- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Case of massive Splenomegaly-A report
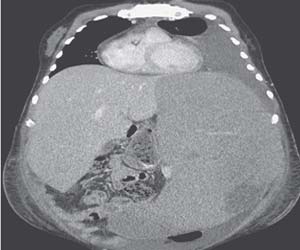
Dr Armin Rashidi, at the University of Minnesota, Minneapolis, MN and colleagues have reported a case of massive Splenomegaly. The case has appeared in the New England Journal of Medicine.
Massive splenomegaly is defined as weight of spleen >1,000 g or largest dimension >20 cm. It is usually reported in myeloproliferative disorders, lymphoma, leukemia, visceral leishmaniasis, tropical malaria and extrahepatic (noncirrhotic) portal hypertension. Splenomegaly is a common finding in a wide-spectrum of diseases. In a retrospective study, evaluating massive splenomegaly in 2,056 patients who presented to a large university medical center from 1913 to 1995, 31% had a hematologic disorder (lymphoma, leukemia), 17% had hepatic disease (noncirrhotic portal hypertension)and 8% had infectious disease (visceral leishmaniasis, tropical malaria). Massive splenomegaly is a rarely described feature of hepatic cirrhosis.
A 35-year-old man presented to the emergency department with a 3-week history of fatigue and painful distention of the left side of his abdomen. He had a history of hepatosplenic T-cell lymphoma and had completed treatment 9 months earlier. Physical examination revealed massive enlargement of the liver and spleen, with the spleen crossing the midline and its lower margin extending into the pelvis.
A computed tomographic scan of the abdomen confirmed hepatomegaly and splenomegaly (with the spleen measuring 36 cm in its greatest dimension). The white-cell count was 17,400 per cubic millimetre (reference range, 4000 to 11,000), the hemoglobin level 3.9 g per deciliter (reference range, 13.3 to 17.7), and the platelet count 10,000 per cubic millimetre (reference range, 150,000 to 450,000).
A blood smear showed atypical mononuclear cells, intermediate to large in size, with irregular nuclear contours, moderately fine chromatin, prominent nucleoli, and some cytoplasmic blebs. Relapsed hepatosplenic T-cell lymphoma was confirmed on flow cytometry. Other causes of massive splenomegaly include chronic myeloid leukemia, myelofibrosis, hairy-cell leukemia, malaria, β-thalassemia major, and visceral leishmaniasis. Treatment with immune checkpoint blockade and opioid analgesics was initiated, but the patient died consequent to disease progression 10 weeks after presentation.
For more details click on the link: DOI: 10.1056/NEJMicm1901064

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd