- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Case of B-cell leukemia presented as inflammatory arthritis: JAPI Case Report
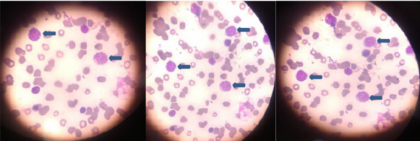
A case report published in the Journal of the Association of Physicians of India describes the case of a 17-year-old male patient resident of Bihar having B-cell acute lymphocytic leukemia (ALL) with pyrexia which was mistaken to be inflammatory arthritis.
The patient was presented with high-grade continuous fever, joint pains and weight loss since 1½ years. Joint pains involved large joints of all the limbs, migratory type, asymmetrical with nighttime exacerbations without any associated redness or swelling. With these complaints, he was diagnosed outside as a case of Juvenile Idiopathic Arthritis (JRA). Erythrocyte sedimentation rate (ESR) and C Reactive protein (CRP) were elevated but RF and ANA were negative. He has been receiving Disease-modifying anti-rheumatic drugs (DMARDs) and steroids with intermittent improvement in fever but the joint pains persisted. After investigations like Computed tomography scans, Ultrasonography, etc, he was started on empirical ATT for Pyrexia of unknown origin (PUO) based on the prevalence of Tuberculosis in our country and as the most common cause of PUO. Peripheral smear during all this time was normal except for pancytopenia.
On examination, he had severe pallor, hepatosplenomegaly and tender joints with no generalized lymphadenopathy. With these findings, we kept the differentials of Adult-onset still disease (AOSD), Lymphoma/Leukaemia, Kala Azar, Secondary Macrophage Activation Syndrome, and TB.

Peripheral smear showed pancytopenia. With these lab investigations, we also thought it to be a case of Adult Onset Stills Disease (AOSD) with Macrophage activation syndrome (MAS) and treated with DMARDs. But since the case was not completely fitting into AOSD criteria (Patient had leucopenia in contrast to expected leukocytosis) and previously treated on similar lines with no improvement and severe weight loss, anorexia,symptoms of joint pains out of proportion to signs with severe pancytopenia, organomegaly and elevated LDH , our suspicion for haematological malignancy was still high, so we did not start the patient on steroids.
A CECT chest and abdomen was performed which revealed hepatosplenomegaly with hypodense cortical lesions bilateral kidney. Multiple lytic/sclerotic lesions were present in pelvic bones, bilateral femur and multiple ribs. This radiological finding strengthened our suspicion for hematological malignancy. Bone marrow touch smear showed near total replacement by blasts which were MPO negative. The patient has completed the induction phase of treatment with oral Prednisolone (60 mg/m2), intravenous Vincristine (1.5 mg/m2), L-Asparaginase 10000 IU/m2 and is doing well. He is planned to be shifted on to the consolidation and maintenance phase.
"We presented here a case of B cell ALL which was for more than a year treated AOSD with steroids. So we would like to conclude by emphasizing that before labeling a patient as AOSD, a bone marrow examination is important in every patient presenting with atypical features of JIA and a normal peripheral smear to rule out an underlying hematological malignancy. Because the treatment of the condition with steroids might mask the diagnosis of an underlying hematological malignancy further delaying the diagnosis and later the malignancy may become steroid-resistant," write the authors.
For more details click on the link: www.japi.org

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd