- Home
- Editorial
- News
- Practice Guidelines
- Anesthesiology Guidelines
- Cancer Guidelines
- Cardiac Sciences Guidelines
- Critical Care Guidelines
- Dentistry Guidelines
- Dermatology Guidelines
- Diabetes and Endo Guidelines
- Diagnostics Guidelines
- ENT Guidelines
- Featured Practice Guidelines
- Gastroenterology Guidelines
- Geriatrics Guidelines
- Medicine Guidelines
- Nephrology Guidelines
- Neurosciences Guidelines
- Obs and Gynae Guidelines
- Ophthalmology Guidelines
- Orthopaedics Guidelines
- Paediatrics Guidelines
- Psychiatry Guidelines
- Pulmonology Guidelines
- Radiology Guidelines
- Surgery Guidelines
- Urology Guidelines
Case of Addison's disease mimicking anorexia nervosa
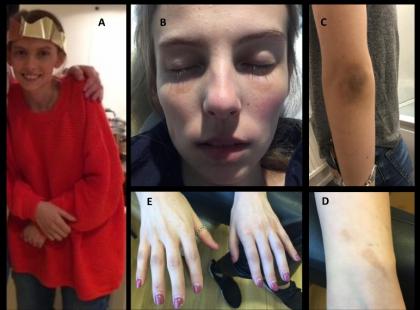
A case of Addison's disease mimicking anorexia nervosa has appeared in the American Journal of Medicine.Dr Claire Feeney at Department of Endocrinology, Imperial Healthcare NHS Trust, London, UK and colleagues have reported the case.
Addison's disease is an autoimmune adrenalitis that causes deficiencies in cortisol, aldosterone, and adrenal androgens. Patients commonly present with fatigue, anorexia, weight loss, and gastrointestinal disturbance.
The diagnosis of Addison's disease is often overlooked in investigations for weight loss and anorexia, especially in adolescents and young adults, in which other diagnoses, such as anorexia nervosa, are more common.
According to history, a 22-year-old woman presented to her physician with a history of unintentional weight loss of as much as 30 pounds.This was associated with nausea, vomiting, anorexia, and generalized abdominal pain. She also had symptoms of anxiety and low mood that coincided with relationship problems. She, however, did not report body image distortion or fear of weight gain, anorexia nervosa and depressive disorder were both strongly suspected.She was subjected to a trial of antidepressant therapy that was eventually stopped because her symptoms worsened. After one year she was diagnosed with primary hypothyroidism and levothyroxine replacement was commenced.
 Courtesy American Journal of Medicine
Courtesy American Journal of MedicineShortly after starting levothyroxine, she presented to the emergency department with syncope, weakness, and marked symptoms of postural hypotension that prevented her from standing up. On examination, she was cachectic, weighing only 77 pounds and measuring 5 feet 1 inch in height (body mass index, 14.5 kg/m2). She was in hemodynamic shock, with a blood pressure of 70/50 mm Hg and a pulse of 115 beats per minute. There was evidence of skin hyperpigmentation at multiple sites.
Her biochemical investigations demonstrated a normal sodium of 136 mmol/L (reference range, 133-146 mmol/L) and a normal potassium of 4.8 mmol/L (reference range, 3.5-5.3 mmol/L), and a random cortisol was low at 48 nmol/L (1.7 μg/dL). A diagnosis of adrenal insufficiency was made, and she was successfully resuscitated with intravenous fluids and intramuscular hydrocortisone treatment.
Prior to discharge, she underwent a short Synacthen test that confirmed primary adrenal insufficiency with a low basal cortisol of 34 nmol/L (1.2 μg/dL), 30-minute stimulated cortisol of 35 nmol/L (1.3 μg/dL), and markedly elevated adrenocorticotrophic hormone of 1992 ng/L (reference range, 0-47 ng/L).
Adrenal antibodies (21-hydroxylase) were positive, which confirmed a diagnosis of Addison's disease. She was discharged on oral hydrocortisone in combination with mineralocorticoid replacement. Six weeks later, her original symptoms had resolved and she had gained 13 pounds in weight (body mass index, 16.8 kg/m2). Six months later, her weight had returned to her baseline of 107 pounds.
Carry Home Points:-
- Addison's disease can be a challenging diagnosis that can be fatal. It shares some clinical features with anorexia nervosa, especially in young patients.
- However, health care providers can differentiate the conditions by taking a careful history; doing a thorough examination; and performing biochemical screening tests, such as tests for electrolytes, thyroid function, and early morning cortisol measurements.
- When in doubt, prompt referral to endocrinology services can provide diagnostic assistance in the case of young patients being investigated for weight loss.
For more details click on the link: DOI: https://doi.org/10.1016/j.amjmed.2018.06.027

Disclaimer: This site is primarily intended for healthcare professionals. Any content/information on this website does not replace the advice of medical and/or health professionals and should not be construed as medical/diagnostic advice/endorsement or prescription. Use of this site is subject to our terms of use, privacy policy, advertisement policy. © 2020 Minerva Medical Treatment Pvt Ltd