- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Case of Paget-Schroetter syndrome
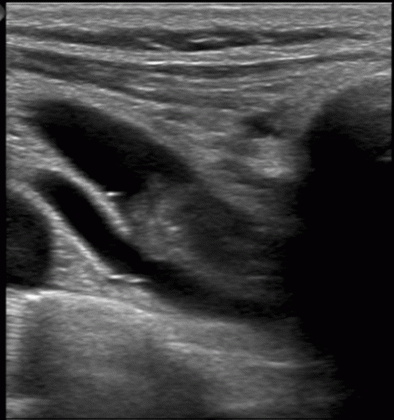
Paget-Schroetter syndrome is thrombosis of the axillary-subclavian vein that is associated with a strenuous and repetitive activity of the upper extremities. Due to overuse of the arm when coupled with external compression microtrauma in the intima of the subclavian vein results which results in the activation of the coagulation cascade.
The syndrome is predominantly witnessed among young healthy individuals.Diagnosis is usually made by Doppler ultrasound and the treatment involves thrombolysis, while routine surgical decompression of the thoracic outlet is controversial.
As history goes, a 21-year-old woman presented to the hospital for right lower neck pain whch started after she attempted to stretch backward. She also complained of pain and swelling over her right upper arm which started a day after the neck pain started. Her vitals were within normal limits and physical examination was positive for erythema, swelling, and tenderness in the upper right arm and right subclavicular region. Her CT angiography of the neck and CT of the cervical spine were unremarkable. Complete blood count and a complete metabolic panel were within normal range. Ultrasound venous of the right upper extremity showed a large echogenic thrombus of the right subclavian vein.
 Ultrasound venous of the right upper extremity showing large echogenic thrombus of the right subclavian vein which appears to be moving slightly during the examination.
Ultrasound venous of the right upper extremity showing large echogenic thrombus of the right subclavian vein which appears to be moving slightly during the examination.Given the above findings, further detailed history was obtained. The patient denied a family history of coagulation disorder. However, she admitted to being on oral contraceptive pills. Coagulation studies showed a normal protein S activity along with a negative factor V Leiden, anticardiolipin and prothrombin G20210A mutation. Antithrombin III level was slightly lower. The patient was subsequently placed on a heparin infusion and was scheduled to undergo thrombolysis. Venography performed before procedure via the right basilic vein which showed complete occlusion as the axillary vein and scant collateral vessels.
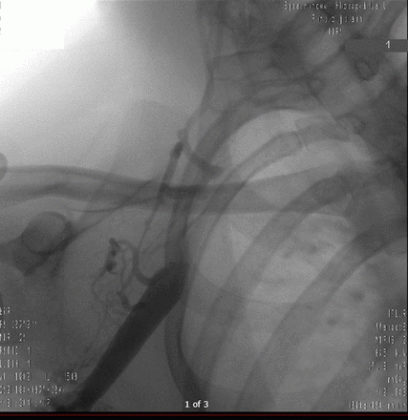 Venography of right upper extremity before procedure showing complete occlusion as the axillary vein entered the chest with scant collateral vessels.
Venography of right upper extremity before procedure showing complete occlusion as the axillary vein entered the chest with scant collateral vessels.The patient underwent intravenous catheter thrombolysis with 10 mg alteplase bolus continued with 1 mg/hour intravenous infusion for 24 hours without any complications. An interval venography which was performed after a day of the procedure demonstrated a reduction in the size of the subclavian thrombus but persistent large obstructing thrombus at the first rib. There was a residual 80% obstruction that correlated with the triangle formed by the scalene anterior muscle posterior to the subclavian vein, the first rib beneath the vein and the clavicle above the vein.
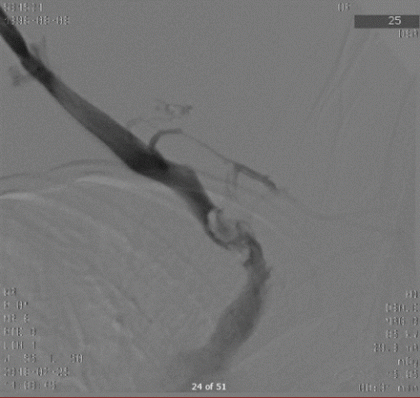 Venography of right upper extremity post intracatheter thrombolysis showing a large obstructing thrombus at the first rib with contrast flowing around it freely into the right atrium.
Venography of right upper extremity post intracatheter thrombolysis showing a large obstructing thrombus at the first rib with contrast flowing around it freely into the right atrium.The obstruction appeared to be complex indicative of possible residual fibrotic material or thrombus. An additional 2 mg alteplase intra catheter bolus was given an intravenous infusion of 1 mg/hour was restarted for another 24 hours. A 12 mm (length)×40 mm (diameter) balloon angioplasty with the pressure of 10 atm was later performed. Interval venography showed persistent 80% obstruction in the subclavian vein with good flow into a central venous system with no progression compared with the previous image findings.
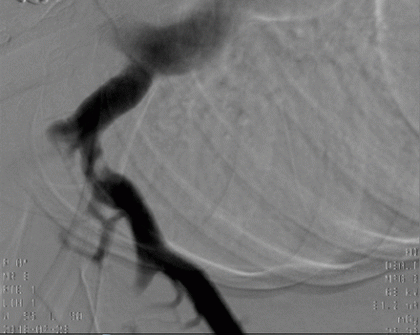 Venography of right upper extremity post second intra catheter thrombolysis and balloon angioplasty showing unchanged residual 80% obstruction with good flow into the central venous system.
Venography of right upper extremity post second intra catheter thrombolysis and balloon angioplasty showing unchanged residual 80% obstruction with good flow into the central venous system.No embolism following balloon angioplasty has been observed. The patient was discharged on rivaroxaban and was scheduled to undergo thoracic first rib resection in 3–4 weeks.
We considered hereditary hypercoagulability, thrombosis related to trauma or catheter placement, and thoracic outlet anatomic abnormalities (Paget-Schroetter syndrome) in our working differential diagnosis. The diagnosis of Paget-Schroetter syndrome was established given the nature of the presentation and negative hypercoagulability workup. Paget-Schroetter syndrome is characterized by primary spontaneous upper extremity deep vein thrombosis (DVT) usually due to anatomical abnormalities of the thoracic outlet with subsequent compression of the axillosubclavian vein. Various structural anomalies are known to cause thoracic outlet obstruction are hypertrophied muscles, cervical ribs, long transverse processes of the cervical spine, musculofascial bands and clavicular anomalies of the first rib.
Management goals are aimed at prevention of complications of venous thrombosis such as pulmonary embolism, recurrences and post-thrombotic symptoms. A minimum of 3 months of anticoagulation is recommended for all patients identified for upper-extremity DVT. For patients with moderate or severe symptoms, thrombolysis is recommended with the anticoagulation. Following thrombolysis, surgical decompression of thoracic outlet has been shown to lower rates of recurrent thrombosis and reduce long-term morbidity; however, the recommendations are very weak.
Carry home points :
The presentation of severe pain in the extremities among patients with known anatomic abnormalities should raise a high index of suspicion for Paget-Schroetter syndrome and should be worked up appropriately.
This upper extremity thrombotic event is usually preceded by strenuous exercise or repetitive movements of the upper extremity. However, there are a few case reports which mild activities could also trigger the event.
Thrombolysis is reserved for patients presenting with moderate to severe symptoms. Even though surgical decompression is known to lower rates of recurrent thrombosis and reduce long-term morbidity, the recommendation is weak since it is based on observational studies.
For further reference log on to : BMJ Case Reports2018; doi:10.1136/bcr-2018-227754

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd