- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Chronic Obstructive Pulmonary Disease- Standard Treatment Guidelines

COPD should be suspected in any person, particularly in middle life, with history of tobacco smoking and/or other risk factors, and presenting with:
- Cough, more during morning hours
- Frequent sputum production
- Breathlessness, mainly on exertion On clinical examination features of hyperinflation, diminished vesicular breath sounds with prolonged expiration and rhonchi are found.
Ministry of Health and Family Welfare, Government of India has issued the Standard Treatment Guidelines for Chronic Obstructive Pulmonary Disease (COPD). Following are the major recommendations :
Case definition:
For both situations of care (mentioned below*)
COPD is a preventable and treatable disease condition characterised by airflow limitation, which is not fully reversible. The airflow limitation is usually progressive and associated with an abnormal inflammatory response of the lung to noxious particles or gases, primarily caused by tobacco smoking. Chronic cough and sputum production often precede the development of airflow limitation by many years. Although COPD affects lung, it also produces significant systemic consequences. The diagnosis must be substantiated by quality spirometry showing post bronchodilator FEV1/FVC < 0.7 and FEV1 < 80% of predicted.
Incidence of The Condition In Our Country
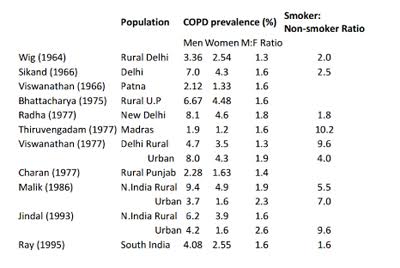
COPD is primarily a disease of the adults. The prevalence of COPD reported in different population based studies from India is highly variable (Table 1). The prevalence rates in male subjects of 2.12% to 9.4% in studies reported from North are generally higher than 1.4% to 4.08% reported from South India. The respective range for female subjects varies from 1.33% to 4.9% from North and from 2.55% to 2.7% from South India. For epidemiological assessment, the rounded-off median prevalence rates were assessed as 5 percent for male and 2.7 percent for female subjects of over 30 years of age. The disease is distinctly more common in males. The male to female ratio varies from 1.32:1 to 2.6:1 in different studies with a median ratio of 1.6:1. COPD results from chronic inhalational exposure to various smokes, noxious particles and gases.
Table 1. Prevalence of COPD and its smoking association in various population studies from India.
Differential Diagnosis
Chronic bronchial asthma, bronchiectasis, tuberculosis, obliterative bronchiolitis, congestive cardiac failure, dilated cardiomyopathy, diffuse panbronchiolitis.
Asthma is a major differential diagnosis. In some patients with chronic asthma, a clear distinction from COPD is not possible using current imaging and physiological testing techniques. The following features sometimes help in differentiating the two conditions.
| COPD | Asthma |
|
|
Prevention And Counseling
- Smoking cessation: Cessation of smoking is of fundamental importance to the successful management of all stages of COPD.
- Adequate measures to control environmental pollutants and provision of occupational hygiene in dusty working environment.
- Vaccines: COPD patients are particularly susceptible to influenza infection, thus annual influenza vaccination is recommended for all. Currently available vaccine pneumococcal vaccines (PPSV23) has not been shown to be effective particularly in high-risk patients. Trials are underway with pneumococcal conjugate vaccine [PCV-13 (CAPITA trail)] and further recommendations should wait till the outcomes of the trial are available.
- Health education about COPD: It is not a curable disease rather it is a preventable and treatable disease.
- Strict adherence to treatment i.e. use of inhaled bronchodilators, with or without other necessary pharmacologic treatment is essential.
- Prompt recognition of features of an exacerbation is of paramount importance, therefore, patients should be educated about warning signs and symptoms.
- Lifestyle modification and treatment of extrapulmonary manifestations such as coronary artery disease, osteoporosis, sarcopenia and anxiety/depression, and co-morbidities like type2 diabetes mellitus and metabolic syndrome.
Optimal Diagnostic Criteria, Investigation, Treatment & Referral Criteria
*Situation 1: At Secondary Hospital/ Non-Metro situation: Optimal Standards of Treatment in Situations where technology and resources are limited
Clinical Diagnosis:
Patients usually present with:
- History of tobacco use.
- Cough with or without sputum production. Cough is particularly worse in the morning and sputum production is a frequent complaint in the early stages of COPD.
- Dyspnoea on exertion: progressive breathlessness in COPD is a persistent symptom with waxing and waning but there is never any time when patients are entirely asymptomatic. Onset of breathlessness is insidious with progressive course, and often a significant amount of ventilatory capacity has been lost before the patient presents to the physician.
- Many patients complain of intermittent wheezing. However, nocturnal wheezing is uncommon in COPD and suggests diagnosis of asthma or heart failure. On clinical examination: patients are frequently seen sitting leaning forward with their arms resting on a stationary object. Some patients also develop pursed lip breathing. Percussion of chest is not very helpful in COPD (might reveal features of hyperinflation of lungs). Auscultation reveals diminished vesicular breath sounds with or without crackles and wheeze. Measurement of FET (forced expiratory time) is a valuable bedside technique to detect and assess airflow obstruction. An FET <5 seconds suggests that severe airflow limitation does not exist, whereas FET > 6 seconds indicates considerable airflow limitation. Many a times patients get disoriented, somnolent, or may complain of headache, which indirectly suggests CO2 retention. Such a situation will require the application of non-invasive ventilation (NIV), if possible at the treating centre. Peripheral edema, raised JVP, and hepatomegaly are signs indicative of pulmonary hypertension and right ventricular failure (chronic cor pulmonale).
Investigations:
- Spirometry is essential to firmly establish the diagnosis. Post bronchodilator FEV1/FVC <0.7 and post bronchodilator FEV1<80%, 50% or 30% predicted are used for purpose of spirometric classification of COPD according to GOLD.
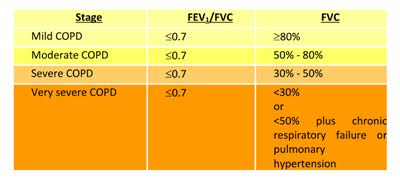
- Blood tests like haematocrit, chest radiograph (postero-anterior and lateral views) may be helpful in resource-poor settings.
- ECG and echocardiography (if available).
- 6-minute walk test.
Treatment:
The goals of COPD management include:
- Relief of symptoms
- Prevent disease progression
- Improve exercise tolerance
- Improve health status
- Prevent and treat extrapulmonary manifestations
- Prevent and treat complications
- Prevent and treat exacerbations
- Prevent or minimise side effects from treatment
- Reduce mortality
Standard Operating procedure
In Patient
Patients would present to the hospital in an exacerbation which is defined as an event in the natural course of the disease characterised by a change in the patient’s baseline dyspnoea, cough, and/or sputum that is beyond normal day-to-day variations, is acute in onset, and may warrant a change in regular medication. Signs of severity of an exacerbation that would require hospitalisation include: use of accessory muscles of respiration, paradoxical chest wall movements, cyanosis, peripheral oedema, haemodynamic instability, and decreased mental alertness. A chest X-ray would help in identifying alternative diagnoses that could mimic an exacerbation, while an ECG would aid in the diagnosis of right heart hypertrophy, arrhythmias and ischaemic episodes. Blood tests including haemogram, sugar and renal functions should be performed. Blood sample for ABG measurement should be drawn, if facility exists.
Management of exacerbations:
- Administer controlled oxygen therapy
- Repeated administration of bronchodilators (β2 agonists and anticholinergics). Increased doses may be required in some patients.
- Add oral or intravenous glucocorticoids
- Consider adding an i.v. methylxanthine, if needed
- Consider antibiotics when signs of bacterial infection
- Monitor fluid balance and nutrition
Out Patient
Stable COPD can be managed with therapy at each stage of COPD as follows:
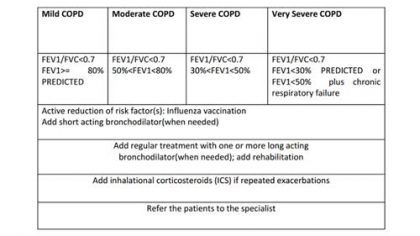
Antibiotics:
Antibiotics may be initiated in patients with altered sputum characteristics (increased volume and increased purulence) and increased dyspnoea. The choice should be based on local bacteria resistance patterns.
Referral criteria:
- Marked increase in intensity of symptoms
- Severe COPD
- Appearance of cyanosis, edema
- Signs of respiratory failure
- Significant co-morbidities
- Recurrent exacerbations
- New onset arrhythmias
- Diagnostic uncertainty
- Old age
- Failure to control exacerbation
*Situation 2: At Super Specialty Facility in Metro location where higher-end technology is available
Clinical Diagnosis:
Patients usually present with:
- History of tobacco use.
- Cough with or without sputum production. Cough is particularly worse in the morning and sputum production is a frequent complaint in the early stages of COPD.
- Dyspnoea on exertion: progressive breathlessness in COPD is a persistent symptom with waxing and waning but there is never any time when patients are entirely asymptomatic. Onset of breathlessness is insidious with progressive course, and often a significant amount of ventilatory capacity has been lost before the patient presents to the physician.
- Many patients complain of intermittent wheezing. However, nocturnal wheezing is uncommon in COPD and suggests diagnosis of asthma or heart failure. On clinical examination: patients are frequently seen sitting leaning forward with their arms resting on a stationary object. Some patients also develop pursed lip breathing. Percussion of chest is not very helpful in COPD (might reveal features of hyperinflation of lungs). Auscultation reveals diminished vesicular breath sounds with or without crackles and wheeze. Measurement of FET (forced expiratory time) is a valuable bedside technique to detect and assess airflow obstruction. An FET <5 seconds suggests that severe airflow limitation does not exist, whereas FET > 6 seconds indicates considerable airflow limitation. Many a times patients get disoriented, somnolent, or may complain of headache, which indirectly suggests CO2 retention. Such a situation will require the application of non-invasive ventilation (NIV), if possible at the treating centre. Peripheral edema, raised JVP, and hepatomegaly are signs indicative of pulmonary hypertension and right ventricular failure (chronic cor pulmonale).
Investigations:
- Same as in Situation 1 (b)
- Assessment of pulmonary haemodynamics
- CT-thorax and ventilation-perfusion scanning (especially for those being planned for lung surgery)
- Polysomnographic studies (if indicated)
- Cardiopulmonary exercise testing
- DEXA scan for osteoporosis [bone mineral density (BMD) and sarcopenia [fat free mass index (FFMI)]
- Psychiatric evaluation for anxiety/depression
- Alpha-1 antitrypsin deficiency screening (for those who develop COPD at a younger age and those with a strong family history of COPD).
Treatment:
not applicable
Standard Operating procedure
In Patient
- Same as in Situation 1 (c)
- Noninvasive ventilation using BiPAP
- Mechanical (invasive) ventilation
- Surgical options including bullectomy and LVRS
Indications for mechanical ventilation:
- Severe dyspnea, use of accessory muscles of respiration and paradoxical abdominal motion
- Severe acidosis pH< 7.25, and/or hypercapnia PaCO2> 60mmHg which does not respond to NIV
- Somnolence, impaired mental status
- Unable to tolerate NIV
- Life-threatening hypoxemia
- Respiratory rate > 35/min
- Impending respiratory arrest
Diagnosis and management of cor pulmonale
The patient develops chronic cor pulmonale when there are alterations in the structure and function of the right ventricle caused by a primary disorder of the respiratory system. Invariably this would manifest as pulmonary hypertension on echocardiography.
Symptoms would include tachypnoea and increase in exertional dyspnoea. Patients with chronic cor pulmonale and right heart failure will present with distended neck veins with prominent ‘V-y’ pattern suggestive of tricuspid regurgitation, cyanosis, peripheral oedema, splitting of second heart sound with accentuation of pulmonary component, left parasternal heave, long systolic or pansystolic murmur with accentuation during inspiration in the lower left sterna border, occasionally presence of right ventricular third heart sound, right upper quadrant abdominal discomfort and pulsatile hepatomegaly.
Medical therapy for chronic cor pulmonale is generally focused on treatment of the underlying pulmonary disease and improving oxygenation and right ventricular (RV) function by increasing RV contractility and decreasing pulmonary vasoconstriction.
In general, in patients with COPD, long-term oxygen therapy is recommended when the PaO2 is less than 55 mm Hg or the O2 saturation is less than 88%. However, in the presence of cor pulmonale or impaired mental or cognitive function, long-term oxygen therapy can be considered even if the PaO2 is greater than 55 mm Hg or the O2 saturation is greater than 88%. This must be documented in at least two consecutive ABGs done 3 weeks apart in stable state.
Pharmacotherapy includes salt restriction, diuretics, calcium channel blockers (indicated only if cardiac catheterization facilities available and vasoreactivity can be demonstrated), prostacyclin analogues (epoprostenol, treprostinil, and iloprost), endothelin-receptor antagonists (bosentan), PDE5 inhibitors (sildenafil and tadalafil).
The algorithms for correction of hypoxia and long term oxygen therapy are given below.
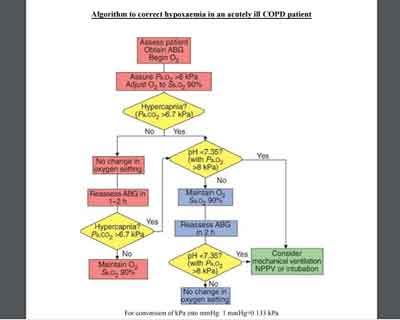
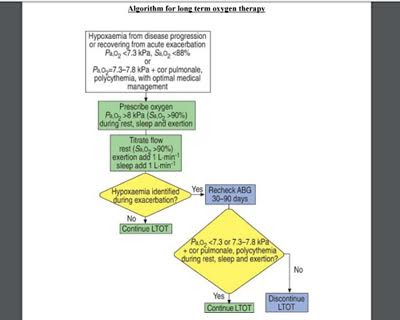
Out Patient
Same as in Situation 1
Referral criteria:
Patients with very severe COPD who are not controlled even on maximal medical therapy and LTOT and who fulfill the selection criteria for lung transplantation should be referred to a specialist centre where expertise of lung transplantation is available.
Who does what? and timeliness
Doctor:
Diagnosis and management including counseling
Nurse :
Implementation of orders and monitoring of patients
Technician:
Carrying out investigations
Resources Required For One Patient
| Situation | Human Resources | Investigations | Drugs & Consumables | Equipment |
| 1. | 1. Physician 2. Nurse 3. Laboratory technician 4. Pulmonary function test technician 5. Radiographer 6. Physician trained in ECHO/ cardiologist | 1. Chest radiograph 2. Hemogram 3. Pulmonary function tests 4. ABG 5.Eletrocardiogram 6 . 2D-ECHO | 1. Inhaled bronchodilators (salbutamol, ipratropium, tiotropium) 2. ICS (fluticasone/bude -sonide)+ LABA (formoterol/salmeterol) 3. Parenteral and oral bronchodilators (theophylline, terbutaline) 4. Parenteral and oral steroids (hydrocortisone, prednisolone) 5. Parenteral and oral antibiotics (Amoxycillin and clavulanate combination, cefadroxil, cefotaxime, Piperacillin and tazobactum combination) | 1.Oxygen cylinder/concentrator 2. Nebulizers (both electric and electronic) 3. Spirometer along with 6-MW facility 4. X-ray machine 5. ABG analyzer 6. EKG machine 7. Echocardiography machine |
| 2. | Above plus 1. ICU staff with pulmonary training 2. Physiotherapist 3. Sleep laboratory technician 4. Thoracic surgeon 5. Psychiatrist 6. Cardiologist 7. Radiologist 8. Anesthetist | Above plus 1. CT Scan 2.Polysomnography 3.DEXA scan | Above plus 1. Higher generation antibiotics | Above plus 1. CT machine 2. ICU set up 3. Noninvasive and invasive ventilators 4. Polysomnography machine 5. DEXA machine 6. Operation theatre with trained staff |
Guidelines by The Ministry of Health and Family Welfare :
Dr S.K. SHARMA AIIMS

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd