- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Case of isolated omental panniculitis presenting as intestinal obstruction
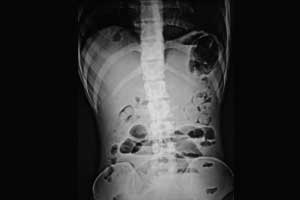
A case of isolated omental panniculitis presenting as intestinal obstruction has appeared in Formosan Journal of Surgery. Dr. Vipul D Yagnik at Department of Surgical Gastroenterology, Ronak Endo-Laparoscopy and General Surgical Hospital, Patan, Gujarat, India has reported the case.
Intra-abdominal panniculitis is a rare condition characterized by intraperitoneal lipodystrophy that may manifest as a necrotic adipose lump causing symptoms due to inflammation or mass effect. Although this condition tends to primarily affect the root of the mesentery, it may affect any part of the peritoneum, including the omentum. However, isolated omental panniculitis, in which no other site is affected, is a very rare form of intra-abdominal panniculitis and only eight cases have been reported in the literature so far. Mesenteric panniculitis, especially in the late fibrous stage of retractile mesenteritis, is known to occasionally cause intestinal obstruction by virtue of its relation to the bowel. However, omental panniculitis has only been reported to cause nonspecific inflammatory symptoms.
A 65-year-old male patient presented with abdominal pain and vomiting. He complained of abdominal distension and had not passed stools for the last 2 days. The pain was sudden onset severe colicky in the left upper abdominal quadrant and aggravated by movement. He had no significant past medical or surgical history notably similar type of abdominal pain, intra-abdominal malignancy, and abdominal surgery. Physical examination revealed a heart rate of 140/min and blood pressure of 80/50 mmHg. Abdominal examination revealed abdominal distension, tenderness in the left lumbar region, and a palpable lump in the left lumbar region.
“This case has a unique presentation which is not reported till date. Intraabdominal panniculitis is a rare condition and tends to affect mesentery primarily. Isolated involvement of omentum is exceptionally uncommon, and till date, only 8 cases reported in the literature with non-specific symptoms like abdominal pain, fever, malaise, and abdominal lump,” Dr. Vipul Yagnik, Consultant endoscopic and laparoscopic surgeon, Ronak Hospital, Patan told Medical Dialogues.
“A careful search of the English language literature did not reveal any report of isolated omental panniculitis presenting with intestinal obstruction. Histopathology will help in establishing a final tissue diagnosis. Treatment guidelines are not well formulated due to the rarity of the condition. Patients with non-obstructive symptoms might benefit from the medical management while those with unresolved obstruction or advanced inflammatory reaction necessitate laparotomy,” he added.
Laboratory investigations revealed leukocytosis (22,100/cu mm), an average random serum glucose (110 mg/dL), elevated serum creatinine (3.89 mg/dL), elevated erythrocyte sedimentation rate (55 mm/h), and increased C-reactive protein levels (110 mg/L). X-ray of the abdomen revealed small bowel obstruction. Abdominal ultrasonography was indeterminate due to the presence of excessive bowel gas. As the patient presented in sepsis with overt bowel obstruction, we suspected bowel strangulation or gangrene. We, therefore, decided against performing computed tomography (CT) abdomen as it would not change our decision for exploratory laparotomy and only add to the delay. After initial resuscitation, exploratory laparotomy was performed, which revealed a large omental lump 15 cm × 13 cm × 10 cm in size, which was adherent to the small bowel and had a yellowish and nodular external surface. The adjacent tissues were dissected without injuring the bowel.
Other abdominal organs were examined and found to be normal, notably the small bowel mesentery, pancreas, and sigmoid mesocolon. Histopathological examination of the mass revealed thick fibrous encapsulation; it was composed of lobules of adipose tissue separated by thick fibrous septae with congested and dilated blood vessels. A focal area of fat necrosis and xanthomatous inflammation was present at the periphery, with the collection of fat-laden macrophages consistent with omental panniculitis. We performed other investigations, such as antinuclear antibody, rheumatoid factor, lupus anticoagulant, and IgG-4, to determine the underlying cause, but all results were within normal limits. The postoperative course was unremarkable. The patient was discharged on the 7th postoperative day, and no problems were noted in a 4-month follow-up.
For more details click on the link: DOI: 10.4103/fjs.fjs_163_17

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd