters, including contrast arrival time, peak intensity, time to peak, and area under the curve (AUC) of the lesion and surrounding normal tissue. A reader blinded to pathology results rated and compared each case with surgical or resection biopsy pathology results.
Out of 107 gastric lesions, 75 were malignant (33 cancers and 42 GISTs) and 32 were benign (11 inflammatory masses and 21 polypoid adenomas).
Compared with regular CEUS, DCUS performed better across a range of measures, Lu said.
| Comparison of CEUS and DCUS in characterizing gastric lesions | ||
| CEUS | DCUS | |
| Sensitivity | 70.6% | 90.6% |
| Specificity | 62.5% | 75% |
| Positive predictive value | 81.5% | 89.5% |
| Negative predictive value | 47.6% | 77.4% |
| Overall accuracy | 68.2% | 85.9% |
Lu's team also found that malignant lesions had faster contrast arrival time and higher peak intensity and AUC than normal tissue in the DCUS exams. In addition, GIST and inflammatory masses had higher peak intensity than normal tissue.
Other results from the DCUS exams were as follows:
- Gastric cancers and GISTs had faster arrival time than polypoid adenomas.
- Inflammatory masses showed higher peak intensity than the other types of lesions.
- Gastric cancers had higher peak intensity than polypoid adenomas and GISTs.
- Gastric cancers and inflammatory masses had a larger area under the curve than polypoid adenomas and GISTs.
Adding DCUS to CEUS appears to overcome conventional ultrasound's limitations in characterizing gastric lesions, Lu said.
"DCUS improved diagnostic performance compared with [CEUS alone] and may be a useful method for evaluating the blood supply of gastric lesions to distinguish between those that are benign and those that are malignant," she concluded.

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd